I’m occasionally stricken by a wave of crippling, all-consuming terror. Sometimes it’s because I can’t find my wallet. Sometimes it’s because I hear the unmistakable sound of Smitty throwing up on my bed. Sometimes it’s because I take a few wrong turns on Youtube and accidentally learn what Piccinini animal-human hybrids are (what is seen cannot be unseen). But these days, it’s usually because I’ve looked at the calendar and realized that—along with being 25 and really old now—I haven’t posted anything on this blog in almost four months.
What madness!
As most of you probably know, I’ve been chugging away on an upcoming book called “Death By Food Pyramid,” which is the main reason Raw Food SOS has been hosting more tumbleweeds than blog entries lately. Thanks to finding some unexpected political shenanigans to investigate (which I’m really excited to tell you guys about), the release date for “Death By Food Pyramid” is now September 2013. More details to come.
Earlier this month, I recorded an interview that touches upon the USDA’s seamy, pyramid-shaped underbelly (mostly in the second half):
I’ll be writing more about the book soon (and resuming my previous rapid-blogging schedule of six posts a year instead of four), but in the meantime, here’s a new installment of Bad Science Du Jour!
Are low-carb diets killing Sweden?
Last week, I wrote a guest post for Mark’s Daily Apple on a study that seemed to link Sweden’s “Low Carb High Fat” (LCHF) movement with an increased risk of heart disease. As often happens when media outlets are vying for readership, the headlines traded accuracy for alarmism—and it turned out the study had more to do with cheese-puffs and Justin Bieber than heart disease and carb restriction. You can read my breakdown of it here:
But it seems the Peer-Reviewing Powers That Be are smiling upon us this June, because Tuesday marked the arrival of yet another study on low-carbing Swedes—this one with a bit more meat on its bones. The BMJ paper (readable here until a paywall slurps it up) implied a grim future for carb-cutting ladyfolk. As Huffington Post UK reported (and you know they’re legit),
Women on Atkins-style diets are putting themselves at risk of heart disease and strokes, experts have warned. Those who regularly eat a low-carbohydrate, high-protein diet are at greater risk of cardiovascular disease than those who do not participate in such diets.
What’s the story, Wishbone? Do you think it’s worth a look?
This is a great study to tweeze apart for a few reasons, hence why it lured me out of blogging silence—but first, an important disclaimer:
I don’t think low-carb diets are universally flawless, especially if food quality isn’t emphasized—and if a long-term study emerges that shows legitimate concerns, I’ll be the first to tell you about it (or maybe the 10th, given my blogging speed). I deeply respect the success many folks have on low-carb regimens, and I have no doubt that this way of eating is often a lifesaver—sometimes quite literally—for folks facing obesity or certain health conditions, or who found themselves trapped in a low-fat-diet-hunger death spiral. At the same time, I think it’s clear by now that some people do well on the carbier end of the spectrum (myself included) and may run into problems on very-low-carb menus. And that’s okay! We’re all special snowflakes.
What I’m saying here is that I like to blog in defense of low carb not because I think it’s the holy grail of macronutrient ratios or the only healthy way to eat, but because it’s the bullied Poindexter of the diet world: no matter what its studies reveal, the media can’t help but punch it in the face, steal its lunch money, and drench it in buckets of pig blood à la Carrie. Few other diets receive such nasty—and generally unfounded—backlash. If we’re gonna embrace this whole “science” thing, we need to fight hard for objectivity wherever it may be lacking. En garde, y’all!
That said, I’ll spoil this study’s ending right off the bat and say that 1) it was observational and 2) it didn’t actually follow low-carbers. Yes, double whammy of ughness. We could technically stop right there and turn our thoughts to more important matters, like why traumatizing things exist on the internet (Piccinini hybrids, I’m looking at you), but I think that’d be a missed opportunity. This is actually a valuable study to analyze because it uses a “diet score” design that’s quite popular—and becoming ever more so—with observational health research. (I blogged about one such study in 2010, but there exists a wealth of other diet-score studies floating in the research sea, woefully undissected.)
Thusly, understanding this week’s study will help us understand the future ones—inevitably incubating in some researcher’s mind as we speak—that will one day hit the news with the same design, the same conclusions, and the same slew of limitations.
(Note before we kick things off: the following who-knows-how-many paragraphs are excruciatingly exhaustive, probably more than they need to be. My goal is to explain the details of this study in a way that makes this dissection relevant for future studies of a similar design. If you just want a summary of why the study is bad instead of my long-winded breakdown (no offense taken!), check out the study’s comment section on the BMJ website, where readers have pointed out many of the paper’s flaws in fewer words than I’ll be using.)
The design… of doom
In the early ’90s, about 50,000 Swedish females—all between the ages of 30 and 49—filled out a diet-and-lifestyle survey as part of the Women’s Lifestyle and Health Cohort. The women self-reported (by memory) everything they’d eaten during the past six months, answered some lifestyle questions, mailed their survey back to the project leaders, and then went on their merry way. This was the only time women reported their food intake during the entire 16-year study.
After kicking some ladies off the data-island because their questionnaires were incomplete (or because they entered the study already diagnosed with cardiovascular disease), our researchers were left with 44,000 participants. They translated each woman’s food-frequency responses into daily intakes for protein, carbohydrate, fat, and total calories, and then arranged that new macronutrient data into deciles—10 equal groups divided at the 10th percentile of intake, 20th percentile, 30th percentile, 40th percentile, and so forth. In the case of protein, for example, the first decile would include data from women with the very lowest intakes of protein, while the 10th decile would include data from women with the very highest intakes of protein. (Another way to look at it, since this system is based on tens: if a woman falls in the first decile for protein, nine deciles’ worth of women—or 90% of the study population—are eating more protein than her. If a woman falls in the 6th decile for protein, only four deciles—or 40% of the population—are eating more protein than her.)
Lather, rinse, and repeat this decile system for carbohydrate intake, fat intake, and total calorie intake.
Isn’t math grand?
But we’re just getting started. Here’s where the “diet score” stuff enters the scene.
Diet patterns: the easiest way for a scientist to score
In order to extort information about low-carb diets from a non-low-carbing population (an ambitious feat, to say the least), the researchers created a “low carbohydrate, high protein” diet score, and assigned points to each woman based on which carbohydrate and protein deciles she landed in. For protein, women would get one point if they were in the first decile; two points if they were in the second decile; three points if they were in the third decile—all the way up to 10 points for falling in the 10th decile. The point-assigning system was inverse for carbohydrate: women would get 10 points if they were in the first decile, nine points in the second decile, eight points in the third decile—on and on—and one point if they were in the 10th decile.
Once those calculations were made, the researchers tallied up each woman’s protein points and carbohydrate points for her combined “low carbohydrate, high protein” score, which could range from 2 to 20.
The purpose of that score was to gauge how closely each woman’s diet resembled the low-carb, high-protein eating pattern the researchers wanted to study. Women with the lowest scores were the furthest away from that pattern; women with the highest scores were, rightly or wrongly, judged to be Atkins fangirls. Some score examples could go like this:
Woman eating lots of fruits, vegetables, and grains, but very little animal food (i.e. Campbell’s future BFF): 1st decile for protein, 10th decile for carbohydrate = 1 + 1 = score of 2
Woman eating lots of lean meats, skim milk, very little fat, and moderate grains and potatoes: 5th decile for protein, 4th decile for carbohydrate = 5 + 7 = score of 12
Woman eating a very low-carb, low-protein diet with abundant fats, organ meats, butter, and cream: 1st decile for carbohydrate, 2nd decile for protein = 10 + 2 = score of 12
Woman eating a very low-carb, high-protein diet with lean meats, egg whites, fish, and protein powder: 1st decile for carbohydrate, 10th decile for protein = 10 + 10 = score of 20
(If you spot the problem here, fear not—we’ll come back to this in a moment!)
Armed with their meticulously-calculated diet scores, the researchers embarked on their next mission: to see which women received a “cardiovascular disease” diagnosis between 1991 and the end of 2007, and—the study’s crux—how their diet in ’91 influenced their health over the next 16 years.
At last, the moment of truth.
After running a battery of sophisticated analyses—looking at cardiovascular disease both collectively and in subcategories, and adjusting for common confounders like smoking, body mass index, education, and exercise—the researchers found the same thing most studies of this kind uncover: that women with the highest “low carb, high protein” scores had a higher incidence of cardiovascular disease than women with the lowest scores.
Straight from the paper (emphasis mine):
We found that women had a statistically significant 5% increase in the incidence of cardiovascular events per 2 unit increase in the 20 unit low carbohydrate-high protein score. In practical terms, and taking into account the rough correspondence in the ranking of energy adjusted and crude tenths of intake, a 20 g decrease in daily carbohydrate intake and a 5 g increase in daily protein intake would correspond to a 5% increase in the overall risk of cardiovascular disease.
Although a 5% risk increase might not sound like much at first, keep in mind that it applies to each 20-gram decrease in carbohydrate intake—supposedly adding up to a much bigger risk for true low-carb adherents. No wonder the media gobbled this one up!
Alas, this study is the last place to look for anything informative about low-carbohydrate diets—or really any diets, for that matter. Although the researchers did a commendable job analyzing the data they had, the rest of this study is a hot mess of defects. You’ve probably spotted some of them already, but a few important problems are tucked out of immediate sight. And we’re about to blow them all open.
Let’s start at the very beginning: the Swedish diet survey from the early ’90s.
Food frequency questionnaires… of doom
If you haven’t read my Will Eating Red Meat Kill You? guest post on Mark’s Daily Apple from a few months ago (which I can’t hold against you, since I never posted the link!), I recommend hopping over there right now to skim the section on food frequency questionnaires. (If two long blog posts are too much Denise for one day, check out this classic piece by Chris Masterjohn on the unreliability of self-reported data instead.)
The bottom line—discussed more thoroughly in those aforementioned links—is that bad things happen when you ask people to report what they eat. That badness only amplifies when they’re reporting from memory, and becomes incrementally worse the further back in time you want them to recall. Most folks just aren’t that aware of what goes in their mouths, especially when those things went in their mouths six months ago. As a result, nearly everyone underestimates what they really consume, and some foods—usually the ones we think are bad for us—tend to be a major roulette-wheel spin in terms of accurate reporting. Health-conscious folk may be particularly likely to underreport their intake of “bad” foods out of sheer guilt (who wants those Saturday brownie binges emblazoned forever on paper?). And since not everyone misreports their food intake in a consistent way, no amount of statistical wand-waving can really make up for the inaccuracies in this type of data.
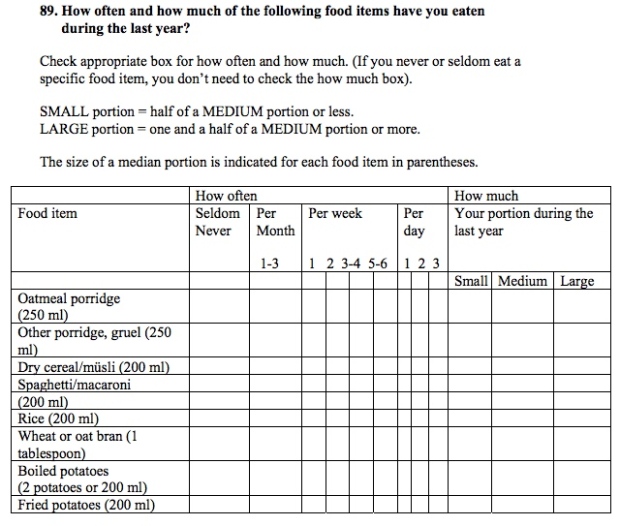
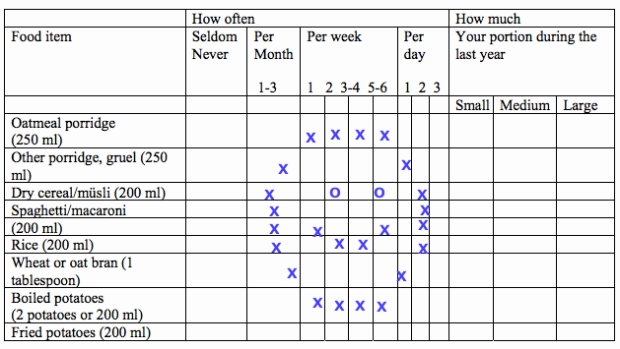
And if that hasn’t convinced you of food questionnaires’ inherent dodginess, maybe this will. Here’s the actual survey those 44,000 women of this study had to fill out in the early ’90s, when they first enrolled in the Women’s Lifestyle and Health Cohort. The diet questions start on page 13.
Here’s a prime example of the torture contained within:
And that’s only the first page. The full table includes 49 more items, just in case the ones above were too easy. I have to wonder how many people saw this questionnaire and were like,
And then filled it out like,
My guess is more than a few.
Indeed, the data from this survey seems pretty sketchy—both in terms of accuracy and in terms of being anything even remotely usable for “low carb” research. Even the validation study for the questionnaire, which was conducted to test how well the self-reported data matched direct diet records (where participants actually weighed and recorded their food each day), notes that refined grains, sweets, cooked and fried potatoes, vegetables, processed meat, poultry, fruit, and whole grains were over- or under-reported by at least 20%!
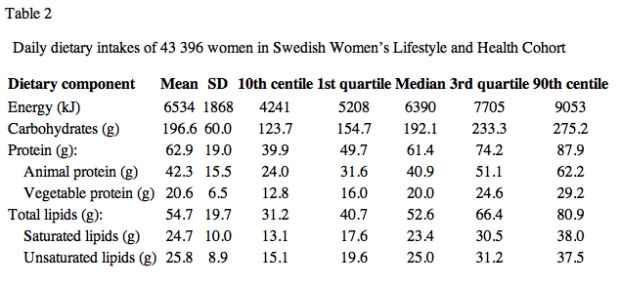
To illustrate the problem further, this table summarizes the diet data for the women in our current study:
Check out that calorie range! Based on the researchers’ translations of the survey data into dietary intakes, the women were eating 4241 kJ (only 1013 calories!) in the 10th percentile and 9053 kJ (2162 calories) in the 90th percentile. Think about that 1000-calories-a-day figure. Were thousands of ladies inexplicably eating starvation-level diets for months on end? Or were they, perhaps, just doing an unsurprisingly poor job of remembering how many broccoli florets, almonds, and tablespoons of salad dressing they’d eaten in the past year?
I’ll let you be the judge.
Equally damning is the data for macronutrients. The cutoff for the first decile of carbohydrate intake (the column marked “10th centile” in this table) is 123.7 grams a day—moderate carb at best, and far higher than most legitimately low-carb eating plans allow. Yet this, ladies and gentlemen, is the decile representing the lowest of the low carbers in our study. Women eating up to 123.7 g of carbohydrate per day received the full 10 “low carb” points when the researchers tallied up their scores. And since many women whose carbohydrate intake landed in the first decile are probably the same ones allegedly eating only 1000 calories a day, their true carbohydrate intake is likely much higher, making this already-not-a-low-carb-study even more so.
Macronutrient warz… of doom
By now, you’ve probably noticed one of this study’s many quirks: the researchers assume that carbohydrates and protein are hinged together on some sort of macronutrient seesaw—where reducing carb intake automatically means increasing protein intake, and vice versa. Although some low-carb plans do emphasize protein, it’s far more common for fat to be the nutrient that fills the calorie void when carbs go down, with protein changing to a much lesser degree. That’s because the vast majority of foods are either carbohydrate dominant (like grains, fruits, and starchy vegetables) or packed with plenty of fat (like meat, non-adulterated dairy products, and nuts), with relatively few whole foods—mostly shellfish and some non-fatty fish—being straight-up protein bombs. Unless you go wild with egg whites and protein powder and don’t mind meals that taste like nothing, it’s pretty hard to raise your protein intake particularly high, at least relative to fat and carbohydrate.
So why did the researchers fixate on a low-carb, high-protein diet score instead of a low-carb, high-fat one? Your guess is as good as mine. Perplexingly, they write in their paper that “The most popular among [weight-loss] diets emphasise reduction of carbohydrate intake, thereby encouraging high protein intake, as high fat diets are generally avoided in most Western societies.” Seems fair enough. But the paper they cite for that statement starts off by describing low carb as unabashedly fat-full:
The diet claims to be effective at producing weight loss despite ad-libitum consumption of fatty meat, butter, and other high-fat dairy products, restricting only the intake of carbohydrates to under 30 g a day.
It’s a head scratcher, that one.
As it stands, in this study, a true low-carbing woman with a moderate protein intake would only get a midrange score—and could easily end up with the same number of points as someone eating lots of carbs but also lots of protein. The bizarre “low carb, high protein” scoring system ultimately does a poor job of identifying any true low carbers in the cohort.
And best of all: towards the end of their paper, the authors eventually acknowledge that the “low carb, high fat” diet pattern in this study was a far cry from what actual low-carb programs promote (emphasis mine… as always):
Among the women studied, carbohydrate intake at the low extreme of the distribution was higher and protein intake at the high extreme of the distribution was lower than the respective intakes prescribed by many weight control diets. However, the underlying trend between low carbohydrate-high protein score and incidence of cardiovascular disease was essentially monotonic, indicating that our findings are applicable across the spectrum of carbohydrate and protein intakes of the participating women.
Translation: “We realize our low-carb study wasn’t actually a low-carb study, but let’s not let that prevent us from using it as evidence that eating low carb is bad.”
What about fat? Could that be the real reason the lowest-carb women got more heart disease?
Now here’s where things get interesting.
In the paper’s Results section, we see a brief (but important) note about fat: “The additive low carbohydrate-high protein score was … positively correlated with lipid intake (Spearman r=0.28 for saturated lipids; Spearman r=0.17 for unsaturated lipids)”—which means that as women progressed upwards on the low-carb, high-protein scale, their intake of fat was generally going up too. No brainer, considering high-protein foods often have plenty of fat.
But the researchers were apparently so committed to making this study only about low-carb, high-protein diets that they did something quite surprising: they designed their statistical models to adjust for both saturated and unsaturated fat intake (in the same way they adjusted for smoking, BMI, and so forth), to completely remove the influence of all things lipid! In other words, the results of this study can’t arguably be linked to any form of dietary fat, because the researchers statistically removed its effects. Whatever was driving the women’s cardiovascular disease risk was decidedly non-greasy.
Presumably, the researchers figured saturated fat would contribute to cardiovascular disease and thus treated it as a confounder. But since saturated fat is—at least by mainstream wisdom—deemed a major reason for the unhealthfulness of low-carb diets, it seems odd that the researchers totally removed it from the equation. What’s left to take the blame for the increased cardiovascular disease? The lowness of the carbohydrates? The highness of the protein?
The researchers offer a pretty standard explanation:
With respect to the biomedical plausibility of our findings, vegetables, fruits, cereals, and legumes, which have been found in several studies to be core components of healthy dietary patterns, are important sources of carbohydrates, so that reduced intake of these food groups is likely to have adverse effects on cardiovascular health.
(I probably don’t need to point out the obvious—that many low carbers end up eating more vegetables than their non-dieting peers, and that no heart-healthy nutrient exists in grains that can’t be obtained elsewhere—but given that the lowest low carbers in this study were still eating up to 123 grams of carbohydrate a day (and likely much more due to underreporting), I doubt they were suffering en masse from a grain-and-legume deficiency.)
Incidence rate ratio… of non-doom
Now that we’ve determined that this study 1) draws on terribly unreliable self-reported data, 2) doesn’t examine diets in a genuine low-carb threshold, and 3) has nothing to do with saturated fat, let’s take a look at just how risky the “low carb, high protein” pattern really was for cardiovascular health.
The researchers—and the media outlets that reported on this study—describe the results as showing that for every 20-gram decrease of carbohydrate intake (and every 5-gram increase in protein), the women’s cardiovascular disease risk rose by 5%. Less publicized was that when the researchers used women with a “low carbohydrate, high protein” score of six or less as their baseline, they found that women with scores above 16 had an incidence rate ratio of 1.60—or a 60% increase in risk compared to their carb-loving, protein-shunning counterparts.
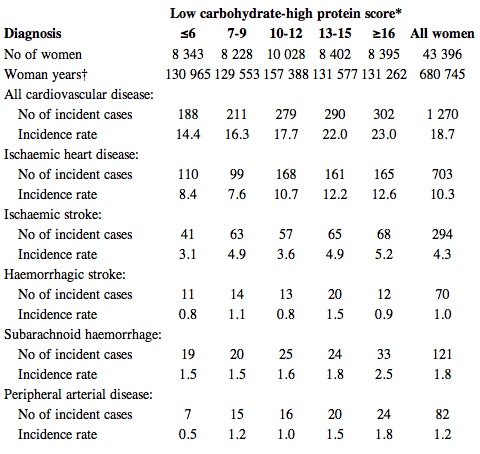
But numbers are a tricky, sneaky thing when they’re relative. Here’s a table showing the actual quantity of cardiovascular disease diagnoses for various score categories (the “incidence rate” is per 10,000 woman years):
Let’s focus on that All cardiovascular disease category. The researchers note that “potential confounding influences have not been accounted for” in this table, so the incidence numbers—especially in the highest- and lowest-point categories—are likely reflecting influences other than diet. But we’ll let that slide for now.
From this table, we can see that for women with a score of six or less, 2.2%—or 22 out of every 1000—were diagnosed with cardiovascular disease during the course of the study (188 incident cases divided by 8343 women). For women with a score of 16 or higher, 3.6%—or 36 out of every 1000—were diagnosed with cardiovascular disease (302 incident cases divided by 8395 women). That’s an absolute increase of only 1.4%, even though it represents a scarier-sounding relative increase of about 60%. And considering the 1.4% is a confounder-riddled value likely to over-represent the actual difference, that number becomes even less impressive.
But that’s not all. Let’s look again at the incidence rate ratios the researchers (and beloved media) gave us earlier: 1.05 for every two-point increase in the “low carb, high protein” score (or for every 20-gram drop in carbohydrate intake/5-gram rise in protein intake). Is that really a noteworthy ratio?
Lo and behold, the researchers help us answer that very question. In a table too unwieldy to capture in a screenshot, they list the incidence rate ratios (age-adjusted) for all cardiovascular disease diagnoses, based on a variety of characteristics unrelated to food:
- Being a current smoker (versus no smoking history): 2.78 — a 178% risk increase
- Having a body mass index in the “obese” range (versus in the normal range): 2.48 — a 148% risk increase
- Having a body mass index in the “underweight” range (versus the normal range): 2.17 — a 117% risk increase
- Having a hypertension diagnosis (versus no hypertension): 2.50 — a 150% risk increase
- Having the highest self-rated level of physical activity (versus the lowest): 0.37 — a 63% risk decrease
- Having over 13 years of education (versus 10 or less): 0.45 — a 55% risk decrease
- Being over 170 cm in height (67 inches, or 5’7″) (versus being 160 cm/63 inches or under): 0.77 — a 23% risk decrease
Compared with things like going to school for a few extra years and not being vertically challenged, the risk associated with the “low carb, high protein” diet score is minuscule!
But frankly, it hardly matters anyway. All these numbers are based on a single survey from 1991 – ’92, with absolutely no follow-up questionnaires to see if the women’s diets or lifestyles changed afterwards. This whole study rests on the assumption that 44,000 women not only accurately reported their yearly food intake in the early ’90s, but that they kept eating, exercising, and weighing the same for the next 16 years. (Or conversely, that whatever they ate in 1991 singlehandedly determined the fate of their health for the rest of their lives.)
To sum it all up…
- This study is observational—meaning it tells us nothing about cause and effect.
- This study relies on one food frequency questionnaire that the women filled out upon enrollment in the Women’s Lifestyle and Health Cohort. We have no idea what they were eating during the next 16 years.
- Women reported their food intake during the early ’90s, when low-fat diets were the gold standard for healthy eating. The most health-conscious women were likely to be eating the most carbohydrate at that time.
- Food frequency questionnaires are all sorts of terrible and don’t let anyone ever tell you otherwise.
- The study’s “diet score” design assumes that all low-carbohydrate diets are necessarily high in protein—resulting in a point-assigning system that doesn’t always identify true low carbers.
- The women with the lowest carbohydrate intake in this study were still eating up to 123 grams of it a day (an amount that’s probably wildly underestimated, to boot)—meaning they weren’t actually eating a low-carbohydrate diet.
- The true increase in cardiovascular disease risk from scoring high on the “low carb, high protein” scale is pretty minor—and pales in comparison to other lifestyle variables.
That’s it!
If your eyes are glazing over and all you care about is this blog entry being over, just remember this one thing:
Good math can’t make up for bad data.
This applies to every single study in the whole world that relies on food frequency questionnaires. These studies are not your friends. It doesn’t matter whether they yield results that make you feel better about your chosen lifestyle or worse for it—they’re all built on shaky ground, and not even the finest statisticians can change that fact. In order to have reliable results, a study needs reliable data. And for the most part, food-questionnaire-dependent studies are not the place to find it.
Likewise, any type of “diet score” study using data from the general population will suffer from one fatal flaw: these studies try to squeeze information about specific, clearly defined diets from people who—by and large—don’t actually eat those diets. It’s sort of the nutritional equivalent of flying to Paraguay to study Greek architecture. The reason this type of study design is popular isn’t because it has many redeeming qualities, but because it’s a heck of a lot easier (and cheaper!) to fiddle around with pre-existing data from large cohorts than to run controlled experiments where you make people do what you want them to do.
So basically, this study tells us nothing about nothing. Most other studies like it also tell us nothing about nothing. What does that leave us with?
Something like this, I’d say:
Although observational studies are a bucket of fun to peel apart, they’re also the sitting ducks of the research world—easy targets, limited by design, and utterly feeble behind their smokescreens of media hype. There’s only so much you can do with ’em before the study-dissection process becomes redundant and you start feeling bad about attacking something too incapacitated to fight back. When I’m back here blogging more regularly, I’ll be covering a great many topics other than observational studies—I promise!
…What, you thought this was over? I’m not letting you go that easy!
What follows is an assortment of things that don’t really deserve their own blog posts but that I want to mention somewhere, so I’m just going to tack them awkwardly onto the end of this entry and hope you guys don’t notice how weird it is.
1. For anyone who hasn’t seen it yet, I added a “For Vegans” page at the top navigation bar with some health tips for committed vegans. Link here:
2. A few months ago, I wrote a summary of the major flaws in “The China Study”—mostly based on my Wise Traditions presentation from last year—that you can read here:
3. For organizational purposes, here are my two most recent guest posts at Mark’s Daily Apple that I forgot to link to from this blog:
4. Are raw vegans immortal? Once in a while, I like to peruse the search-terms page on WordPress to see how wayfaring Googlers find my blog. After the standard pileup of “China Study” and “Forks Over Knives” phrases and various creative spellings of my name, things start getting weird. This came up not too long ago:
And then there’s tons of this:
Although I can’t honestly say I know why someone “loves popcorn craves” (or what that even means), I can say that vegans do get cancer, and raw vegans definitely die. Sometimes from cancer, no less. I think the general vegan community is pretty realistic about the fact that becoming a vegan—even the junk-food-shunning, non-smoking, non-drinking, non-drugging, non-rabid-honeybadger-owning variety—isn’t the same as putting on an invincibility cloak and forever evading disease, but raw vegans often have more confidence in their eternal immunity, which I find concerning. Case in point: the responses to this post from 30 Bananas a Day.
At any rate, the can-vegans-get-cancer question seems to be the most common of the bunch, and I’m not surprised. I’ll wager that “The China Study,” especially Campbell’s research with casein, has left some folks with the impression that—even if you’re exposed to a nasty carcinogen like aflatoxin—cancer can only happen if you’re eating enough animal protein to feed it. Raw vegans often feel they’ve got added protection because they’re eating nothing but quintessential health foods.
At the risk of being kind of morbid, I want to put up a list of some really-long-term raw vegans (and a few non-raw ones) who got diseases they weren’t supposed to get. I don’t think this is common knowledge—I’ve only gathered this list piecemeal from hanging out in the vegan gossip stream for much of my past—so here it is for the rest of the world to see.
- Bif Naked—award-winning musician and actress—was a raw vegan for 10 years before getting diagnosed with breast cancer.
- Ross Horne, famous Natural Hygienist and author of a book called “Cancer-Proof Your Body,” died of prostate cancer in 2004—after 22 years of eating a high-fruit, raw vegan diet in the tropics. (Although the previous link says he died “well into his 80s,” his actual age at death was plain ol’ 80.)
- Harvey Milstein—leader of the raw vegan “natural hygiene” movement in Houston, Texas—died of colon cancer in his 60s after 23 years as a fruit-based raw vegan.
- Vihara Youkta, dancer and wife of famous raw foodist Viktoras Kulvinskas, died of bowel cancer after being raw vegan for 30 years.
- More recently, Robin Gibb of Bee Gees fame died of colon cancer at the age of 62, after being a drug-and-alcohol-abstaining vegan for decades (cooked, not raw).
- T.C. Fry—fruitarian and early raw vegan pioneer—died of a coronary embolism when he was about 70, and his autopsy revealed additional blood clots in his legs. (Joel Fuhrman notes that Fry’s B-12 levels were extremely low before his death, so he probably had high homocysteine, which makes blood more prone to clotting.)
- And on the cooked side of things, we’ve got H. Jay Dinshah—the founder and former president of the American Vegan Society—who died at age 66 of a heart attack. He was a vegetarian from birth and vegan for his final 43 years of life. (Here’s an excellent write-up about the implications of his death by Michael Klaper.)
There are definitely some long-lived cooked vegans (like Donald Watson, who invented the word “vegan,” remained one for 60 years, and died peacefully at the age of 95). But so far, raw veganism has had a less-than-impressive track record for longevity. The raw foodists who’ve made it into old age in good health typically included some animal products. Fifty-year raw foodist Norman Walker—who lived to be 99 (despite rumors of a supercentenarian status)—used goat’s milk, raw cream, and cottage cheese. Bernando LaPallo, a still-living 109-year-old, mostly-raw foodist from Arizona, eats fish along with his fresh fruits and veggies.
Hopefully people who google “can vegans get cancer?” will now find this page.
Now I’ll let you guys go. Here’s a picture of some baby hedgehogs so we end on a happier note.






Thanks for posting this. I’m sick and tired of the vegans and agricultural corporations, in any country, butchering science to support their own agenda. (Yes, I happen to be one of those people who only does well on the lower end of the carb spectrum, so the constant lies and misinformation never ceases to piss me off.)
Can’t wait for your book! 2013 never seemed farther away. =)
Lon, I am sick and tired of the vegans too. I find them irritating, dogmatic, poorly educated, aggressive and plain stupid. Some are also dishonest.
I can’t believe that mature individuals can’t grasp a difference between not eating any animal product (vegans) and not eating meat only (lacto-ovo-whatever vegetarians), but “professional” vegans routinely drag innocent vegetarians as a proof of superiority of vegan doctrine. This is as dishonest as it can be. In addition, it looks like most vegans also cheat with diet.
Anna, from the vegan perspective, eggs and dairy are ethically no different than meat. Meat, dairy, and eggs all involve “enslavement” of animals, and egg and dairy production both involve the slaughter of unwanted animals (unneeded males and old females.) I am shamelessly omnivorous, but I actually agree with vegans that it’s ridiculous to claim the ethical superiority of non-flesh animal foods over flesh foods when production of those non-flesh foods leaves a trail of dead carcasses in its wake.
Maus, you’re missing my point. OK, at the same time you’re reinforcing my point (the same or different – too early too think).
You’re saying that vegans have a problem with vegetarians … OK, BUT they don’t have any problem with using vegetarians – VEGETARIAN athletes or just survivors (it’s always: “look this vegetarian has lived two million years which proves that veganism is ueber Alles”). Go, for example, to a ridiculous so called discussion at NYT (Can Athletes on Vegan Diet Perform – something like that)
thanks anna for your really good points – i will again content that veganism is a bourgeois eating disorder. there is simply no precedent in the anthropological record to support it regarding our health. the only reason people can currently survive and reproduce on such an inane non-human diet is because of massive supplementation and eventual medical intervention.
… and the oh-so-tired animal cruelty political stance is at best, pathetic – do vegans have any clue whatsoever what is being done to animals AND humans in the rush to grow frikkin soy or ANY field monocrop? the animal slaughter is absolutely staggering – bugs, birds, ground critters and the death from destruction of habitat. and the human cost of stripping the homelands and forests of say, brazil, to produce industrial soy is horrific. (not to mention the killing and dismembering of environmental activists trying to save the rainforests…)
” I find them irritating, dogmatic, poorly educated, aggressive and plain stupid. Some are also dishonest.” yes – me too but having now had a child later in life and getting down and dirty about what is actually human food appropriate for our genetic makeup, i have become downright hostile regarding id*ot vegans who feed their children a vegan diet – essentially starving them for their absurd, misguided political agenda. wanna screw your own nutrition and body fine, but feed a child what it is genetically adapted to digest and use – and that includes animal products.
I have written heartfelt letters to vegan parents i have met whose children are frail, nervous, scared, always hungry and pale – but not out-and-out sick …. yet. all to no avail – they consider me intrusive at best, villainous more often (i eat MEAT!!!!….)
so really – we can all save our breath – i understand Denise’s youthful wish to TRY to communicate to vegans (after her personal experience) but i bounced through her post (very good albeit pointless) and the comment section just made me gag.
what to do? i enjoy Denise’s intelligence, vigour and enthusiasm and will appreciate that!
You can’t blame the vegans – many experts say that it’s the best diet, it seems at first blush to reduce some animal suffering. . .As Lierre Keith points out, it’s only later when the B12 and other serious deficiencies kick in that they become aggressive, neurotic, and slide into eating disorder. No one tells them that what at first seemed so hopeful actually destroys the rainforest, enriches Monsanto, and causes massive animal harm of smaller creatures as it destroys soil health. The soy they eat adds more support to the GMO industry. But when they are suffering the neurological and mood symptoms of their deficiencies, it’s hard for them to understand what’s really happening to them. They deserve our support out back into health, not our contempt.
Sorry, but they won’t be getting any support from me – I’m busy defending my right to eat the meat that my genetic makeup finds necessary for good health and vibrancy, while they are fighting to take that right away from me and all other meat-eaters. The difference is that I don’t give a shit what vegans eat, but they care very much what I eat — to the point at times of violence and crime in the name of their beliefs. It’s never just a case of “to each his own” — NO, they have to change the world, and unfortunately, our government likes to take it’s clues from deceptive and misinformed agencies who agree that a “plant-based diet” (read vegan) is “suitable for everyone.” I simply don’t have the time or patience to consider them more than a group of stupid people who don’t consider anyone’s best health even a blip on the radar-
well said Ann and greensleeves – nice to see that there are others who are waaaaay fed up with these zealous food-malcontents…
You’re saying vegans are fighting to make meat illegal? Funny, I haven’t seen that reported in the news. There still seems to be plenty of meat at the grocery stores I go to. Or maybe you mean vegans are mugging meat eaters of their beef in grocery store parking lots and then giving those steaks a proper burial?
I’m not vegan or vegetarian btw, if that matters.
*this post is for entertainment purposes only*
“I’m busy defending my right to eat the meat that my genetic makeup finds necessary for good health and vibrancy”
1 – Human’s intestinal tract is 12x longer than any carnivore on the planet, and is more ribbed with pockets for fermentation of plant matter, much like a cow’s digestion process, but on a smaller scale.
2 – We don’t have claws. We have opposable thumbs and rounded nails for picking, climbing, and peeling. We can’t chase down game, it easily runs away leaving us starving. AR15’s are not natural.
3 – Our pH is much, much lower than any carnivore or flesh-eater on the planet.
4 – We have color vision to identify the vast rainbow of fruits and vegetables in any given forest. Nearly all carnivored have limited range vision, but incredible hearing for stalking prey.
5 – Teeth, nuff’ said. [“but we cook..” no, I choked on a piece of a steak when I was a kid, and it was finely cooked. That shit aint meant to be in a kid’s mouth!!]
6 – Intuitive salivary hunger response. Man wasn’t meant to put his food under a microscope. I’m out in the wild, I see a rotting dead carcass, I literally have vomited. I walk up to a berry bush, or see an apple tree – my mouth waters.
I understand how some vegans can be ignorant, but I don’t see how meat-eaters can be so blind to these anatomical facts?
Oh and for the record, I’ve never been healthy eating organic grassfed clean meats, nor was I healthy eating a 100% raw diet. So I’m fucked.
I’m literally about to go breatharian, lol..
Dude, you forgot the other *omnivorous* species. We’re far closer to *them* than we are to herbivores or carnivores or anything that only eats fungi.
Humans aren’t carnivores, we’re omnivores.
Your point is moot. No one is claiming we’re carnivores.
We have qualities of both the herbivore (the points that you mentioned) and carnivore (forward facing eyes, hunting techniques etc)
Two of the closest animals to us in biological composition from skin, organs etc are pigs and other apes. Both animals are omnivorous and eat fruits, veggies and meat, often in the form of bugs but sometimes hunting as well.
Personally, I seriously think different people need different diets. Some vegetarians do amazing on that diet. Others feel absolutely awful on the same diet.
I feel like I do better in the low carb end of the spectrum.
Also, I did vegetarian for a year and vegan for 6 months.
Thing is, any diet that require nutritional supplements is not optimal and definitely not the way we evolved to eat. Veganism always requires supplements.
Eating a balanced diet of fruits, veggies, complex carbs, a few simple carbs (particularly on days where you expend lots of energy IE exercise), fish, little red meat etc pretty much covers everything you need. You get in the vitamins and minerals, protein, fat and carbs your body needs.
And lastly, we honestly do not know what optimal is. just because humans evolved to eat a certain way doesn’t actually mean that it’s optimal for health. Evolution doesn’t work that way. Mother nature doesn’t know best, but it does know something, if that makes sense.
We’re constantly learning new information about how our bodies intake nutrients, what diets work best for people with certain criteria (certain illnesses or imbalances)
Sadly a lot of it is guess work. All I can say is that an elimination diet, one in which you try to figure out what foods make you feel best and what foods you have negative reactions to (if any) is the only way to figure out what works for you (taking into account any nutritional needs one may have due to disease, allergies etc), and tons of people do not have the time, money or motivation to do a diet like that.
About the only thing we do know for complete and utter certainty is that too much sugar or simple carbs in a diet are not good for us, simply because humans have not existed long enough in a time period in which soda, twinkies and white bread have just been completely at our disposal in the 1st world countries.
But at the same time, mental health has a HUGE role to play in over all health, considering the brain controls or influences pretty much all the rest of the body, it’s condition matters a lot when it comes to physical health, part of the reason the placebo affect even works and why having a loving family and a reason to fight for life can make people live longer despite whatever bad health habits they may have. And there is something to be said for treating yourself in typically bad, but not dangerous in moderation things that can increase longevity.
Hi Anne (and others here), I know this is an old thread but I wondered what your thoughts on eating in Space were? There’s a push towards a colony on Mars. If veganism is out for long term nutritional health, would eating insects meet the protein requirements? They seem easier to ship to Mars than cows, and can feed of fruit and vegetable scraps and peelings that the colonists would be eating anyway.
Insects have a great nutritional profile – generally high in fat and animal protein.
A 30 second internet search would change all that. Willful ignorance is no excuse.
Sorry, but isn’t most of that soy you mentioned used to feed animals? Also, eating vegan doesn’t necessarily mean eating a lot of soy..
I’m an omnivore too, but by saying that vegans (like … what … 0.2% of nowaday’s population?) are responsible for soy monocrops, loss of rainforest and Monsantos awfulness, you are in NO WAY better than the most delusional raw vegan-frutarians ever. Sorry, but more than 80% of nowadays soy-output is used as animal food, even for animals that can’t digest it properly like cows. I have no reason whatsoever to deny that animal food (and meat) contains very healthy things and is eaten for 1000s of years by human beings, but the soy argument is just ridiculous.
Yes. Bringing Monsanto into this is just ridiculous, it’s a whole other line of argument. If vegans make a lot of environmental claims about their diet, *possibly* it could be a point to rebut that claim. But for ordinary vegans just trying to eat to be healthy, to slam them with this Monsanto label is just not fair.
What Monsanto do is what the vast majority of vegans, raw foodists and anyone interested in or knowledgeable about food are against. I am of the impression that vegans are much more pro-environment than low carbists. A number of people have called vegans “stupid” and “idiots” above and show a lot of hatred towards them.. Surely the real enemy is Monsanto and the legislators who allow them to do what they do.
It’s neither accurate not right to throw around the terms Monsanto and GMOs like that about these individuals who are vegans, unless these people are knowingly eating GMOs. Vegans aren’t responsible for what Monsanto does, and neither are low-carbists. Monsanto is responsible for it.
Suppose Monsanto got into animal transgenics, are you supposed to ditch all your eating of your favourite meat from then on to avoid them? That wouldn’t solve the problem. You have to fight the real enemy. For the small proportion of vegans who do think GMOs are just fine and dandy and advocate them, yes, they deserve all the seven flames of hell thrown at them and to burn there forever for betraying not just everyone else in the world but all of our descendants to come and all other living things on the planet.
I’ll give a paleo-eating agreement to your statement here. Saying vegans are instantly supporting Monsanto is wrong. I have vegan friends and they go out of their way for organic non-gmo everything.
While I’m a hard core paleo eater, I feel like far too much energy is wasted between paleo and vegans fighting. The fact is that the whole world is not going to wake up one day and turn paleo and/or vegan. In fact, most Americans don’t have any desire to eat better, at all. They want the decadence of sugar, grains, etc. The fucked up part is that people who eat healthy end up footing part of their health bill by being lumped into the same medical policies.
I think a much better point could be made here that until we get added sugars, chemical food additives, and vegetable oils, we really aren’t doing a damn thing. The last two substances here are changes that need to be made at a policy level. i.e. NYC outlawing transfats. Let’s switch the country to using coconut oil for cooking and start banning food additives that are causing major health problems. Perhaps we start taxing sugar like cigarettes to cover the added burden it’s putting on our health care costs?
Once these three matters are taking care of, vegans and paleos can have a steel cage death match to determine the future. I’ll be in the corner of the bacon eaters of course.
Treys, great post however one issue about semantics: I don’t how you say “paleos” as if it’s the anti-thesis of veganism. Certainly a lot of the people who call themselves “paleo” today are eating nothing like the paleo lifestyle… which was super high in fruit just like how all of the other great apes eat to this day. I myself would like to think I follow a paleo lifestyle as best I can, though I still have potatoe chips from time to time.
Padraig,
Rubbish. Fruit isn’t available year ’round in any but the most temperate climates. At best we can say that the cultures living in temperate areas likely ate a diet “super high” in fruit and the ones in glacial areas ate a diet super low in fruit. Those in-between only got “super high” fruit intake for a few weeks a year, when it was in season. And since the Earth was in an ice age until about 10,000 years ago, the idea that early humans ate mostly fruit for the 100,000 years prior is simply not supported by anthropology and climatology.
paleohuntress, the most temperate climates is where humans and their ancestors evolved until about 70,000 years ago when they left Africa (and about 50,000 years ago for when they left the temperate regions).
I think that was a mini ice age and I think we’re still in fact in it. Fruit and indeed all life, has enough time to evolve along with ice-ages to ensure that their species does survive. Despite the name, the whole of the earth isn’t covered in ice, it is just a number of degrees lower.
The “paleo = carnivore” idea was popularized decades ago from books such as Man The Hunter and initial flimsy evidence that has since been overturned. Adrienne Zihlman was among the first critics, the ways we interpret evidence now have changed drastically and serious anthropologists generally dismiss Man The Hunter now as allegorical nonsense designed to capture the imagination of the masses. The theory falls on many levels: anthropologically, the fact that the model doesn’t reflect tribes of today, and make-it-up-as-you-go-alongness. Firstly, if man did eat significant amounts of meat, it would have nearly all been done by scavenging, not actively hunting. So that would be a philosophical shift if nothing else for many so-called “paleos”. Secondly, it would only have been on the rare occasions they were hungry…. so-called “paleo” folk love to rave about the chimps hunting, all the gang going out to capture monkeys, using spears etc. certainly captures their imagination… but there’s one catch:: recent estimates have shown that meat only actually accounts for about 3% of chimp diet, not the 80%+ many so-called “paleos” prescribe …. oops!
To add to what paleohuntress said, even in tropical areas it appears that paleolithic humans ate substantial meat, what with the koobi fara site showing consumption of hippo and other large herbivores almost 2 million years ago.
Padraig, recent reseach shows that we transitioned from scavenging to hunting at least 2 million years ago as well.
That doesn’t mean we were carnivorous – we might have eaten moderate amounts of fruit – but we were certainly very far from vegan.
Padraig,
“the most temperate climates is where humans and their ancestors evolved until about 70,000 years ago when they left Africa (and about 50,000 years ago for when they left the temperate regions).”
I’m not quite sure what point you’re making here. I agree, many of our human ancestors left temperate areas and thrived in colder climates without much or even ANY fruit consumption. This is pretty much the same thing I wrote.
I guess we could argue semantics, but frankly I believe you understand my point. The earth is currently in an interglacial period, and the last glacial period ended about 10,000 years ago, right around the time that agriculture popped up.
“Despite the name, the whole of the earth isn’t covered in ice, it is just a number of degrees lower.”
Though obviously global temperatures are causal in glacial periods, they are not defined by temperature, but rather by how much surface is covered in ice sheets.
The Flying Spaghetti Monster is the deity of the Church of the Flying Spaghetti Monster or Pastafarianism, a movement that promotes a light-hearted view of religion and opposes the teaching of intelligent design and creationism in public schools. Although adherents state that Pastafarianism is a genuine religion, it is generally recognized by the media as a parody religion.
There was no one single paleo diet. Without a doubt, there were paleo cultures who ate animal foods and little else just as there were cultures who ate plant foods and little else. To suggest that either one is somehow “wrong” because it doesn’t fit YOUR ideal is disingenuous.
Huh? Early humans hunted many animal species to extinction. There is no question that they scavenged too, but there is evidence of pit-traps and even stampeding herds over cliffs. They also consumed significant quantities of fish, shellfish, insects, land crustaceans, turtles, etc.
Could you be ANY more condescending? I mean really. The ‘so-called’ “fruitarian” or “vegan” belief systems are somehow not ridiculous? Please. If the idea is too vague to define then it isn’t worthy of debate, if however you are going o put time and energy into he debate, then clearly you consider the debate worthwhile. Dismissive qualifiers like “so-called” are also disingenuous and when used to suggest disdain, merely make you look fickle. Modern paleo is a diet template and how a person chooses to fill that in is going to be based on their own specific macronutrient needs.
First, “meat” and “animal food” isn’t the same. I don’t know why chimps’ diets are so contentious among the plant-based community. The fact is that homo sapien sapien is NOT a chimp. We are far more dissimilar genetically than Darwin’s finches (all from the same common ancestor) whose diets range from almost fully carnivorous (with some consuming blood) to fully vegetarian. Who cares what the chimps eat? We are human. Oops!
psychohist,
“That doesn’t mean we were carnivorous – we might have eaten moderate amounts of fruit – but we were certainly very far from vegan.”
That’s completely false. We would have eaten huge amounts of fruit, as much as was available. On the other hand we were very close to being vegan when we did not have to eat meat. Meat was used as a backup for when times were very bad and there was no fruit. Note that I am not a vegan and think veganism is unnatural and stupid.
What a bizarre “concession”… “we might have eaten moderate amounts of fruit”… who do you think you’re kidding? You’d fit right in with those utterly deluded so-called “paleo” group forums.
paleohuntress,
“I’m not quite sure what point you’re making here. I agree, many of our human ancestors left temperate areas and thrived in colder climates without much or even ANY fruit consumption. This is pretty much the same thing I wrote.”
I would never say our human ancestors THRIVED in those conditions: on the contrary: they nearly died out!!! Many of them starved to death!!! Faced with a new environment completely unlike what they’d known before and a massive shortage of fruit, life was short, brutal and miserable for these primates. That’s why the majority of these populations, especially Neanderthal ones, went extinct. It was the exact opposite of thriving in every way.
“The Flying Spaghetti Monster is the deity of the Church of the Flying Spaghetti Monster or Pastafarianism, a movement that promotes a light-hearted view of religion and opposes the teaching of intelligent design and creationism in public schools. Although adherents state that Pastafarianism is a genuine religion, it is generally recognized by the media as a parody religion.”
I really have no idea what this has to do with anything I said.
“There was no one single paleo diet. Without a doubt, there were paleo cultures who ate animal foods and little else just as there were cultures who ate plant foods and little else. To suggest that either one is somehow “wrong” because it doesn’t fit YOUR ideal is disingenuous.”
Now hold on, the paleolithic age lasted a long, long time… from 2.6 million years ago to about 10,000 years ago. For over 90% of that time there was no such thing as homo sapiens, and for the vast majority also our brain size was much more like chimps. In the earlier half of the paleolithic era, it’s highly likely that our ancestors all ate a very similar diet as chimpanzees do today.
.
You’re completely right that there is no one “paleo” diet. That’s why I suggested that the people on the so-called paleo diet should call it the “neo” diet, for the diet eaten by people during the neolithic era. That’s the essence of all the arguments I have with these so-called “paleo” eaters…. they’re not being honest and truthful about what was eaten during the paleolithic era. They are crazy and ridiculous and misleading people. A true paleo diet would have at least 90% fruit.
“Huh? Early humans hunted many animal species to extinction. There is no question that they scavenged too, but there is evidence of pit-traps and even stampeding herds over cliffs. They also consumed significant quantities of fish, shellfish, insects, land crustaceans, turtles, etc.”
Where is the evidence that they “hunted many animal species to extinction”? That sounds like a very strange thing to be able to know. Also I don’t know what “significant quantities” are… I know chimps eat quite and amount of insects, that’s why I always try to get at least some small amount of animal protein every week. .
“Could you be ANY more condescending? I mean really. The ‘so-called’ “fruitarian” or “vegan” belief systems are somehow not ridiculous? ”
The “so-called” part is necessary because as explained above, these people are no more eating the “paleo” diet than your average “meat, potatoes and two veg” type of individual. I don’t have to put “so-called” before “vegan” or “fruitarian” because whatever you or I may think about those diets, they at least actually describe the type of diet it is. “paleo” doesn’t, it’s a wildly inaccurate term to use. They might as well name themselves to be eating the “right” diet.
The “vegan” belief system is ridiculous yes. Certainly some of the people who are calling themselves “fruitarian” on the internet are ridiculous. However when completely in the wild, when you can get vitamin b12 from the bacteria on the freshly picked fruit, being a fruitarian is IMO not ridiculous at all.
“Dismissive qualifiers like “so-called” are also disingenuous and when used to suggest disdain, merely make you look fickle. Modern paleo is a diet template and how a person chooses to fill that in is going to be based on their own specific macronutrient needs.”
derr derr derrr. Maybe instead of the flowery language you could try to see my point a bit more, and think a little bit more since in your OWN POINT above you state there is no such thing as a single paleo diet! As I said above, the whole idea of these people saying they’re eating the “paleo” diet really riles me up, because they’re NOT eating it. Even if they CLAIM they’re eating a paleo diet, they CANNOT call their high protein low fruit diet “the paleo diet” or “the primal diet” because it’s ridiculous, it’s a joke and it’s extremely misleading and just plain stupid and wrong.
So I put a “so-called” before it. Because I do not believe it’s a “paleo” diet. What the hell could be fairer?! My idea of the “paleo” diet is vastly different.
“First, “meat” and “animal food” isn’t the same. I don’t know why chimps’ diets are so contentious among the plant-based community. The fact is that homo sapien sapien is NOT a chimp. We are far more dissimilar genetically than Darwin’s finches (all from the same common ancestor) whose diets range from almost fully carnivorous (with some consuming blood) to fully vegetarian. Who cares what the chimps eat? We are human. Oops!”
We are human, but I view humans as a kind of monstrosity, in particular after we left Africa all the normal developments of natural selection and evolution went out the window. Sexual selection turned into a complete joke among humans. We are a bizarre mish-mash of everything gone wrong. We really shouldn’t even be walking on two legs, as we realize when/if we get old and our legs fall apart. This is why I’ve been trying to walk around on all fours lately, however our evolution somehow made this uncomfortable as well so we’re stuck between a mass of evolutionary contradictions.
Padraig,
and-
One has to wonder if it is only you who can time travel since the meat to fruit ratio in primitive man’s diet appears to be something that only you know definitively. LMAO
Considering that geneticists have determined that there was a genetic bottleneck of approximately 10 males in our human genome, it would seem that ALL humans nearly died out. I suppose there was something more relevant than meat versus fruit determining human survival.
Yup… that’s pretty much what I was thinking when I read what you wrote. I figured I’d respond in kind with something equally irrelevant to the topic at hand. =)
Very true. But modern man didn’t emerge at the start of the paleolithic so the point is moot.
lol Precisely. And just like Darwin’s finches, each descendent branch went its own way, likely based on DIET. Chimpanzees may not have evolved much from our common ancestor. But the fact that we evolved differently suggests there was a stressor and adaptation that facilitated it. Meat! Who cares what was eaten 2 million years ago? What matters is what homo sapien sapien evolved to eat.
Perhaps you have a hidden tardis you’re beaming through time with? Saying it again doesn’t make it any less false.
Comparing the archaeological records of Australia, North America and New Zealand, all three places lost their megafaunas when people arrived.” ~Surovell and Grund
So “quite an amount” doesn’t translate into significant in your eyes? Insects make up abut 5% of the chimp diet and according to The Predatory Behaviour and Ecology of Wild Chimpanzees, chimps possess the first instance of organized hunting and carnivory in hominids- the first instance where other, larger mammals are being hunted in an organized fashion.
Really? “Vegetarian” has a single definition? A vegetarian may be a vegan, or an herbivore or a frutarian or a hygeinist… they may eat eggs, fish or dairy. In fact, most people who identify as vegetarian still eat MEAT in quantities comparable to self-identified omnis. “Vegan” is a term that was coined to refer to someone who not only doesn’t eat meat, but who doesn’t use or consume anything that was derived from the labors or exploitation of animals. (well except for most all of agriculture which depends on animal pollination, but why splits hairs?) Honey from bees, bad. Fruit from bees, good. But most people use it to infer that they don’t eat any animal foods. And “fruitarian”? Hah! “There is a lot of gamesmanship, sleight-of-hand, and word redefinition that goes on among fruitarian advocates to redefine “fruit” away from the common definition (soft, pulpy, sweet, juicy fruits from tree or vine) so that it includes the so-called “vegetable fruits” like peppers, cucumbers, tomatoes and the like, or “nut-fruits” and so on, so as to broaden what is considered “fruitarian.” In a botanical sense, these foods can be considered fruits, and thus–if we stretch things a bit–perhaps “technically” permissible in what might be called a “fruitarian” diet. The problem, however, is that most fruitarians don’t even stop there either. Most go further and allow or even specifically recommend “greens” and/or “green-leafed vegetables” as essential, and of course neither of these qualify as fruit even in the botanical sense. Once you get this far, any sense of integrity about what “fruit” really means has been sacrificed to the realm of fast-talking slipperiness.” ~Ward Nicholson
So drop the high and mighty bullshit. Paleo refers to a template- just as does primal, ancestral and caveman. It is no less descriptive than the so-called vegetarian, fruitarian or vegan diets.
You can’t. This is a myth. B12 producing organisms live in the soil and in the hind-guts of mammals. If you were pulling plants out of the ground and eating dirty tubers with the soil still on them, this might be true. But there is no B12 on unwashed fruit- after the seedling emerges from the soil, any B12 it may have on it gets washed away by rain. And contrary to this image of soil-splashed plants after a rain, there is no bare ground in the wilderness. I both garden and forage and the ground around wild plants is naturally mulched with last season’s dead plant matter in the same way I mulch my garden to keep my greens from getting muddy when it rains.
Get over yourself.
Kewl. So after all of that, you completely invalidate every argument by voiding all references to other similar animals with your disclaimer. ROTFLMARO
~Huntress
I don’t find it worth it to reply to most of your post paleohuntress, especially because your last sentence shows you don’t understand what I’m saying at all, but I find this particularly hilarious.
“There is a lot of gamesmanship, sleight-of-hand, and word redefinition that goes on among fruitarian advocates to redefine “fruit” away from the common definition (soft, pulpy, sweet, juicy fruits from tree or vine) so that it includes the so-called “vegetable fruits” like peppers, cucumbers, tomatoes and the like, or “nut-fruits” and so on, so as to broaden what is considered “fruitarian.”
HAAAAAAAAAAAAAAAAHAHAHAHAHAHAHAHA!!!!
Those fruits were NEVER vegetables except in the supermarkets of fool Americans and other westerners. Personally I never even knew peppers were ever considered “vegetables”, by what stretch of the imagination someone came up with that I will never know. Such a joke.
Padraig,
You don’t even realize that you have just evidentiated my point so poetically. The ‘so-called’ fruitarian movement can’t even agree on that constitutes fruit. You should take a look at who Ward Nicholson is. Keep laughing my so-called fruitarian friend.
~Huntress
Based on the nearly complete “Ardi” – Ardipithecus Ramidus – fossil documented a couple of years back, the common ancestor of humans and chimpanzees was bipedal and upright. If there’s a branch from that which became a “monstrosity”, it’s the chimps, not us.
I thought the paloo diet was supposed to be more like what Cro-Magnons and Neanderthals ate in Europe during the Ice Ages, not like how all of the other great apes living in the wild in Africa and Southeast Asia eat to this day.
PLEASE, no, not coconut oil in everything! Or at least label it . . . My husband is allergic to coconut, along with several additives. At this rate, he may never be able to eat out.
If you eat at all in a country that has GMO legal, you support Monsanto. However, almost all vegan and vegetarian food in the states will have soy in it, which is very likely to be Monsanto. Omnivores can eat grass fed beef if they can afford it. For a while nonGMO was not an option
Eating cheap supports Monsanto, regardless of diet. Most people can’t afford grass-fed, organic, non-gmo. I happen to live in a country where gmo is illegal.
Point still stands though. Any diet which forces you to take supplements, or hunt desperately and “make absolute sure” that you get in this vitamin, this mineral or this macro nutrient is probably not the best diet. And vegan does this. Vegetarian or pescetarian are better options with all we know about health and how the human body works.
It seems that the best diet is one of moderate to lower moderate protein, moderate fat and somewhat low carb. a 50 fat-30 protein-20 carb scale or something similar. Not this 10fat 40protein 50carb nonsense we eat today Protein and fat sources from healthy fats like avocados, oilves, fatty fish and shellfish and on occasion (say once or twice in two weeks) some red meat. Carbs mainly coming from low amounts of fruit and high veggie along with minimal starches and refined sugars.
This gets in everything someone needs and leaves tons of room for variety and flavor.
I think the key to a good diet is variance. Our ancestors would of had something like this due to being nomads and eating what they can
All I know is carbs were just plain not plentiful before agriculture and berries and honey were very special and rare treats. Veggies/root fruits, meat source (hunting or fishing) were the most likely staples for how we evolved. Fish seems to be one of the better ways to get in omega 3, healthy fats and other nutrients.
Eating disorders aren’t things you should throw around lightly. An eating disorder is a mental disease and has far, far less to do with food than most people think. It can be offensive.
Veganism was the number one thing that saved me from my eating disorder, an illness which was felt predominately in my mind, my food choices were really a symptom.
However, I do strongly agree that many vegan parents do not properly feed their children (I grew up with a few unhealthy looking vegan friends) and would benefit from taking the advice of a well educated person! But then again, many parents could use similar advise for their overweight, undernourished children. It is an unfortunate world where so many people do not care for their health or at the very least, the health of their offspring.
Actually, harvesting non-animal non-flesh foods happens to leave a trail of dead carcasses in its wake too:
“The other reason for beef eating is, hold on, ethical–a matter of animal rights. The familiar argument for vegetarianism, articulated by Tom Regan, a philosophical founder of the modern animal-rights movement, is that it would save Babe the pig and Chicken Run’s Ginger from execution. But what about Bugs Bunny and Mickey Mouse? asks Steven Davis, professor of animal science at Oregon State University, pointing to the number of field animals inadvertently killed during crop production and harvest. One study showed that simply mowing an alfalfa field caused a 50% reduction in the gray-tailed vole population. Mortality rates increase with each pass of the tractor to plow, plant and harvest. Rabbits, mice and pheasants, he says, are the indiscriminate “collateral damage” of row crops and the grain industry.
By contrast, grazing (not grain-fed) ruminants such as cattle produce food and require fewer entries into the fields with tractors and other equipment. Applying (and upending) Regan’s least-harm theory, Davis proposes a ruminant-pasture model of food production, which would replace poultry and pork production with beef, lamb and dairy products. According to his calculations, such a model would result in the deaths of 300 million fewer animals annually (counting both field animals and cattle) than would a completely vegan model. When asked about Davis’ arguments, Regan, however, still sees a distinction: “The real question is whether to support production systems whose very reason for existence is to kill animals. Meat eaters do. Ethical vegetarians do not.”
Read more: http://www.time.com/time/magazine/article/0,9171,1002888,00.html#ixzz20kxHWCda
(the quote is from page 8)
Now, the above is comparing best and worst case scenarios in production of grass-fed beef vs large scale factory farming, but one can also include the human cost in immigrants who are treated poorly or die trying to get to places where crops are harvested just to get enough money to feed their families and.. “ethical superiority” is quite a relative thing and I don’t think anyone has the high ground there just from choosing general food types. One can perhaps move a little up or down the ethical slope by choosing foods from particular sources or growing them one’s self.
That’s rediculous. that’s like saying black people steal from your house in the night. get a grip and grow up. I’m not claiming to be anything but humane yet you perpetrate the ignorant side of life.
Yes, the vegans and the agricultural corporations have formed an axis of evil! :). This analysis is very entertaining, in the way that Rush Limbaugh can sometimes be. I would estimate that the analysis of this study is about 10 times more flawed and innacurate than it claims the study is.
I agree with Lon…seriously, whatever happened to “Live and let live?”
I suppose it all depends on what vegan’s vitamin D level was the whole time. Look at Steve Job… It would have cleared up the big picture significantly. I believe that vitamin D is the ultimate role of cancer fighter compared to anything else. I have my old clinical nutrition book saying it’s a cancer fighter but VERY LITTLE to go on. Now thanks to Vitamin D Council and Grassroots Health, we know much more about it. Getting it out to public is another story. According to this website, it could potentially save us 4 trillion dollars in health care expense. http://lewrockwell.com/sardi/sardi111.html
That’s a lot of businesses to bankrupt dependent on healthcare…
Vitamin D prevents cancer initiation, but high blood sugar promotes cancer growth. High carb diets, which vegan diets are likely to be, are more likely to cause high blood sugar.
Denise,
Are you familiar with the book ‘The Starch Solution”? Endorsed by T. Colin Campbell I actually had a pretty good laugh reading a few things from it such as high carb diets are healthy.’ As always, solid job. The fact that you tagged your post as ‘hedghogs’ makes it that much better!
High card diets are indeed healthy! I feel my best eating a high carb diet composed mostly of potatoes, rice, beans (properly soaked/prepared), bananas, some fruit/fruit juices, very lean cuts of meat, some cheese and a little milk.
…Not to much the numerous societies and cultures that eat high carb and enjoy good health.
Ha ha. I laugh at you, actually.
Are you a fatass?!!
Of course you feel better. Carbs or more specifically glucose (sugar) is what the body prefers to run on because it’s easy energy. That doesn’t in anyway mean it’s good for you. Carbs are for instant use and aren’t good being the biggest part of your diet. Even if you don’t have a low carb tolerance like many people (and most don’t know it) that many is just simply not what our bodies adapted to. You get in lots of nutrients, but the body isn’t evolved enough to handle that amount of sugar. In case you didn’t know carbs = sugar. In fact, the body only has two fuel sources. Fat and sugar. Protein also, gets broken down into sugar. Many many MANY people do not know that. That’s why high protein is bad too.
Sugar+fat =body fat. Carbs bind fat lipids so that they’re harder to work off.
If you lead an active lifestyle, your high carb diet won’t be as bad, but there are still many health repercussions.
Also name 3 societies that function really well on high carb. Because I can’t think of one
Medeteranian, most Asian and Inuits function on either high fat moderate carb, or high fat low carb. The inuits eat really really high fat and mostly meat.
The longest living people (not just an anomaly like one random person, but actually hordes of 90+ people) are to my knowledge in Okinawa. They eat mostly fish and veggies, have an 80% full plate rule and most importantly of all, they feel wanted.
The true key to health besides diet is usefulness and feeling like you’re wanted and helpful in older years. Mental has just as much if not more to do with health and longevity then diet or exercise. Depressed or mentally ill people tend to not have good diets.
You’re reply shows how incredibly ignorant you are concerning the diet that Dr McDougall recommends. Maybe if you’d actually read it you’d have a different perspective. And no where in the Starch Solution does he say to eat snackwell cookies. Also, how is it the Chinese, or the Okinawans can eat a mostly starch based diet and be thin, and have long lives and be free of many chronic metabolic diseases?
The Chinese aren’t long-lived and healthy at all, I don’t know where anyone would even get that idea. They’re struggling obesity, metabolic syndrome and heart disease.
The Okinawans have a genetic component that leads to longevity as evidenced by the longevity of Centenarian’s siblings, regardless of diet.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3259160/
Add in that calorie restriction always extends longevity and you have a culture whose diet may have little or nothing to do with their overall health. Heck, you can improve health on the Twinkie Diet as long as calories were kept low. Plus, the Okinawans don’t eat “corn and potatoes” like McDougall recommends, and they eat PORK.
In addition, the Okinawans traditionally ate a mostly fish based diet, and the modern addition of starches has coincided with poorer health.
What a masterful piece of Bloggdom!!!
Holy moly, two Wyatts. I’d say this blog is big enough for the two of us. 😉
Wyatt Power! ☺
Not true. It’s Ann(a)s power. No sharing.
Minger is back. Finally. I was starving intellectually. I’ll read tomorrow.
Great study shred, as usual! Wow, that 30 bananas page is scary!!! Poor Charlotte Darling! Wonder if she’s still alive?
“And that’s okay! We’re all special snowflakes” Hahahaha. Your writing style is pure gold. If I come to Portland Denise can you autograph my copy of “The China Study”?
Denise,
Excellent post. To me, it’s not so much an issue of bad science but rather a lack of integrity, intellectual honesty. There are many causes of obesity and disease far more complicated than animal food consumption. Are you aware of the exploding ME/CFS epidemic? Do you know of Dr. Jamie Deckoff-Jones’ blog? There are in fact tons of stealth viruses going around that the “scientific community” fails to recognize and these are playing a huge part in our ill state of health. The picture is far more bleak and probably hopeless than anybody realizes. And it will only get far worse before it has any chance of possibly getting better. In the future, people will eventually realize that obesity, diabetes, and heart disease are to an extremely large degree infectious disease related ilnesses. If HIV didn’t kill, would it have even been identified? If you think government dietary advice has been bad, take a look at the sorry situation of Gulf War Syndrome. The high rates of veteran suicides are not only a result of PTSD, many of them are in fact sick and just suffer in silence.
ahhhhh? dsfd – do you really think we would, as a species, have made it this far without an immune system primed and tuned to nail **almost** anything thrown at us? the key here IS the diet, and the bad science IS EXACTLY the issue – in fact, this study is not science at all. ONE questionnaire in 16 years about diet and then reams of analysis of that collected data? this is number-crunching, postulating masturbat*ion of the most frantic kind – not science.
… and i think that there are some VERY GOOD postulation as to the “gulf war syndrome” being a result of the untested and highly questionable/toxic vaccines that were massively administered to these poor service people – and that is not even to mention the nuclear waste ground weapons that were used extensively –
eat a real human diet and up your survival chances exponentially…
Respectfully, you don’t know what you’re talking about. The majority of the of the world’s population already eats real food for the most part. The obesity, diabetes, and other degenerative disease epidemic is NOT only a result of diet. There are in fact huge biological events taking place that are going unnoticed for many reasons. As more people get sick however with various infectious diseases, CFS, Lyme, GWS, hepatitis A B C (the ones we know about) etc…, then doctors and scientists will begin to pay attention….but it may be too late by then. While diet and lifestyle changes are always useful, they don’t do a damn thing if you’re positive for HIV or if your sexual partners are. I’ll ask again: If HIV didn’t kill, but just slowly deteriorated it’s victims, would it even have been identified? That is exactly the situation for those with ME/’CFS. There are (officially) 17 million ME/CFS sufferers alone yet they are hardly noticed. That will change. It is in fact an INFECTIOUS DISEASE.
Vaccines, biotechnology, and military bio-weapons probably have much influence here.
These blog posts are fascinating, and right in the veign of this comment thread. Dr. Jack is a little difficult to follow, and I must say, as bright a bulb as I consider myself, I do have a “time” understanding it all, and I find I must read a couple of times to feel that I have an even basic grasp of what he says.
I’m not saying he’s right, or that others are wrong, but some of his hypotheses are staggering…
http://jackkruse.com/brain-gut-1-who-are-we-really/
http://jackkruse.com/brain-gut-2-viral-marketing/
http://jackkruse.com/brain-gut-3-look-in-the-past-to-see-your-prologue/
And I happen to find the comments sections of these posts EVERY BIT as interesting as the posts themselves! It’s fun to see people have that “Oh! Yeah! Duuuuhhh!” moment!
dsfd, I very strongly agree with some of what you’re saying, though I think it’s inaccurate to say that ravi has “no idea what you’re talking about”. ravi does have some idea what he/she is saying, they are making a point. You can agree or disagree with what they’re saying. However they’re not like Anna, who was talking about bread being good for you and eating a diet of a lot of fruit giving you “horror diarrhea” (however the hell you spell that).
What ravi said makes a lot of sense. It would be true if we were living in the environment we are perfectly evolved to live in. It’s the civilized world and the spanner that has thrown in the works that is creating all of these nightmare viruses, infections and bacteria that NEVER occur in the wild or in nature.
But I strongly and profoundly agree with you on two things:
1) That the situation of humanity is hopeless. We are way beyond the point of humans as a species having a chance to survive. All of these microorganisms, viruses, bacteria, tiny flies, all evolving and multiplying in obscenely unnatural environments. Humans cannot hope to stay anything like they are now with this sort of thing going on… that is why there are “big bangs” in evolution followed by relatively stable periods…. because once one key element in an ecology changes they all have to change. And then there is the insane joke of purposefully genetically modifying organisms, which will exponentially accelerate the process of imbalancing and destroying the ecology, environment, and thereby humanity.
Optimism is really a LIE. It means purposefully taking a non-objective view of something, it is just as bad as pessimism. There is a book called “The Optimism Bias”, which looks at this curse of trying to be “optimistic” as we’re going down in flames. All of these people are such utter clowns.
It’s so bad almost everyone purposefully tries to be optimistic, to put a smile on their faces and put on a good mood. They find it helps them in their daily lives, as this lie that they put on themselves instinctively gets other people to view them in a more positive light. But the thing is… it is all just lies upon lies upon lies… all false and fake… refusing the natural human reaction of misery and despair, things which have a purpose… to get you working really hard, fast and passionately about the situation that is killing you or threatens to!!
2) I really like and agree with your emphasis of this small, subtle damage that we’re being subjected to. According to the orthodox medical literature, if it doesn’t have a huge, observable effect on you that can be routinely tested for and catalogued, then it doesn’t exist. This is how it works in Cloud Cuckoo Medical world. You come in and give symptoms, the doctor tells you what’s wrong or gets you tested, and then you get pills for it or perhaps surgery…. that’s how the entire scheme is built up.
Anyone talking about subtle differences, such as the fact that they are genetically modifying foods in ways that nobody has a clue what effect they’re having on people, is just snubbed. People are told “derp derp where you’re evidence???”. Their stupid tests show GM food to be “safe”…. but in how many subtle ways is it killing us or inferior to the natural food we were evolved to eat???
There is every reason in the world to assume that food that has naturally co-evolved with our ancestors for millions of years would be infinitely better for us that food just RANDOMLY CHANGED in ways they don’t even understand themselves. It’s just crazy stuff.
If I could I would engineer a virus that would wipe out the one organism in the planet that is causing all of this deranged nonsense… humans. Then maybe our relatives the other great apes and all of the other animals in the planet would have some sort of hope of surviving, despite the fool human’s best efforts to mess it up.
It’s always nice to see someone who thinks.
Have you seen this btw?
Soon, everybody will have this misery. (Ms Minger included)
Food does matter. I am someone with CVID (which is a primary immunodefiency) and I don’t make IGG, IGA and only about half of the other immunobodies. I get an infusion of IGG monthly and though that helped nothing has done my health so well as eating paleo. I used to half CFS, now its gone. Infections, mostly gone. I can breathe through my nose, I am entering the coldest month of the year and I haven’t been sick since the first week of summer. No colds, no flus, no coughing fits…every time I have felt a cold or infection coming I up vit D intake and go to sleep early.
Good for you. We should all be so lucky! Unfortunately, we aren’t. Paleo/LCHF/SCD have helped me a lot as well, but probably less than you….and they are by no means panaceas. Imagine telling an HIV or hepatitis patient to forego his meds and replace it simply with lifestyle changes! My point stands: within the next decade or two, it will become increasingly clear that stealth viral/bacterial infections are at the root of almost all degenerative disease, especially in younger people. Doctors/Scientists now scoff at that notion. In the future, they will realize its fundamental veracity. You can in fact “catch” obesity, CVD, MS, Autism, cancers, stroke, etc…. The exploding obesity epidemic is NOT only lifestyle related. Teitelbaum states that the “average” CFS weight gain is 36 pounds. This is just the bare tip of the iceberg.
Heck, given that the symptoms of autism are behaviors, you can even *teach* people to might as well be autistic (“don’t care about what other people think!!!” “social skills are for snobs and jocks!!!” “who cares about liberal arts, math science math science [as if a university with a College of Liberal Arts isn’t where that university will put its pure-sciences departments like biology, chemistry, physics, and math]!!!”), like the lady who wrote that Toger Mom book tried to do.
I hope you’re trolling or sarcastic. That or you have NO idea how autism or any mental disease works. Behavior is not something easily changed by any means. Our brains do NOT like changing habits, because it’s easier then change and evolutionarily speaking, it was beneficial at the time to have the “if it ain’t broke, don’t fix it” (which is a really stupid mentality as it promotes stagnation and lack of discovery, which kills species)
Autism is a disorder in which the persons social part of the brain doesn’t connect in the same way a “normal” persons does. Autism can vary greatly in how it manifests, for some it’s not an issue. For others it destroys their life quality and ability to function as a normal person. Same goes with any mental illness or disorder, such as clinical depression, chronic procrastination (often associated with depression and/anxiety) OCD, bi-polar, borderline personality disorder and many many others.
That sounds an awful lot conspiratorial there. What in the blue blazes use would our government or anyone’s government have for deteriorating it’s own subjects and economy bloods health and longevity? Sure, doing things overtime to get more people into hospitals and shell out money for something that could of been prevented, but out right killing? That doesn’t make money and therefore doesn’t make sense.
Also, it’s true that pollution attributes to higher obesity and health declines, but that could be due to either toxins, mood ambiance that big cities cause or just the culture in places that happen to have high pollution.
Obesity is a disease because food, specifically sugary and bad for you (the body loves fat and sugar, it’s its freaking food sources and the only ones) specially in easy digestible forms is addictive. Much in the same way alcoholism is addictive in a physiological and mental way, though usually not as serious. If Obesity was not caused by food THEN WHY CAN IT BE FIXED BY CHANGING ONE’S DIET??
OMFG, not all vaccines are bad. You probably wouldn’t exist right now if it weren’t for the vaccines you got as a kid. Small pox, bubonic plague, polio etc those things STILL exist. You have zero chance of getting them because your body was taught to fight a small version of it off and you shower and have hygiene. That’s what a vaccine IS. I will say though that they are often not tested properly and can have some mishaps.
You sound a LOT like an Illuminati is nigh preacher. I agree the world is not roses and unicorns, but for freaking sake, really? Doom and gloom we’re all gonna die messages? The government wants us dead? I think you’re the one who has no idea what they’re talking about.
To put it super simply. If a government or corporation can’t make money out of something either short or long term, it’s probably not happening. Killing most of the human population would be a really REALLY stupid thing for them to do. However, making people sick, bad health slowly over time, not instantly racks in a TON of money, short and long term. Encouraging more children for more consumption does the same. Those all work together, not be design, but by the common goal being the same. Profit.
Please educate yourself on mental diseases. You show that you have no idea how they work. Specifically PTSD.
Also, most if not everything you mentioned has existed WAAAAY before vaccines, bio weapons or anything else. We just didn’t have a way to identify nor a name for it. You’re putting down medical science for no reason then to justify your misguided attempts and trying to make sense of the “evils” of the world.
And yes, HIV WAS DISCOVERED AND DOESN’T KILL. It deteriorates the immune system and can develop into AIDS. AIDS KILLS. NOT HIV.
Paying attention to one blog to answer all the worlds ills is extremely typical for a conspiracy theorist. It’s always this one doctor or scientist or person who has the answers. No actual research required, because anything that points to the contrary about you being 100 percent right has to be paid by the government to keep the sheep in the dark, right? That’s why there is no point trying to bring logic or peer reviewed science into a conversation with a conspiracy theorist.
If you didn’t notice, I’m REALLY hostile to disinformation like this. That was the most ridiculous read I’ve ever seen. Humans are healthier and longer living then we EVER have been in history. And yet because information on sicknesses and such exists for the public to see and for scientists/doctors to name and discover, now everyone thinks we’re doing worse then before. It’s utterly ridiculous.
I hope you realize that smallpox vaccine isn’t even generally available any more – I tried to get it for my children and the doctor said no go, even though he was pushing all sorts of other vaccines.
It’s reassuring to know that cancer sufferers are in such knowledgeable hands over at 30 Bananas A Day – I know I sure feel better knowing I can rely on them for solid health advice in my time of life-threatening health crisis-
My favorite comment on that 30BAD thread-
“Too much fat makes your blood sugar high, high blood sugar is what cancer likes.I used to have high blood sugar on a very low carb diet.”
<>
I guess eating all those bananas changes your metabolism…..
no, it makes you stupid as monkey sh*t (sorry to be so blunt…)
LOLOLOL OMG, just the stupidity hurts when someone says that fat increases blood sugar. Maybe, just maybe they meant high blood pressure? But the fact that they said blood sugar twice just destroys that glimmer of hope. Either they were not low carb, or they went so far the other direction that they got ketoacidosis in reponse to flushing out all electrolytes and not getting in any carbs on a low carb diet and instead eating WAAAAY too much protein, which turns into sugar.
That was gold, thank you for quoting that. The amount that people don’t research how things work is sad and hilarious at the same time. Mostly sad though.
Oh, and can we add to the list of vegans with cancer, Aveline and Michio Kushi, who were instrumental in bringing Macrobiotics to the US. Aveline died of cervical cancer, and Michio has been suffering with colon cancer since the age of 81. Macrobiotics is pretty much vegan with some fish-based broths and maybe a little fish or shellfish. VERY grain-based. I do believe those two were vegan, however. Another glaring failure to dodge the cancer bullet in spite of dietary restriction-
I watched an online friend die of breast cancer after going macrobiotic. I warned her, gently, that cancer likes sugar but she insisted. In fairness she was stage four and might have died anyway. But she certainly didn’t improve her chances.
Swedish Hospital in Seattle has been working with mycologist Paul Stamets (number 2 mushroom guy in the world) Fungi.com, on studies using Turkey Tail mushrooms with breast cancer patients. The results have been nothing less than remarkable! Even Paul’s mother was completely cured of stage 4 breast cancer. Her cancer was diagnosed in 2009 as the second worse case her doctor had seen in 20 years of practice. With the cancer spread to her liver and into her sternum, she had been taking 8 capsules of Turkey Tail/day. She is now completely cancer free.
I don’t mean to negate what your friend went through, Dana. I just saw a talk by keynote speaker, Paul Stamet’s yesterday at our college and wanted to get word out about the fantastic work that is being done with mushrooms, mycelium and fungi. Check out the TED talk by Paul Stamets–6 Ways Mushrooms Can Save the World.
Lion’s Tail mushrooms are showing to cure Alzheimer’s. You can get these capsules at Whole Foods. Lion’s Tail has been shown to eliminate the ameloid plaques found in Alzheimer’s patients.
Mycology appears to be a promising field in combating cancers. In addition to turkey tail mushrooms, maitake, shiitake, and reishi have some real promise. I cook with maitake and shiitake (and beech and crimini) regularly, and dunk dried reishi caps into broths. As a supplement, you can find good combo mushroom pills rather inexpensively as well.
Glad you posted this, Sue!
Denise! I was JUST thinking about you. Perhaps I had a premonition…Any debate on dietary health, pro-veganistas vs loose vegetarians vs locked-up vegetarians and your name pops into my head: “What would Denise say to this, she’s good at winning arguments with vegetarians…”
Very cool to see you dusting off the blog again, I’m on edge waiting for the release of your new book, along with many, many eager folks.
Rock on, Sister
Isn’t Sweden the land of Everybody Loves Butter? Didn’t they have a butter shortage recently?
So this may be part of their national conversation on fat. A salvo from the anti-fat brigade.
Norway had the butter shortage.
But, yes, Sweden has a love affair with all dairy products.
Don’t know why you’re anti-fat. You need at least some to survive. Maybe you’re anti-high fat?
hey denise – great job yet again – and a funny note about this search thang – we have not been active blogging at daiasolgaia due to big life changes, but on the stats we started seeing that each and every day – even with not too many hits per day, we would get someone searching “vegan gas problems” or “vegan flatulence” or some such search hit – now i am sure that they came desperate for a cure to their now horrible gut condition due to (mostly the raw) vegan issues – but they end up with our post telling them that nature is telling them in no uncertain terms that their diet is suboptimal (to put it mildly) – (Trolling for Farting Vegans and Nutritional Lessons Missed http://daiasolgaia.com/?p=2750)
… no immortal farting vegan searches yet, though….
as for your debunking of this yet-again inane study, how can these researchers, with any kind of scientific straight face – observational or no – get ONE food questioneer in 16 years and call themselves serious???
this is the very definition of ludicrous.
Brilliant post as always, Denise. My father (a physician) sent me the BMJ paper yesterday after getting excited about nutrition after reading Eat To Live. I then spent quite some time on a rebuttal that touched on many of the same points. If only I had waited a day you could have done all the work for me! Keep on crushing the book, and hopefully we’ll make it through the Mayan “apocalypse” unscathed. I know I freak out ever time my calendar ends on December 31st.
Ηi Denise. Very informative post, thank you. Another thing I ‘d like to point out is that two of the researchers, Lagiou and Trichopoulos are Greek. Trichopoulos, and especially his wife, are very big promoters of the Med diet. It is quite safe to assume that they could be biased for various of reasons.
Interesting that researchers Ronald Krauss and David Ludvig both found separately that high carb and high fat diets seem to have a negative effect on cardiac risk blood markers. Neither is a food fundamentalist, they just came up with similar findings they didn’t expect.
David Ludwig put his study data through the statistical wringer to support his well-known anti-low-carb views in the recently announced National Institutes of Health study. The markers you refer to are elevated cortisol and C-reactive protein (CRP). The elevated cortisol is mildly interesting, but the study period (4 weeks) is too short to permit *any* conclusion about the observation. The CRP information is just plain hogwash. If you look at the study data, rather than the author’s conclusion and media reports, you find that the low-carb diet reduced CRP by nearly *half* compared to initial measurements to below 1, a reading that’s considered healthy by any standard. To say something dramatic about CRP, the research team tortured the data, performing a rank transformation on it, i.e., tossing out all values below a certain rank, then compared the *trend* of the remaining data. Even then, the p value (.05) just barely met the test for statistical significance.
You are so funny! I love your writing and at age 25 with such wit. The way you make something so factual so readable is just fantastic.
I can’t believe that the only reason for these low carb diet studies is to discredit the diet, there has to be something more afoot….
Could it be these egos, in the guise of scientists, sense much danger from finding out they might need to take out all their beloved addictive foods?
The ego loves to be addicted, addicted to any substance or thought process (you know those stupid thoughts that go over and over again through you mind). Keeping us addicted is a great way for our ego to keep the status quo and that is it’s prime directive, “At all costs permit no change”.
Fogging thinking is a sure sign of too much carb eating and these scientists sure are foggy thinkers!
Cassie
http://alkalinepaleodiet.com/why-has-the-alkaline-paleo-diet-made-me-so-clear-thinking-with-such-an-even-mood/
Someone on a rabbit and insect based diet might also be high-protein and low-fat.
I like that Klaper article.
Yeah, and then there’s rabbit starvation.
I don’t actually know how “low-fat” insects are. It would depend on the insect. They’re probably high-cholesterol though (not that that’s a bad thing), as sea crustaceans are known to be.
I love your posts, you’re a genious!!!
I’ve been raw foodist and vegan for a lot of years and everytime I felt bad and reintroduced fish and meat and diary I started feeling better, but there was always that sense of guilt in me for the animals and vegan diet being the perfect fountain of youth, etc, but after having lichen plannus for the second time due to soy I decided that I’ve only one life and my health is more important than a diet.
It’s so true that vegans feel themselves superior than vegetarians and that raw foodist feel superior than anybody else in the world, a very disturbing thing has happened last year here in Italy, when a well known and respected nutritionist died of cancer, on some very famous veg. blogs people started writing things like: “He would be alive if he’s eaten less meat”, “He wasn’t a vegetarian so he’s dead, if he was a vegetarian, he’ll never have cancer”, this unrespectfull attitude has made me angry, there’s no respect for “others”, how can you respect animals when you don’t care about other people? And how can you define yourself compassionate, when you’ve demonstrated no compassion for this man and his family?
I’m so happy that people like you exist, you demonstrate respect fro everybody, I really like your attitude to science and eating choices.
I’d like to add that, unfortunately for her and her family, also Paul McCartney wife has died of cancer and she was a vegetarian.
I am INSPIRED! Beginning today (actually yesterday since I can remember that far back), I will keep a food log. Then, in 10 or so years, when the call comes out to participate in a study, I will be ready with accurate data. Yesterday I had sausage and eggs for breakfast, then too many pieces of pepperoni pizza for a late lunch/early dinner combo. Cabernet with that of course. Wait….do guys ever get called for these studies? BTW, my scale said I gained 2 pounds since yesterday. Must have been the egg yolks. Glad you’re back 🙂
L., if you look closely at this vegan movement you’ll see that it’s manipulated by some Hollywood extremely wealthy pre-school dropouts and similar corporate types. Last year, a wife of a CEO of one of the biggest companies in the world was bragging about being vegan and training her husband to be the same. These people eat humans before and after lunch, unlike the rest of us. I see this movement as a distraction from real societal problems.
Vegans just don’t notice the homeless, the unemployed, the uninsured, and spend their idiotic lives soaking and sprouting, posturing and distracting. I despise them.
Five bucks says that post gets deleted at 30 bananas a day!
still there
Denise I wish you’d make more videos, they save me a lot of time. When we’re hit by a “vegan” assault on the diabetic message boards trying to tell us that a diet of 90% carbs will “cure” our diabetes (along with any other ills) it’s so easy to just answer with a video. After all, they’re very long-winded and always have to have the last word on everything. They have an entire library of peer-reviewed (ha ha) studies and false facts to respond with(high fat causes blood glucose to rise!.) I did find one video by you, but more would save me so much time and effort.
Take pity on me Denise, make more videos. 🙂
“vegan” assault on the diabetic message boards trying to tell us that a diet of 90% carbs will “cure” our diabetes.
Looks criminal to me. Even I know that diabetics should avoid carbs.
Unfortunaterly the medical profession doesn’t know that. 😦
No kidding. It’s a shame and definitely breaks the Hippocratic Oath.
Umm, did anyone look at genetics? I’m convinced, that barring accidental death I’ll live a long, long time. I have the genetics for it. On both sides of my family tree, (including aunts, uncles and cousins) the median age of death is 97. I don’t know if it would matter what I ate (barring things like antifreeze and rat poison) I’ll probably make it to 97.
I have low blood cholesterol because I have the genetics for it. My mother, a Dane (In Denmark butter is a spice) ate a pint of heavy cream, a cup of full fat cottage cheese, a stick of butter and a 1/2 cup of premium ice cream EVERY DAY for the last 20 years of her life. She died at age 97 (cancer of the liver spread to the bone marrow) with low blood cholesterol, low blood pressure and a healthy heart. Something got to kill you eventually.
genetic predisposition of the human species seems to be irrelevant except to the paleo/primal leaning crowd- don’t even expect to see such a logical factor in any study like this…
You do know that low cholesterol is associated with cancer. Having a low blood cholesterol is not a blessing. The icecream might be a problem, but I don’t see anything wrong with the rest.
I would also want to increase my cholesterol to above 200, but inspite of a lot of ghee and meat, its not happening :-(.
Hi.
When I went LC about ten years ago, my total cholesterol dropped from 185 to 110 despite (more likely because 😉 of getting most of my calories from animal fat. A year ago, I started eating pork brains – 3500mg cholesterol/110g serving – 4-5 times a week. That brought up my TC back to 185, with a doctor pleasing HDL/LDL ratio. Pork brains also are a good source of phospholipid bound DHA, phosphatidyl serine and other brain nutrients. I experienced a number of health improvements including a rapid and lasting relief of a persistent overtraining caused arthritis in my shoulder and a 20% increase in strength despite having been lifting for years.
I know it sounds kind of radical, but is it not said that our ancestors evolved eating the contents of bones and skulls? Perhaps we are adapted to eating brains for over a million years. Oh, and I get them for only $1.90/lb.
Where do you buy them and how in the heck do you cook them!?
And, um, how do they taste?
Oh yeah, she was also fond of thick cut bacon, pork loin stuffed with prunes and twice cooked pork (from those Sichuan Danes)
Kaede my grandfather was the same way and lived to be 99! My cholesterol is perfect, even at the lower ranges they want diabetics to be in. It always has been without any effort on my part. Genetics plays a HUGE role in outcomes.
Excellent (and humorous) post as usual, Denise. You should consider a career in stand-up science comedy–that would be a new niche, wouldn’t it?
Always a pleasure to read one of your posts Denise… and I don’t think it is just a case of absence making it that much fonder 🙂
On the vegan super-powers theme: here is a clip from Scott Pilgrim vs. the World… http://www.youtube.com/watch?v=dLpCZ8g5uK8
Great video Frank. I posted it on my diabetes message board. Since we have to put up with them so often we might as well have a few laughs. 🙂
Denise, regarding your personal diet choices, I’m surprised you’re not on a VLC diet. Check out grc.com/health and the two low carb podcasts on those pages. Also the “Art and Science of Low Carb” books are great resources. According to a leading MD in bariatrics, there are probably only about 1 or 2 people in the entire world that are adapted to a high carb diet. I know your schedule must be full, but if you could find the time for the podcasts I think you would be convinced it’s underrated even in the paleo community.
Harley and Freelee of 30 bananas a day will not be convinced by your list of dead vegans. Their standard response for people with problems are: those dead people either did not eat enough fruit, or did not drink enough water, or did not sleep enough.
But then, I am not even convinced by this list. Except of the fact that it shows humans are moral.
” When I’m back here blogging more regularly, I’ll be covering a great many topics other than observational studies—I promise!”
What about observational studies on how non-human primates that are very similar to us eat in the natural habitat in the wild? Better to get the that priceless data before 1) their natural way of living is wiped out or 2) some huge corporation finds a way to manipulate everything to skew the results and forever change history.
I suggest that you watch the BBC documentary “Did Cooking Make Us Human” during which a group of human volunteers take up residence in a zoo for several weeks and are fed a nutritionally balanced diet of raw fruit and vegetables, comparable to that given to the chimpanzees — our closest relatives. Two things are observed: 1) there is never enough toilet paper in the loo for the frequent visits! and 2) there is not enough time in the day for all the chewing involved to ingest sufficient nutrition.
Comparing human digestion to the other great apes is facile. We took a different path perhaps as much as 4 million years ago.
That documentary would make me very angry because I have personally went on just fruit and small amounts of raw vegetables for 30 days and never experienced anything like that. Only if you came to it from eating a ridiculous joke of a diet would something like that happen. 1) Toilet paper? You don’t need any toilet paper at all. You will never be stinky like you are with a modern diet, NEVER, not one bit. Go play with the other children in the playground if you want, whether they call themselves “scientists” or not, I’m a serious individual. Some joke.
I’ll stay away from that documentary, I don’t want to watch **** on tv except maybe to give an insight into the pathological derangement in the world today (seriously).
2) You have to spend a long time eating to get all the energy you need… true. Multiply it by four or five if you’re getting your energy from raw vegetables. I love eating… I never ever say no to raw, nutritious, organic food if I even have the slightest desire to eat it. The second you start saying “no” to yourself for fruit is the second your entire system goes off balance, you won’t trust yourself anymore to eat when you’re hungry.
It still only takes maybe half an hour, maybe an hour of chewing a day. I don’t know, I’ve never timed it. Let me be honest with you, I drink a LOT of smoothies and fruit juices, the main reason being the huge amount of time saved. I believe that in this hectic, topsy-turvy world, it’s hard to find enough time and privacy to always eat properly. I’m eating lettuce right now, which is neither here nor there.
Another positive aspect of smoothies is that if in an “emergency”, you suddenly start to get quite hungry, you can get all of this juice in your system extremely quickly. I can’t tell you the amount of times they’ve saved me from eating something dreadful like cereal.
Emergencies??? Funny that… since I started eating LCHF (4 years ago) even as a diabetic I have rock-steady Blood Glucose… so much so that I can go all day without eating when the need arises 😉
Anyone can go all day without eating “when the need arises”, but it’s damaging. Just like anyone can go a minute without oxygen or can stand staying in freezing cold for a while. The fact that your body doesn’t say “hey, hey, I need to eat now!!!” shows a profound damage to your natural signalling and hormonal system.
Seriously? So you think that your pre-modern human primates, that lacked language or culture, ate three square meals every day? Man … its a miracle that the human race has survived at all 😉
and from your description it sounds like YOU can’t go all day without eating “when the need arises”… gosh you might end up eating some cereal :-0
“Seriously? So you think that your pre-modern human primates, that lacked language or culture, ate three square meals every day? Man … its a miracle that the human race has survived at all ”
They didn’t eat “three square meals a day”, they ate fruit intermittently throughout the day. This is the optimal use of energy… it doesn’t have to be converted, stored or hurriedly gotten rid of… a steady influx of readily available energy throughout the day. What protein is really is it’s like a “dirty fuel”… your body can turn it into energy, but it has hard work doing it.
“and from your description it sounds like YOU can’t go all day without eating “when the need arises”… gosh you might end up eating some cereal :-0”
I could do it, but I would get huge desires to eat and harmful stress hormones would show up trying to get me to eat…. yeah you’re right, I might end up eating some cereal. Not getting the desire to eat all day… sorry to tell you but that’s abnormal and not healthy.
Did I say I had no desire to eat all day? Please quote where I say that otherwise apologise for misquoting me!
As a Type 2 Diabetic I know all about Blood Glucose swings and the need to eat “urgent;ly” or else. Even my son became attuned to my mood changes and would warn me when I needed to eat something.
That has all gone away since I started eating in such a way that does not require constant “top ups” of food every couple of hours. Now if or when I find myself away from my home-cooked food or perhaps on a longer hike than I had expected, it is no big deal to wait and eat later.
I also fail to see how my ancestors living through the European ice-ages could have survived if they needed food every few hours… let alone where they would have found a ready source of fresh fruit in the snow and ice.
The simple and evident fact is that we cannot meet all our nutritional needs from just eating fruit…
but I see that I am just wasting my time with you so enjoy your lettuce 😉
Were did we get all that fruit from on the African savanna?
It grows on trees there, some fruits are growing all year around. Huge amounts of fruit come together in a tiny amount of forest canopy.
There is huge amounts of fruit there, all year around. Many primates still depend on it and it’s available there, some have too much, despite the idiot human currently destroying the vast majority of what’s there.
Padraig, there is no canopy on the savannah. It is grassland. There are some fruit trees but not many.
According to the scientists, that’s where we did much of our evolving as a species. It wouldn’t have been possible for us to have been eating fruit all day.
Me too and my husband too who used to be such a cranky puss if he didn’t get his food on time! Can miss a meal without any trouble at all and feel good. Such is the blessing of a LCHF diet
I’m just wondering a couple of things about you if you don’t mind my asking, and if you do mind, and don’t answer, I, and a lot of others here may find you hard to take as seriously as you’d like, because you do indeed sound very young-
1. What is your age?
2. What is your nutritional background – i.e. any formal education in human diet?
I’m having a hard time imagining that you are anything over 30. That much sugar – and if you don’t believe it is sugar my friend, you are seriously deluding yourself – is simply not healthy for the liver and pancreas, and has increasingly been shown to cause harm to all of your other organs as well. These changes tend to manifest themselves as a person reaches their middle and upper years.
If you truly believe that a juice or smoothie diet has never pushed anybody over the edge into being a full-blown diabetic, you better go back and do some research. Carrots, being a starchy veg, are the base of a lot of the smoothies and juices folks are drinking so many of these days. It has about as much sugar as the same quantity of many fruits, as do beets. Have you ever heard of the term “beet sugar”? Mmm hmmm. Make no mistake – smoothies are simply “mainlining” all that sugar, and dropping it into the lap of your pancreas to be dealt with all at once. Not smart.
Not to even mention how difficult it is to maintain any sanity about food choices when your appetite is constantly stimulated by all the blood sugar drops a person would experience from that quantity of sugar absorption. I would be hungry ALL THE TIME. One blessing of a low-carb/higher protein/higher-fat diet has been the appetite suppression. I am able to eat nutrient-dense foods in tiny quantities, satisfy my appetite for hours (allowing my digestive tract to REST,) and I have consistent energy throughout the day without all the blood sugar spikes and drops I would have if I were constantly stimulating my pancreas to release insulin!
You say a smoothie has saved you from eating cereal because you were having a food “emergency” – guess what? Most of us on low-carb diets never have “food emergencies” anymore. Why? Because our diets don’t stimulate much insulin to help digest our foods. No blood sugar, no blood sugar crashes, which is what is giving you those food “emergencies”.
It has been unarguably proven that the heart muscle prefers burning fat over carbohydrates for it’s energy. The obvious reason for this is that fat is a much more constant and stable source of that energy than carbohydrates. One can only prudently conclude that this must be true for the rest of the organs as well, with the brain preferring glucose, but adapting quite nicely to ketosis after a brief time.
“I’m just wondering a couple of things about you if you don’t mind my asking, and if you do mind, and don’t answer, I, and a lot of others here may find you hard to take as seriously as you’d like, because you do indeed sound very young-
1. What is your age?”
I’m older than Denise, the owner of this blog. I’ve been eating like this for almost ten years.
“2. What is your nutritional background – i.e. any formal education in human diet?”
None whatsoever. I actually tend to hold a prejudice against people with a lot of formal education in human healthcare, especially MDs. When an MD says something about diet, I tend to take it with a grain of salt. Being affiliated with such institutions just raises so many questions about motives and incentives, not to mention how they could have stuck to learning all the orthodox nonsense for so many years.
“That much sugar – and if you don’t believe it is sugar my friend, you are seriously deluding yourself – is simply not healthy for the liver and pancreas, and has increasingly been shown to cause harm to all of your other organs as well. These changes tend to manifest themselves as a person reaches their middle and upper years.”
A person eating a diet of all fruit will eat vastly less sugar than a person eating a “normal” diet with mashed potatoes, ice cream, cereal and meat. One apple only has something like 40 calories. That is a very small amount of sugar.
“If you truly believe that a juice or smoothie diet has never pushed anybody over the edge into being a full-blown diabetic, you better go back and do some research. Carrots, being a starchy veg, are the base of a lot of the smoothies and juices folks are drinking so many of these days. It has about as much sugar as the same quantity of many fruits, as do beets. Have you ever heard of the term “beet sugar”? Mmm hmmm. Make no mistake – smoothies are simply “mainlining” all that sugar, and dropping it into the lap of your pancreas to be dealt with all at once. Not smart.”
I never said smoothies were something optimal, I said they are a lot better than alternatives like cereal. I never made claims about smoothies being something you could drink as much of as you wanted, nor would I. However smoothies do satiate me quickly, like raw fruit.
“Not to even mention how difficult it is to maintain any sanity about food choices when your appetite is constantly stimulated by all the blood sugar drops a person would experience from that quantity of sugar absorption. I would be hungry ALL THE TIME. One blessing of a low-carb/higher protein/higher-fat diet has been the appetite suppression. I am able to eat nutrient-dense foods in tiny quantities, satisfy my appetite for hours (allowing my digestive tract to REST,) and I have consistent energy throughout the day without all the blood sugar spikes and drops I would have if I were constantly stimulating my pancreas to release insulin!”
I’m not hungry “all the time”, I can sometimes go hours without thinking about food. It’s usually after this going for hours that I suddenly wake up and get strong desires and have to either eat fruit fast or go for juice.
Your signalling system is abnormal. You might find it all fine and convenient and think it’s wonderful, but you’re actually causing subtle damage that adds up over time. This isn’t how dogs or other primates work. It’s like taking a pill to get your body to ignore the desire for food for hours at a time.
“You say a smoothie has saved you from eating cereal because you were having a food “emergency” – guess what? Most of us on low-carb diets never have “food emergencies” anymore. Why? Because our diets don’t stimulate much insulin to help digest our foods. No blood sugar, no blood sugar crashes, which is what is giving you those food “emergencies”.”
yeah, and it’s because your body doesn’t have a clue what it’s doing anymore and is taking all sorts of damage from several sources.
I’m not sure if we mean the same thing by food “emergency”. I didn’t think of it as anything like that dramatic, but I just noticed that when I got really hungry, sometimes I would start to eat multiple bowls of cereal, and sometimes even other stuff (never biscuits or nonsense like that though). I really hated these disasters and because I wanted to emphasize to myself how hungry I would get I began to think of them as a sort of “emergency”. Where I was liable to eat almost ANYTHING. It’s not like I was suffering or in desperate need of sugar, it’s just that it would require a ton of willpower and I personally have very little willpower. That’s when I realized that smoothies and fruit juice, with a little walking around, completely fixed these situations where I was in huge danger of eating non-fruit. But the reason I used “emergency” is because of the danger of me just caving and eating cereal, or sometimes a lot of tinned fish, or whatever’s there.
“It has been unarguably proven that the heart muscle prefers burning fat over carbohydrates for it’s energy. The obvious reason for this is that fat is a much more constant and stable source of that energy than carbohydrates. One can only prudently conclude that this must be true for the rest of the organs as well, with the brain preferring glucose, but adapting quite nicely to ketosis after a brief time.”
Nonsense, the body is in such desperate need for glucose that it in fact usually converts about half the protein it receives into glucose itself automatically.
“One apple only has something like 40 calories. That is a very small amount of sugar.”
http://nutritiondata.self.com/facts/fruits-and-fruit-juices/1809/2
one medium apple (182 g) raw + skin = 95 calories
including 25g Carbohydrates of which 19g are Sugars.
You see when someone spouts “facts” that don’t stand up to even the most superficial scrutiny, I have to question whether anything they write can be taken as credible?
Absolutely – especially considering the fact that many firmly diagnosed diabetics have been able to get off of insulin and reverse diabetic symptoms by keeping carbs at less than 30 per day. That apple sure wouldn’t leave them much wiggle room for vegetables, now would it?
I find it so comical that someone who claims that gucose is so necessary for the human body has never wondered how humans survived the ice ages, when there were absolutely and without question times when carbohydrates just weren’t available as a food source.
Yes, protein can absolutely be turned to fat but usually only does so in the presence of carbohydrate metabolization, or in cases of HUGE protein intake. Most experts agree that it is hugely unlikely that the average person is eating enough protein to convert it to fat – it’s unlikely because being such an nutritionally dense food, it’s uncomfortable to even eat that quantity.
Dr. Kruse advocates eating his “Big Ass Breakfast” which is based on 50 grams of protein eaten within 30 minutes of rising. His theory is that this helps to reset damaged leptin responses. Read the comments on some of his posts to see how difficult it is for most people to even come close to that much protein at a sitting. An egg, of which I eat two each morning for breakfast, is a measly 6.8 grams of protein. I’m not in any danger of having my body convert that 13 grams of protein into fat.
How exactly is saying: “something like 40 calories” the same as saying something as fact? Where did I say it was a “fact”? Indeed, I said the exact opposite… that it was an APPROXIMATION. And in fact, you don’t absorb all of the calories in raw food at all, so the net result is significantly less calories than whatever’s stated.
Granted I would have hoped for my approximations to be better than that. Of course you had to blow your own credibility by going over the top about it and lying by saying I had stated it as a “fact”, and suggesting things to others about my credibility, instead of giving clinical rebuttal and letting people make up their minds for themselves about how important an error it was when it was a clear approximation on a topic I’m not interested in. It wasn’t even about the calories, it was about the sugar.
You are “not interested” in the nutritional value of your food? and you think off by over 200% is a close enough approximation? Wow! Yes I am the incredible one for sure;-)
Pradrig has demonstrated his poor “approximation” skills in the past when comparing a fruitarian diet to an average American diet.
I’m done with you, because now we’re relying on semantics and mincing words.
It’s clear that you DON’T understand human metabolism very well, and as such are probably in over your head here.
I’m not sure many of the folks following this blog, and many others like it, are going to think your high-fruit diet is a good idea, or to give you much credibility, OR to have their minds changed by your (lack of) facts.
I think you should go back to the beginning, read some metabolism 101, read some of the experts, like Sisson, Wolf, Eades, Cordain, Eenfeldt, and others, some who are doctors and some who aren’t, but who rely on science that is NOT mainstream, and figure out what’s really true, ’cause your facts don’t add up.
Oh, and read “The Art and Science of Low Carbohydrate Living” by Phinney and Volek. So far, for me, it ranks up there with anything Taubes has written, and that’s saying a lot- it presents the FACTS about fat metabolism from two long-term, healthy low-carb experts.
And how is Lustig benefiting from telling people how to reverse the diseases that he makes money treating?? That particular line of reasoning was perhaps your most illogical statement of all. He is a pediatric endocrinologist, treating children who suffer from diseases of metabolism. HE UNDERSTANDS metabolism – why would he tell people how to bypass the pitfalls of metabolic disorders if he wanted to profit from their disease?
You are truly a warped thinker, dude.
“And how is Lustig benefiting from telling people how to reverse the diseases that he makes money treating??
What diseases? I don’t have any metabolic diseases. If you’re talking about diabetes or for people who’s metabolism and insulin response has been ruined by processed food, ie. anyone who’s been fat, then sure, maybe cutting down on “carbs” can be good.
I’m not one of those people who goes around saying everything is reversible. If a person has osteoporosis, then no it probably will not cut it to just eat fruit, you will have to artificially try things like supplement calcium. If people have messed their body up to such an extent that it cannot function normally then all bets are off.
A diet of almost all fruit isn’t bad for normal, healthy individuals, it’s only bad for people with impaired insulin responses.
Nobody would have an issue if Dr. Lustig and the paleos said that this is what they do to treat their disease and impairments. It’s this trying to push it on all of us and saying this is the best diet for humans… despite going against all our instincts and the exact opposite of what our ancestors ate and what we are evolved to eat.
“That particular line of reasoning was perhaps your most illogical statement of all.” He is a pediatric endocrinologist, treating children who suffer from diseases of metabolism. HE UNDERSTANDS metabolism – why would he tell people how to bypass the pitfalls of metabolic disorders if he wanted to profit from their disease?”
What??? Advocating low carb is Dr. Lustig’s and many others’ shtick. It is their hypothesis, their belief system, the reason they’re famous. They’re not going to admit that everything they wrote before was bs despite being so convinced that they were right about it. Like Campbell, they probably still believe in it themselves to some extent despite the huge questions being raised and the epidemiological and other data coming back showing that fruit almost always has a positive effect and that a lot of protein for example shrinks brains as shown in one experiment on mice (NOT a Campbell-style experiment, one using levels of protein that would be realistically consumed by humans).
See this is what happens when you only read the headlines or blindly accept what others tell you to think…. simply because it happens to fit in with your own disjointed view of the world 😉
Dr Lustig himself — in all his interviews presentations etc… speaks favourably about real whole fruit (although I doubt he is a fan of juicing or smoothies).
Where he has been most outspoken is against the massive amounts of soda being consumed, especially by children.
But hey… why let the truth get in the way of a good story 😉
And if you really can’t stomach watching that documentary perhaps you should try one which I believe is called “The Changing Ape”. It has footage of chimpanzees hunting (in groups) to catch monkeys and even using rudimentary sharpened sticks (spears?) to kill and then pry bush-babies out of holes in trees. As I recall: Jane Goodall has documented cannibalism among chimps.
It seems that even our closest cousins are smart enough to realise the nutritional limitations of an all plant diet 😉
FrankG, at first I found your smileys to be neutral or kind of cute, however I’m now starting to find them obnoxious. And I’m beginning to think that these smileys are in fact intended to be obnoxious and to mean something like: “well duh, don’t you sure feel dumb now”. So I’m not answering you anymore. Also you’re polite one minute, the next you’re losing it. You seem really edgy and frankly I couldn’t be arsed dealing with your issues and these mocking smileys after saying offensive things anymore. I already wrote multiple times about the supposed “hunting for meat” of chimpanzees in the comments section on this blog.
Let’s not forget the making of tools for “fishing” termites out of their nests! Another non-plant source of nutrition AND and an example of culture — the transmission of group knowledge from one generation to the next 😉
I am a regular reader of Denise’s blog but I must have missed your “supposed” comments about the fact that chimpanzees do hunt for non-plant sources of food including other mammals. Perhaps you could point me to them?
Chimpanzees do hunt for meat; it’s very well-documented. And as for fruit being available year-round on the savanna, this simply isn’t correct. Savanna is grassland with patches of trees, and most of these are acacias. Acacias produce fruit, sure, but they produce pods, being legumes, and are never fleshy and hypersugary. They’re also highly fibrous. Other fruiting trees on the savanna, like marulas, baobabs, monkey oranges, and the like, are seasonal bearers. Even at Gombe, which is forest and not savanna, there is a five-month dry season when little fruit is available.
If you are a vegan, you will have a tough time getting the protein that your body needs. However, eating large portions of meat is very inflammatory. There needs to be balance. There is a huge difference in eating only bananas and eating giant plates filled with meat. Denise, I know you like your fruit. Why is the discussion not about BALANCE?
Because BALANCE means different things to different bodies. My perfect balance is lots of meat, no – or few – starchy carbs, and and almost obscene amount of vegetables, but no grains or beans. I eat animal protein daily, sometimes more than once a day, and my numbers nicely reinforce that this is a pretty darn good way for me to eat. Everything is in low-normal range with little evidence of inflammation. And you can’t say it’s because I’m young either – I’m heading towards 50.
And who here is talking about eating “giant plates filled with meat” anyway? I must have missed that.
I’m sure if you read that somewhere here, it was more than likely tongue-in-cheek, as most folks who are not paleo/primal/traditional diet savvy seem to think that’s all we do-
I think your body would like you a lot more for it if you cut down your “almost obscene amount of vegetables” and ate a lot more fruit instead. Obviously you’re not going to listen to me when I say you would do a lot better to half your meat intake also. But there is no way your body can handle that amount of vegetables…. even though I’m a fan of vegetables… comfortably. I’m sure you must mainly cook your vegetables, isn’t that a dead giveaway that we are not really evolved fully for them like we are for fruit?
I actually eat most of my veg raw – only cooking that which is cruciferous, and lightly at that. I don’t care much for cooked vegetables. I feel pretty great eating like I do, as I’m sure a lot of other paleo/primal eaters will say, and I don’t seem to have any discomfort whatsoever from my diet. I’m not sure what you think could possibly be “uncomfortable” with it, but it’s not bothering me a bit.
I do eat some fruit, mostly berries and an apple here and there, but there is no way I would do a fruit-heavy diet. I’ve seen several friends, all at healthy weights and with no apparent markers, choose fruits over vegetables and become diabetic in their 50’s. I happen to think this smoothie thing that people are doing is diabetes in the making. It’s too much fructose entering the system too quickly, especially at my age – the body sees it as sugar, just like a lot of other carbs. There simply isn’t any need to have that much sugar in the diet, and I certainly wouldn’t do it on the suggestion that we evolved from fruit eaters.
i got your back Ann, your diet sounds very sound to me – and for my body type as well – and i don’t imagine that i our you are genetically sooo different than other humans. the idea that fruit is the perfect food in volume for humans is rather obviously wrong due to the constant slamming our insulin response takes. Kurt Harris has a great letter from a man who lived repeatedly over years with a settled hunter-gatherer tribe that was generally omnivorous, but dropped EVERYTHING when a large piece of game was obtained. when quiried about why they left hanging trees and trees of gorgeous sweet fruit while other food was available, they shrugged and walked on.
our bodies have serious metabolic problems with too much sugar of any kind – as opposed, for example, to too much salt which, although stressful for the organs involved, we actually have very effective salt-removal capabilities.
i’m not sure Dr Lustig is the new Ancel Keys for sugar as has been suggested, and i am not sure he is wrong about the fructose being toxic. it seems that we have a threshold for such “toxins” – but 30 bananas a day? only if i am a baboon–
Ravi, can you really still believe in all that anecdotal shit and test tube nonsense they’ve done with fructose after all of the evidence over the years that has been about using REAL fruit has always come out in favour of eating fruit? All of the other great apes have been shown to eat fruit in front of anything else. A baboon is a lot smaller than you for one, so he/she has less need for that amount of food. A baboon is also a much better hunter than a human, so one would expect the diet of a baboon to in fact do better with non-fruit than humans.
Mainstream nutrition has seen the error of its ways for quite a while now, there’s been a big reversal about fructose. HFCS has been found to cause a huge amount of damage that the same quantity of normal fructose will not, despite the previous mantra of “fructose is fructose is fructose”. And the amount of fructose and sugar in raw fruit is very little anyway. The only people who still continue to perpetrate this myth about fructose are hacks like Dr. Lustig, who have a huge financial incentive to keep going about it, and naive people like yourself who don’t understand nutrition.
And indigenous tribes can NOT be taken as a good example of what primitive man ate, in any way shape or form. They’re often just as much of a joke as a lot of modern humans in terms of diet… for example tribes that drink huge amounts of animal blood and milk and their health suffers tremendously from it. Taking tribes as an indicator for anything diet-wise is a complete fallacy. They’re not living naturally at all in a large amount of ways. If they’re using language, keep up weird traditions and teach their young, then they’ve already gone down the same bad road of modern humans.
“…huge amounts of animal blood and milk and their health suffers tremendously from it” — are you referring to the Masai? What health problems?
And do you really think we need to go back BEFORE we had human language and culture to lead an healthier life? Perhaps you would be happier swingin’ in the trees my friend… but not me 😉
I would be happier, and so would you. Then we might have an actual chance of humanity surviving, unlike the utterly hopeless situation we have now.
Umm no.. I already said that I would NOT be happier. Thanks
What health problems? …
and do please cite your sources 😉
Padriag, you seem to have problems “separating the wheat from the chaff” – and you are only a teeeeeny bit less annoying than Richard (he wins the most annoying commenter award by far). Your style is, however, similar – to be insulting, make illogical statements without citation or logical premise, and to be demeaning to any other belief than your own.
when diabetic, overweight aboriginals are taken back into the outback and shown how to resume their indigenous ways of gathering, hunting and preparing food, and they get BETTER (reversal of diabetic symptoms, loss of weight, better muscle tone despite a more sedentary life during the experiment), then i tend to sit up and take notice – and that is only one small example of what information/research/trials are out there.
as for availing myself to your further abuse – or Richards, i will not – bye bye and best of luck with your vegan/vegetarian nutrition.
The tribes that consume huge amounts of animal blood and milk (Masai) are very, very healthy while consuming said diet. After they retire from “warriorhood” and begin consuming a diet more similar to SAD, their health plummets.
“I’ve seen several friends, all at healthy weights and with no apparent markers, choose fruits over vegetables and become diabetic in their 50′s.”
Haaaahahaha, hilarious. You’ve given me a good laugh. Just for future reference could you give some sort of warning in the future as people can be at serious risk of choking from that sort of post.
just a thought here for anyone reading -does padraig sound at all like the infamous richard?/
maybe twins–
Nobody is going to listen to you bro, because it is perfectly clear that you’re clueless.
Science and truth meet in a very messy place and your like, “Come on in the temperature is perfect.”
“I don’t think low-carb diets are universally flawless, especially if food quality isn’t emphasized—and if a long-term study emerges that shows legitimate concerns, I’ll be the first to tell you about it (or maybe the 10th, given my blogging speed).”
“1.This study is observational—meaning it tells us nothing about cause and effect”.
1) Epidemiologic observational studies have shown that high LDL correlates with prostate cancer for decades, now see the same in clinical experimental studies.
The Importance of LDL and Cholesterol Metabolism for Prostate Epithelial Cell Growth (June, 2012)
http://www.plosone.org/article/info%3Adoi%2F10.1371%2Fjournal.pone.0039445
2) The same goes for eating meat:
How eating red meat can spur cancer progression
“Researchers at the University of California, San Diego School of Medicine, led by Ajit Varki, M.D., have shown a new mechanism for how human consumption of red meat and milk products could contribute to the increased risk of cancerous tumors. Their findings, which suggest that inflammation resulting from a molecule introduced through consumption of these foods could promote tumor growth, are published online this week in advance of print publication in the Proceedings of the National Academy of Sciences (PNAS)”.
http://www.eurekalert.org/pub_releases/2008-11/uoc–her111308.php
A tightly controlled metabolic ward study with human participants found NOC arising from heme iron in meat forms DNA adducts in the colon, a risk factor for cancer.
Click to access 1859.full.pdf
Numerous tightly controlled metabolic ward studies with human participants have confirmed that heme iron from meat significantly increases the production of cancerous N-nitroso compounds (NOC) in the digestive tract.
http://cancerpreventionresearch.aacrjournals.org/content/4/2/177.full…
3) I think you should inform your crew over the Inuit lifestyle. 2000 years, fossiles, died in their 20’s, atherosclerosis, osteoporosis, etc.
4) 3/4 of the known world were eating high-carb/starch, low-fat diets still couple decades ago, with very low levels of obesity, diabetes, etc. Maybe the problem is that the developed world has not been eating a high carb diet since the Great depression era.
Thanks for the laugh bro.
He wasn’t kidding.
You do not seem to understand that what you are posting proves nothing. BTW, at least one of your links don’t work.
Correlation != Causation is one of the absolutely fundamental aspects of scientific research.
What is the risk of dying from prostate cancer? How much exactly is the “increased risk of cancerous tumors”? What about studies which show decreased risks for other diseases?
You cannot simply pick and choose a couple of studies which show negative health effects and conclude that the overall health effect must be negative. It does not follow.
Paleo is actually low protein, but complete protein. Does complete matter? It is high saturated fat, also non-heated olive oil, and coconut oil is eaten either raw or used in cooking, something olive oil should never be used for, so I read, and it’s the only source of information I have, that is, reading. Any science I’ve read states unequivocally that Vegan and Vegetarians over 80% of the time are B12 deficient. It’s inarguable except those who want to argue just for the sake of argument. And we all know where B12 comes from, don’t we, meat and fish. Even some meat eaters are B12 deficient, but only 3% (approximately). Any what difference does it make whether we get B12 or not? Here’s the symptom list from Harvard, that rather impressive Boston, Mass university that impresses everyone in academia: Symptoms of B12 deficiency include memory loss, disorientation, hallucinations, and tingling in the arms and legs. Some people diagnosed with dementia or Alzheimer’s disease are actually suffering from the more reversible vitamin B12 deficiency. Measuring vitamin B12 in the blood is actually not the best way to determine whether someone is deficient. Blood levels of methylmalonic acid, a protein breakdown product, are a much better marker that captures actual vitamin B12 activity. There are other deficiencies that Vegans and Vegetarians experience, but there are deficiencies that rampaging meat eaters experience, too, but usually they’re connected to eating, drinking, and charbroiling grain fed meat, a little cancer to go around if one does that. But let’s just stick with two things, first B12, a very necessary nutrient (Oddly the only person I ever met who was deficient worked in a meat packing plant and he was a mess, but maybe he didn’t eat what he peddled, I haven’t a clue.) and animal protein is where you find it. Pure, at least to my way of thinking, if the food one eats fails to supply the nutrients I need to live, something is wrong with the food I eat. Is that fair? The second “thing” is Weston A. Price’s ten year journey in Europe, Asia (I think), and Africa. He wanted to find a healthy strictly vegetarian tribe/clan but failed to do so, and he had a bias, he truly wanted to find such a tribe. The closest he got was one that ate meat once a week. How much meat did they eat? I don’t know I only remember him writing they ate meat once a week. I read a very well researched archeological study that claimed using their archeological skills, that we started out as fruit eaters. Not too impressive in the physiological department, and one day, hungry and on the brink, they surmised, if starving, a rotting animal body, maybe of their own clan, odor wafted into their survival senses, and thus, it said, meat eating began. Now here’s a modern true story. A personal one. I was looking for kefir grains and found a source in Kirkland, WA from a woman who no longer needed them, it seems she found a new source of food, rotting meat, or should we say, fermented meat. This scared the heck out of me in a way, I thought, wow, I’m going to see a woman who eats rotting, er, fermented flesh. Human? Nah, it was beef as it turned out. I expected to see some rather grotesque creature with sharp teeth, sharp nails, fat and greasy, but what I actually saw was a lean, pretty woman who didn’t invite me in, just handed me the kefir grains, but did ask her what kind of meat she fermented. That brought a grin, the ferment thing. She said beef and she’d been doing the rotting meat thing for over two years and her daughters were so impressed by it’s affects on her they had started to eat the same way. To sum up the Paleo thing, it’s low protein, high sat fat, low carb, no fruits out of season, milk is controversial, lots and lots of vegetables especially green leafy ones, no grains, that is, wheat, barley or rye, or oats for that matter, water is the main liquid drunk, Celtic sea salt, and what it comes down to is, one simply buys the food and eats it without worrying about it since everything that’s stored in the refrigerator or cupboard is acceptable. No processed food except nuts and fermented veggies, and maybe I’ll look into the fermented meat thing. There was a tribe who claimed without fermented meat they lacked strength and something about being very much a man. We’ll leave the latter to our imagination. Apparently fermented anything is easy to and aids digestion.
You can also get vitamin B12 from eggs and dairy. I’m not claiming that a vegetarian diet is the healthiest diet (I do eat some meat myself), but B12 deficiency is much more of a problem for vegans than other vegetarians.
Anyways,
I think it’s rather clear that low-carbers and pushers of Kurt Harris “TC cholesterol of 300 is healthy” – diets are so off the track that the only fake asset they have is “debunking” observational studies, as if we wouldn’t have enough animal models, bile-acid studies, clinical trials, metabolic ward studies, surgical studies, etc to conclude that diet high in animal products and deficient in unrefined starches are detrimental to health. Sugar is just a poor scapegoat. Attacking observational studies is a symbol of holding tribe/sect together, together around pseudoscientific nonsense. Big posts around one or two studies is only what this “real food” sect has to offer.
“Death by the food pyramid”…lol
LOL, this is great. I have seen a couple of videos of yours, now. So you’re doing a “The onion” thing, just with diet as a subject. I love it, its great. Have you tried to send some of your golden comedy to larger outputs like cracked.com or heck…perhaps the very onion itself would appreciate this mockumetary style ‘science’ show. Good job. Keep it up.
Richard didn’t make those videos. They aren’t a joke.
You already used the “golly gosh this must be a joke” tactic on this exact same thing.
When a poster makes a statement like this that they know is false I lose all respect for them. Who are you trying to pull the wool’s eyes over? You’re a liar, at least I could have had some respect for you before as an ignoramous. You would try to put this little trick here and manipulate matters and consider yourself clever for doing this when you know full well that you are lying to say it is a “mockumentary”. You only mock yourself, clown.
Be honest, say what you mean and mean what you say. You should never use a lie or sarcasm to try to “prove” something.
Denise, I am much impressed with your clarity of thought, and your ability to find good informaiton. I was pleased to meet you in Dallas.
On this low carb study, though, the consistency of results may mean that the method may not have been all that bad.
Omission of confounding factors more likely is the weakness in the study.
Another is that they target “low carb” when there method would just as well have blamed it all on high protein, though neither carbs not protein had a wide range.
A real scientist tries to disprove his own claims; I don’t see much of that anymore, as everyone wants to prove someone else is wrong.
Keep up your good work
Ira Edwards (author of HONEST NUTRITION)
Ira – how can you suggest that “consistency of results” means ANYTHING when this diet “study” (i cringe to eve call it that)- the actual food eaten was tallied ONLY ONCE in 16 years? do you know ANYONE that was not food-obsessed (with some long-term maniacal diet dogma) that at the same food for 16 years?? it is patently absurd. the results are consistent cause the data is based on one set of purely observational parameters that were collected – ONCE….
ridiculous–
They do these “studies” because they are cheap. You can observe what fructose does to a human if you feed them controlled food in a controlled environment for a while. But that costs a lot of money and produces very few claims, usually only one. Not much food for the industry, the blogs, the magazines and the papers. Statistics on the other hand, is very cheap and you can produce lots of output. I wouldn’t trust even a 50% higher danger for disease A if it came from statistics and questionnaires. Most of the times, even a 100% wouldn’t be safe. There is a thing called ERROR that PROPAGATES and pollutes the output. Ask a mathematician about a rough error estimation in the claims of these “studies” and whether it’s safe to claim you see a 20% or a 30% here and there without even isolating key factors.
But these guys ignore the basics of science so that the press can cheaply get their headlines that get people to read articles and ads, and eventually buy product. The more the errors lead to contradictions, the more they are happy, the more you will read. Food A is good, then bad, then good again, then a tight, controlled and scientific study in vivo proves food A is irrelevant.
But advertising is not about causation either. Buying an expensive watch will not make you a star but you get to correlate (in your mind) with the lifestyle of the movie star that wears it in the ad. They don’t want talent or luck to kill the deal:)
I love epidemiology. Epidemiology has an impeccable track-record in getting everything right, starting from smoking.
“In 1940, I confirmed De Langen’s results . . . by the observation that in North China, coronary disease, cholesterol [gall]stones and thrombosis were practically nonexistent among the poorer classes. They lived on a cereal-vegetable diet consisting of bread baked from yellow corn, millet, soybean flour and vegetables sautéed in peanut and sesame oil. Since cholesterol is present only in animal food, their serum cholesterol content was often in the range of 100 mg. per cent. These findings paralleled the observation of De Langen that coronary artery disease was frequent among Chinese who had emigrated to the Dutch East Indies and followed the high fat diet of the European colonists (Snapper 1963, 284)”.
Cornelis de Langen: Diet-Heart Theory, 1916
http://www.epi.umn.edu/cvdepi/essay.asp?id=111
1) From the Framingham data:
“Under age 50 years these data suggest that having a very low cholesterol level improves longevity. After age 50 years the association of mortality with cholesterol values is confounded by people whose cholesterol levels are falling–perhaps due to diseases predisposing to death.”
http://www.ncbi.nlm.nih.gov/pubmed/3560398
2) Relationship of baseline serum cholesterol levels in 3 large cohorts of younger men to long-term coronary, cardiovascular, and all-cause mortality and to longevity.
“These results demonstrate a continuous, graded relationship of serum cholesterol level to long-term risk of CHD, CVD, and all-cause mortality, substantial absolute risk and absolute excess risk of CHD and CVD death for younger men with elevated serum cholesterol levels, and longer estimated life expectancy for younger men with favorable serum cholesterol levels”.
http://www.ncbi.nlm.nih.gov/pubmed/10891962
3) Ornish et al. demonstrated in an intervention trial that lowering LDL was associated with increased telomerase activity, which in turn is associated with longevity.
Click to access blackburn_and_ornish_lancet_2008.pdf
4) A meta-analysis of 108 randomized controlled trials of various lipid modifying interventions found that lowering LDL cholesterol significantly decreased the risk of coronary heart disease and all-cause mortality, whereas modifying HDL provided no benefit after controlling for LDL cholesterol.
Click to access bmj.b92.pdf
gawd richard you are an incredible bore.
Truth often times bores people.
I see you have golden comedy genius at large, Dean Ornish thrown in the mix now: is that not a bit dangerous so early in the show?. I mean that guy. Thats A material. I wouldn’t just bomb the show early on with him and the totally and utterly deranged collection of sideshow freaks at PCRM. I always go to their site every time I need a hearty laugh at what can only be described as science bashing. Kind of what youre doing here, only they are the elite in their field of comedy.
Please make an actual argument instead of just labeling groups and people according to how you view them. You need to acknowledge your own perspective of them as a perspective to have a meaningful discussion here. It does not seem that you do this. In other words, it doesn’t seem that you can or will separate “fact” from “opinion”.
There’s seems to be lot going on in terms of cancer regression and even reversal with vegan diets. Ornish has his landmark trial on the issue with pretty impressive results:´
INTENSIVE LIFESTYLE CHANGES MAY AFFECT THE PROGRESSION OF PROSTATE CANCER
“The diet was predominantly fruits, vegetables, whole grains (complex carbohydrates), legumes and soy products, low in simple carbohydrates and with approximately 10% of calories from fat. The diet is intensive but palatable and practical. In earlier studies most patients were able to adhere to this diet for at least 5 years”
http://www.ncbi.nlm.nih.gov/pubmed/16094059
@Richard: I’m sorry to say that your particular brand of of logic, reasoning and specious argument makes me think of nothing but this parody of advertising from Mitchell and Webb…
😉
Carbohydrate Restriction and Cancer
Fek yes!!! Not just Ornish. We get Eurgene from the sideshow of freaks. His mockery of …well everything sane, is very delicate. It must have taken him years to perfect the act. I just wish they would cut to the laughing audience more. But I guess its fair, its his show, so…
This is interesting research, but it seems dubious that the low amount of carbs is actually what’s preventing or helping to treat the cancer – it probably has more to do with eliminating refined grains (anything made from flour) and replacing them with vegetables and protein (not all low-carbers eat that many vegetables; I suspect that a diet higher in vegetables would have even better results). These videos were put out by nmsociety.org. On their own website, they link to this article:
http://www.foodconsumer.org/newsite/Nutrition/Diet/low_carb_high_protein_diet_may_help_fight_cancer_0617110701.html
A quote from that page:
“…although a low carbohydrate diet is better than a Western diet in terms of its effects on cancer growth, we do not know if the low carbohydrate diet used in the study is the best. Could a high starch, high vegetable diet, or a plant-based diet as Dr. Campbell calls it, be more beneficial than the low carbohydrate, high protein diet? More research is needed in this regard.”
Oops. I guess I need a space between them.
Carbohydrate Restriction and Cancer
@Richard: the mistake you seem to be intent on making is: treating the audience here as if we are mindless sheep — perhaps you are used to more receptive listeners when you preach to a crowd of avowed herbivores?
You will not get far here with an approach that seeks to tell others WHAT to think, nor will you impress with studies that are peppered with weasel words such as “MAY AFFECT THE PROGRESSION” or “could contribute to” etc…
Rather than trolling here with lengthy and pointless posts: I suggest that you could start a blog of your own which open-minded and critical-thinking readers can then choose for themselves whether they may decide to read, or give you any credibility, or not… as the case may be 😉
Please go easy on the vegans the poor fellows think they have discovered the immunity to all disease and the way to save the world. I know I was one of them, that why I tried to evangelize family and everyone one I meet on the wonders of veganism. That until I got sicker and my vegan friends keep dropping out because of the health problems. Which got me started in investigating diet thru real science and not vegan messiahs. But just so many careers, money and reputation are made around all the vegans fallacies that they just need to perpetuate them luring the next gullible person, just the same as the whole healthy grains and the SAD diet is a shame that there is so much misinformation floating around on diet and health.
Actually, I don’t think that Padraig and Richard are the same person . Padraig is like durianrider – just irrational wacko, while Richard is more like Furman/Esselytin etc – psuedoscientific zealots. What they have in common is that they are driven by a leftist radical vegan political agenda. I am not going to go easy on these vegans because they want to pass laws to force the world to eat like them. They are doing their utmost to take away my right to eat as I choose.
The Humane Society of the US raises $130M/year, spends $1.3M on animal shelters, and $2.6M on their “retirement fund”. And the rest? It is spent on propaganda and lobbying to pass anti-animal food laws. That is part of the reason for this increasingly pervasive vegetarian bias in the media. The three doctor/scientists featured in Forks Over Knives are all present or past members of the board of PCRM, a front group of the terrorist PETA.
If radical leftist/fascist politics are not resisted, we know what happens – massive deaths by famine, genocide, labor camps etc. Stalin, Mao, Hitler (vegetarian, BTW). These people need to be vigorously opposed in an organized way.
http://www.humanewatch.org/
What?? I’m not a vegan at all and never have been and never advocated it. The reason is because the great apes tend to get some animal protein and because some vital nutrients can be depleted from the food we buy in the shops. I have meat and fish at least once a week. I have thereby eliminated any possibility of being deficient in anything.
I’m not the one going to crazy extremes, you are. The vast majority of high protein people are unscientific, crazy, extreme, delusional, irrational, uneducated psychopathic zealots…. and they’re all fat, pretty much (yes, 12+ stone is fat for anyone under 6 foot 5).
Your behavior on this forum is anything but trust inspiring, Padraig.
You’re definitely deficient in things!
Except for all the ones from the Crossfit crowd who as a sport adopted “Paleo” more or less wholesale. And all the strength athletes who made the switch for training season…oh and the bodybuilders who adopted the fad and love it etc.. yup. fact bunch of fuckers the lot of them. Or you are out of your mind, your league and place.
The “Crossfit” crowd? Bwaaaahahahahaha. You actually believe all that marketing gimmick hype? Sweet Jesus, those things are for people who don’t know their left from their right, who ring up Psychic hotlines. I think they should be illegal, taking money from pathetic individuals.
“Crossfit” my arse. It’s a made-up marketing word. What does it even mean? Nothing, it’s a joke.
The only correct and optimal way to exercise, is the natural way. Walking, maybe running a bit sometimes. Carrying a little weights sometimes. I’ve recently been doing some hanging from branches of trees near me, imitating what the other great apes do all the time and our evolutionary ancestors did. I have felt my back getting slightly sore from it, but I know for a fact that it can NOT damage me since it is a perfectly natural activity. All those stuuuuuuupid contrived artificial exercises are for dummies. Studies have proven that moderate exercise is far better than “intensity sessions” and one leg over the other push stretch nonsense which if anything is just damaging. If you want to be flexible… eat more fruit, and become more thin, that way you will automatically flex yourself spontaneously as it will come naturally to you.
” Studies have proven” what studies? The voices in your sugar drunk brain?
I guess you would know psychosis. It certainly looks the part
“I think they should be illegal…”
I rest my case!
No refutation at all, I see. Crossfit alone destroys your laughably ignorant and baseless assertions. What’s next, are you going to be telling us that all of the success stories on MDA or Robb Wolf are actually full of pictures of near-vegans? That athletes like Romda Rousey are the same despite their public statements of eating a paleo way?
You are literally ridiculous.
I did “refute” it, I pointed out it doesn’t mean anything. It’s a made up word, it’s the name of a company. It’s not in the dictionary and god help us all if it ever comes to be.
Crossfit – the branding and merchandising of simple exercises… Idiocracy here we come. I never thought I’d see the day.
It is so utterly stuuupid, with such an incredible lack of understanding of anything in the world, any ideas or concepts surrounding branding or language.
Talk to me about a particular exercise if you want, do not talk to me about a company.
On second thoughts I’d rather you not talk to me at all. I don’t believe any of those studies are done in any way properly, I think they are ridiculous.
I would not be satisfied with any study claiming a particular group of exercises to be better than natural exercise we are evolved to do. It is too complicated for reasonable results to be gotten from such a study. Doing things as we are evolved to do them has many hidden benefits while doing things another way has many hidden disadvantages/perils. We only see a small fraction of what’s going on.
You’d rather live in your fantasy bubble than confront uncomfortable truths? “believe” that studies disproving your position just had to have been wrong, they just had to be!?
Regardless of your complaints of Crossfit’s branding, it is an extant community of people who largely eat and exercise similarly. They exist whether or not you dislike their blatant paleo lifestyle. And a google image search for Crossfit says all that needs to be said about your laughable claim that paleo eaters are all fat. Or look at MDA success stories, or Mark Sisson, or Ronda Rousey (recovered vegan).
This is a matter of science, not wishful thinking.
“You’d rather live in your fantasy bubble than confront uncomfortable truths? “believe” that studies disproving your position just had to have been wrong, they just had to be!?”
No, I just know that studies like that don’t exist. What are the studies even looking for… lean muscle? Lack of fat? “favourable blood profile”? But you can have too much or too little fat on any part of you. You can have too much or too little muscle. Most Americans are psychologically pushed towards saying that fat is always bad, simply because the vast majority of Americans have too much of it… oh and don’t get me wrong… they do!!! However these weird, unnatural exercises are only going to have weird unnatural results and cause imbalances to the human system. MAYBE we can say they help (since they may put the body in a more natural state), however they can in no way do better than natural normal exercise.
Also, we never get to see the “failed” studies about things like “Crossfit”. They are all thrown away and hidden. It’s a joke.
“They exist whether or not you dislike their blatant paleo lifestyle.”
Paleo my ass. What they do is not in any way paleo, it is a disgrace to the name of “paleo”.
Paleo man ate a diet very high in fruit, rarely ate animal protein and exercised in a natural way. Not one leg over under back and jump and let me see your arms… this is all gimmick nonsense designed for fools.
“This is a matter of science, not wishful thinking.”
It is NOT “wishful thinking”, it is the truth. And the truth means terrible things for people with the way the world is going, far worse than with your simple-minded model where we just put everything through a simple test.
Those tests are anti-scientific, they are meaningless. Evolution is science, these tests and experiments are complete junk. People think they mean something because they take the name of “science” and because the government is persuaded and cajoled into providing them with millions of dollars of taxpayers’ money.
A great comment, Charlie.
As I said earlier, I find them with their style, Orwellian, full of platitudes, cliches and slogans, and their aggressiveness truly irritating. Today, on NPR yet another Hollywood starlett was promoting the usual stew of New Age, veganism and recipe for peace. Who is she to preach to me and you? Is there a California separation movement? Eh, I am dreaming.
god, you people truly are utterly demented and deranged. Probably from lack of carbs to your brains and terrible cravings.
“Another positive aspect of smoothies is that if in an “emergency”, you suddenly start to get quite hungry, you can get all of this juice in your system extremely quickly. I can’t tell you the amount of times they’ve saved me from eating something dreadful like cereal.”
Terrible cravings indeed.. glad I don’t suffer from these any more 😉
FrankG, please do not fantasize that you’re anything like me. There’s a massive difference here in that I’ve always been thin while you’ve always been fat, am I right?
I said nothing about “terrible cravings”, just that I have very little willpower and almost never fight my desires. You’re the one who stated “terrible cravings”, by all means have fun with your imagination but you shouldn’t confuse your dreaming with reality.
Another massive difference is that I am eating a perfectly natural diet, apart from the occasional small serving of fried chips I allow myself (I have no idea why I do it really). The smoothies allow me to eat this way with more or less zero effort at all, while before I might get cereal.
Padraig-
Wow – now you’ve gone beyond embarrassing just yourself, I’M even becoming embarrassed for you…..
fog brain much, bro?
Rest assured that you are in no way involved in any of my fantasies 😉
You are wrong (again)… I have not always been overweight — not that it is any of your damn business 😉
I am also eating a perfectly natural diet 😉
When I used the word “cravings” above — much as when I quoted your words on “calories” earlier — I was simply repeating what you said 😉
In my world: hunger has very little to do with “willpower” and everything to do with nourishing my body what it needs.
So what are the health problems you claim for the Masai? Third time of asking BTW … AND I’d still appreciate verifiable sources because your word is NOT a credible source 😉
I also want Padraig to explain how we’re harming our bodies by “ignoring” our hunger signals?
Padraig said
“yeah, and it’s because your body doesn’t have a clue what it’s doing anymore and is taking all sorts of damage from several sources.”
What damage from what sources EXACTLY?
Do you have references, studies, or sources to back up that claim?
I find it strange that I would be so much healthier now than I ever was before if I’m taking “all sorts of damage from several sources.”
My body didn’t have “a clue” back when I ate so many carbs that I had foggy brain syndrome all the time, and felt like I needed a nap after every meal because my blood sugar soared so high.
Lower-carb diets aren’t just for people who have metabolic issues – lower-carb diets are also GREAT for anyone wanting to avoid them-
“I also want Padraig to explain how we’re harming our bodies by “ignoring” our hunger signals?”
Ann, your body has warning signals that it best change its environment or it will be put under harmful stress in order to do its essential processes, to keep homeostasis if you want to call it that. So if you go into the cold, it gets you to go to a warmer place, so it doesn’t have to work really hard and go under undue strain. My mom doesn’t feel the cold as much as I do, and she’s old now. I used to think that was a problem with me before, but I later came to realize that it’s her own sensors that are off. That not everything that happens to be convenient is a good thing.
If you somehow found an artificial way to never feel cold anymore, would you use it? Of course not (at least I hope you have more sense than that), because your body won’t know when to get into a warmer environment. You already stated that this works for food… that you somehow just don’t feel hungry all day. Well for me that is a sort of abnormal and suboptimal state to be in.
Sure, your body can find ways to surmount its hunger…. which is why people who stop eating for days at a time sometimes claim to have no hunger after a couple of days. This is a weird sort of famine mode your body goes into… where it doesn’t want to harass you with thoughts of food anymore. But guess what? This doesn’t mean everything is fine… your body is still starving, you’re just numb to the pain of it. Another example is people dying of the cold that can’t feel it anymore, or people in such blinding agony/pain and suddenly they don’t really feel it anymore…. the body shuts off that pain to give you a chance to think straight for a minute.
“What damage from what sources EXACTLY?”
The damage is done by it straining to convert protein and fat into energy for you to use. There are several metabolic processes that have to be gone through for this, or there is ketosis which also has problems. Protein is really like a “dirty fuel”… it can be burned for energy, but it’s not good.
This is why people who eat a lot of protein or fat have been shown to weigh less than people who eat high carb with the same amount of calories. “Oh joy”, says the overweight American…. and indeed for people who have fat blocking their arteries this may be a good thing. However unfortunately that energy has to go somewhere… it just randomly bounces around your body, metabolized in some non-descript ways, creating free radicals and toxins. There are elaborate theories on how metabolism is the cause of aging itself, and to have this sort of energy bouncing around in there and going god knows where is just not good. Do you know about “calorie restriction”? They are a highly serious group with oodles of scientific theory behind them… they advocate eating much less calories for a longer lifespan. I don’t go along fully with all their theories and philosophies myself, but they certainly make a lot of sense in some ways. If energy was so easily gotten rid of inside of you, why would the body ever allow itself to get fat? The body really has no means of getting rid of it, it just goes around chaotically inside you wreaking havoc wherever it goes.
“I find it strange that I would be so much healthier now than I ever was before if I’m taking “all sorts of damage from several sources.””
I never said you weren’t. But I bet you weigh less now and this is why you’re making this claim? Being too fat causes a huge amount of problems and can cause vastly more damage than eating low carb. That doesn’t mean low carb isn’t subtly damaging you.
“My body didn’t have “a clue” back when I ate so many carbs that I had foggy brain syndrome all the time, and felt like I needed a nap after every meal because my blood sugar soared so high.”
These carbs wouldn’t happen to include biscuits or cakes or pasta or soda or ice-cream or bread would they….? Those are joke foods and nobody on the planet should be eating them ever.
“Lower-carb diets aren’t just for people who have metabolic issues – lower-carb diets are also GREAT for anyone wanting to avoid them-”
Completely false.
Wow – you just really have no grasp of metabolism. Ketosis is an abosolutely healthy state to be in. It simply means that your body is burning fat – don’t confuse this natural, healthy state of metabolism with ketoacidosis, which is only dangerous for diabetics.
Why would our bodies convert and store everything we eat to fat for energy if that wasn’t it’s preferred fuel???? Can you honestly answer that with any logic whatsoever???
I have not lost a significant amount of weight – I do however feel better, have better numeric markers on my lipid and metabolic tests, have constant and, most importantly CONSISTENT, energy throughout the day with no blood sugar surges and drops, and I have enough of a reduction in food cravings and appetite that I am able to make good, consistent food choices throughout the day, and from one day to the next. My hormones are in balance, my sleep is improved, I’ve been able to discontinue the use of antidepressants, my blood pressure has normalized, and I just feel SO MUCH BETTER. There’s just no arguing with that anecdotal evidence for me.
I don’t happen to be one of those people that thinks we have to be thin to be healthy. Thin people drop dead of heart attacks and are diagnosed with type 2 diabetes ALL THE TIME, we just don’t hear about it because it’s so much more fun and interesting to point our nasty fingers at the fat kids.
When I’m hungry, I’m hungry, and I pay attention to those signals and eat – a VERY SMALL amount of food. I can do this because I am getting the nutrition my body needs, including enough fat, in a tiny, efficient, nutrient-dense amount of quality food. This means I don’t have to eat as often.
Do you realize that longevity enducing calorie restriction leads to fat burning?
In the study “Calorie restriction increases fatty acid synthesis and whole body fat oxidation rates.”
“CR mice oxidized four times as much fat per day as ad libitum (AL)-fed controls (367 +/- 19 vs. 97 +/- 14 mg/day, P < 0.001) despite reduced energy intake from fat. This increase in FA oxidation was balanced by a threefold increase in adipose tissue FA synthesis compared with AL."
http://www.ncbi.nlm.nih.gov/pubmed/19887594
Fat
Padraig, are you an idiot or just highly misinformed? Not one thing you mentioned is true or makes actual sense. You are just spouting absolute rubbish that is not only biologically possible but has absolutely no science behind it.
For starters, protein is used as a building block and also for repair to muscles, as well as many other things. If eaten in excess some protein can be turned into glucose – a process that also happens when your glucose levels need topping up on a low carb diet. It is not used for energy – that is the role of fat (or in your case the glucose from your carb substrates).
Energy does not bounce randomly around your body! This is a stupid comment and is one of many things that show your complete lack of intellgence. It makes me wonder whether you are just deliberately trolling.
And to comment on somethig eles you posted before: If you eat a meal every 2-3 hours because you start to feel hunger then that is definitely not natural. Hunger is the sign that your body needs more fuel to replace the macro- & micro-nutrients it needs to function. If you eat a protein/fat rich diet then hunger can be kept at bay for a long period of time because you have fulfilled the need for the required macro-/micronutrients, but if your diet is high in carbs, especially refined carbs, then hunger will come back quickly because these nutrients are missing. If you are feeling hunger every 2-3 hours then your engine is severely broken and you need to sort it out.
Not feeling hungry for a long period does not mean you are damaging yourself because your body is capable of feeding off it’s own stores of fat. This is what they are for.
“If eaten in excess some protein can be turned into glucose – a process that also happens when your glucose levels need topping up on a low carb diet. It is not used for energy – that is the role of fat (or in your case the glucose from your carb substrates).”
Good joke. Glucose is almost always used for energy shithead.
“Energy does not bounce randomly around your body! This is a stupid comment and is one of many things that show your complete lack of intellgence. It makes me wonder whether you are just deliberately trolling.”
It doesn’t randomly bounce around your body. “derp, that doesn’t sound like something a scientist would say derp”. I was trying to put it into easy words for you to understand. Energy that goes in and doesn’t come out raises your temperature or basal metabolic rate or does some other process to your cells which all points to damaging and aging, it can’t just disappear. That’s why calorie restriction helps so many organisms and probably humans to live longer.
“Not feeling hungry for a long period does not mean you are damaging yourself because your body is capable of feeding off it’s own stores of fat. This is what they are for.”
You are damaging yourself because of the stages the fat has to go through to get back to readily available glucose that is available from fruit from the start. This puts a tax and a strain on the system creating free radicals and oxidation effects. Nothing is free when it comes to metabolic processes. This may be all well and good for fatties who want to burn off extra fat and want this additional strain so more of their energy is used up, but normal people shouldn’t listen to that.
Don’t reply back and never call me an idiot again. I am clever, you are an idiot. Now I think you know who is more honest here.
“In my world: hunger has very little to do with “willpower” and everything to do with nourishing my body what it needs.”
Finally you say something I completely agree with. I hope the best for you in your future eating.
“So what are the health problems you claim for the Masai? Third time of asking BTW … AND I’d still appreciate verifiable sources because your word is NOT a credible source.”
Firstly, I didn’t mention the Massai, you did. I said people who drink large amounts of blood and animal milk, which I thought was an obvious fact. We hear a lot about the Massai, so it’s probably selective bias to concentrate on them alone (as opposed to other tribes who do terribly).
Yet the Masai people have a life expectancy of only 45 years despite their primitive lifestyle. Sure, lots of that can be explained away by malaria and all (diseases caused by civilization), but you can hardly point to them exponents of amazing health.
I never said anything like eating fresh, clean, organic, raw animal products is suicide, you would probably be better off eating a diet like the Massai than the typical American diet of today… probably .
Try these: http://www.bitterpoison.com/archive/masai-people-and-heart-disease http://wholehealthsource.blogspot.ie/2008/06/masai-and-atherosclerosis.html
The ONLY thing the Masai show is that you can eat a low carb diet and still remain thin. Frankly all your paleo “friends” are overweight or used to be overweight and despite their health claims their weight is the only thing they really care about. In fact, “health” and “weight” have become practically synonymous for some of those people.
The Massai aren’t known for their extraordinary health at all, it’s their trimness that gets the American overweight supposed “paleo” man’s hearts racing.
errmm… when I say “as opposed to other tribes who do terribly”, I mean hypothetical tribes that might do terribly. Even though it would be very difficult to imagine them eating such a ridiculous diet as a typical normal-weight American, if they have rituals and sacrifices and language etc. then IMO it’s possible.
ermmmm…. right… we should all be VERY concerned about “hypothetical tribes that might do terribly” just imagine how tremendously bad our health might be if we (gawd forbid) followed their example 😦
Yes I did ask you if the tribe you described were the Masai… you didn’t respond in either the positive or the negative. Who did you mean if NOT the Masai?
You are really on a different planet Padraig… I ask for verifiable sources and you offer this poorly written opinion piece from an affirmed vegetarian! For example… it starts off as if they know what they are talking, about even offering multiple spellings for Masai “The Masai (or Maasai)…” wow they do sound smart don’t they?!
…then it very rapidly goes downhill with spelling and grammatical errors which for me, are a clear indication that this person (much like yourself) has no clue what they are talking about 😉 …”The Masai (or Maasai) are a people in Kenia. They use lots of dairy products and there arteries show for it:”
Let’s try “Kenya” with a ‘y’ and “their” (possessive). As for “show for it” this is the kind of imprecise writing one might see in a tabloid newspaper, not in a peer-reviewed scientific journal.
I make typos in comments quite often but if I were presenting a learned opinion in my own blog I’d try using a spell checker at the very least — a fact checker would be ideal too 😉
As Ann suggested earlier, I really think that before you can even consider taking part in a reasonable discussion you need to go back to basics and learn more about metabolism… otherwise your comments provide little more than fodder for comic relief… but do please keep them coming as the more you write the more you reveal of your ignorance;-)
FrankG, I gave you two links. How about you actually read my posts properly and make valid criticism of them instead of fishing for spelling mistakes and alleged “imprecise writing”? Ridiculous.
Padraig it seem that even YOU can’t read your own posts intelligibly so why don’t you just give it a rest 😉
I asked for verifiable evidence of your stated claim (and I quote you directly) regarding “…tribes that drink huge amounts of animal blood and milk and their health suffers tremendously from it.” and you offered a poorly written vege-agenda-driven opinion piece and a post by Stephan Guyenet which broadly says that the Masai are healthy despite their diet — you see it really does pays to read BEYOND just the headline 😉
…Harley, you tosspot, is that you?
Ditto – I feel hunger — WHEN I’M HUNGRY — and not just when my blood sugar drops – because it never really does.
BTW, I am not primal and I doubt I will ever be. I am relatively speaking low-carbs, but I haven’t eliminated grains and dairy.
Sadly, “les extremes se touchent” and the radicals of the paleo diet are no different from the vegan radicals – the same style, the same techniques and similar idiocy. Yesterday, someone called “bread” “yuck” (sp?). This “yuck” is the cornerstone of the civilization we know, unlike some dangerously romanticized unknown past. Not surprisingly then both movements attract unhinged extremists who shouldn’t be encouraged.
“BTW, I am not primal and I doubt I will ever be. I am relatively speaking low-carbs, but I haven’t eliminated grains and dairy.
Sadly, “les extremes se touchent” and the radicals of the paleo diet are no different from the vegan radicals – the same style, the same techniques and similar idiocy. Yesterday, someone called “bread” “yuck” (sp?). This “yuck” is the cornerstone of the civilization we know, unlike some dangerously romanticized unknown past. Not surprisingly then both movements attract unhinged extremists who shouldn’t be encouraged.”
I agree Anna, bread is the “cornerstone of civilization”. Both literally and metaphorically, bread stands for all that humans have done in terms of civilzation. You could say that bread is the food that epitomizes civilization, and its effects mirror all the achievements man has made down through the years and everything civilization has granted for us today, with that I agree.
But therein lies the problem: Civilization is a horrible, morbid, terminal curse on the face of humanity. Everything that “civilization” has done has been to take us away from nature, and the environment we are perfectly designed to live in. The entire human race will be wiped out no question within the next couple of hundred years, if not through accidentally exploding the universe through a stupid physics experiment then the designer babies and genetically modified organisms are going to change humans so much that nothing like us any longer exists. Civilization is the cancer that is destroying not only humanity, but all life like ours. In this way, it is like bread.
If you’re still at the stage where you think bread is an okay food, then you really have learned nothing in terms of food. Even the so-called paleo people are far ahead of you. Bread… my god… are you really that clueless.
Oh, people, I don’t function on this level. I am out of here.
Fruits, smoothies.
I knew someone who during WWII was eating fruit and fruit only for a long period – working and eating fruit (grapes). She remembered this horror of constant diarrhea as well as the horror of fleeing in wet clothes during Russian winter and other horrors. What are you babbling about?
anna you’re retarded. Please leave the world alone and don’t spread misinformation that you have no clue about.
I’ve personally gone periods of eating almost nothing except grapes, I would eat 2kg to 2.5kg a day sometimes. Grapes are my favourite food. Other people into fruit have gone for weeks eating just organges and orange juice. You’re full of ****, full of it. Ridiculous nonsense.
You’re a joke honey, and you are doing tremendous damage by spreading lies over the internet, like a lot of other LC dimwits. Then it’s left to people like Neisy and I to try to mop up the crap people like you spout, (obviously Neisy does it millions of times better than me but I do what I can). Time for a new hobby I think.
OH MAN, FRANK — That hit’s the nail on the head! You are officially my favorite person of the day today!
I still want Padraig to answer my question about why the body stores EVERYTHING as fat if that’s NOT the bodies preferred fuel source?
Even all that healthy fruit will be stored as fat if eaten in excess – doesn’t that say something about what the body prefers to burn as it’s primary fuel?
I’m not getting any satisfaction on that one…
Is it not because if the body stored it as starch you would be in a very rigid/stiff body? like plants? Having a belly as hard as a tuber? 🙂 Still, if it stores fat I would expect the body to be able to use it efficiently.
“Science is the disbelief in the authority of experts.” –Richard Feynman
Well, I guess my disbelief in the value of this pronouncement makes me automatically a scientist. Where do I apply for a Nobel?
In the same vein I like these quotes fro Jacob Bronowski…
“Dissent is the native activity of the scientist, and it has got him into a good deal of trouble in the last years. But if that is cut off, what is left will not be a scientist. And I doubt whether it will be a man.”
and
“It is important that students bring a certain ragamuffin, barefoot irreverence to their studies; they are not here to worship what is known, but to question it.”
It seems to me that many, if not all, of the wold-view changing scientific discoveries were made by non-conformists.
Well, people, there is a problem with memorizing quotes. Seems to be an extremely conformist activity. I don’t know what is the age of participants, but aren’t we supposed to be able after the age of … to say something of value without the quote crutches.
LOL! I am of an age where I’m just grateful that I can memorize anything!
Good to hear from you again, Denise, keep up the good work!
Can’t wait for your book, get writing, girl!
I am seeing the beginnings of a religious (diet) warfare in these comments. I I think it is so sad we keep making the same mistake over and over again in history, “My god (diet) is the only real god (diet)”. We will never come to any real peace in the world as religious (diet) zealots. Tit for tat will only leave rifts and animosity. We need to step out of this way of communication if we are to become the evolutionary beings of the future.
I really believe Denise is quite special as she is not taking sides in any diet warfare.
Cassie
@Cassie: are you suggesting that we should not question it when others post unsubstantiated assertions? Just let them have their say? Ignore them? How would you deal with it? So far as I recall I have not been vocal about my own way of eating… I have been “accused” of being primal or paleo, while I have said no such thing myself. Personally I dislike such categorizing… as if I were part of a secret society or something. My choices are based on rational decisions, not religious zealotry.
Cassie, there is an additional problem – some gods are really ugly and people who promote them couldn’t care less about victims – nobody can live long and be healthy on some fruit diet or soy diet, but some people can make a lot of money promoting themselves as saviors, “discoverers,” “heroes” etc.
“Padraig, there is no canopy on the savannah. It is grassland. There are some fruit trees but not many.
According to the scientists, that’s where we did much of our evolving as a species. It wouldn’t have been possible for us to have been eating fruit all day.”
What do you mean “where we did much of our evolving”? We did the vast, vast majority of our evolving eating fruit alone. Baboons also live and evolved in the savannah and yet they have a large preference for fruit. It may be true to say that we are a bit more tolerant of non-fruit foods than the other great apes, but we’re still hugely more adapted to fruit!!!
And dangph, please say “according to the evidence”, not “according to the scientists”. The word “scientist” is a ridiculous term to throw around. “The scientists say this” is a meaningless statement. There is no band of elite unified people known as “the scientists”. Some of “the scientists” are full of crap.
So where is the evidence for your broad assertions?
I’m still waiting for you to follow up on your “…tribes that drink huge amounts of animal blood and milk and their health suffers tremendously from it.”
dangph! 😉 You haven’t even tried to explain what you think the “health suffers tremendously from it” bit actually means, let alone provided a verifiable source to back up this scaremongering tactic of yours. And this is discussing a people that are still around today… not some vague idea that you have about our distant past.
Although you do seem confused about your own stance on this point in a later comment where you wrote “…you would probably be better off eating a diet like the Massai than the typical American diet of today”
As above: even our closest cousins the Chimpanzees are evidently smarter than you seem to be, in their varied choice of diet… including several non-plant sources.
or maybe you have yet again slipped off into the fantasy-land of your “hypothetical tribes that might do terribly”. ermmmmm….
I think your brain is starved of nutrients. Your comments are senseless and pointless. You are very rude to others (and you started this trend… others simply responded to you) AND most importantly you are not impressing anyone with your complete lack of reliable input to this discussion.
Padraig has already stated that “I actually tend to hold a prejudice against people with a lot of formal education in human healthcare, especially MDs.”
Padraig’s post go from interesting to nonsensical as he never bothers to cite anything to back up his pronouncements. Having a discussion with Padraig is completely useless; unfortunately, he continues to fill this blog with his unsupported beliefs.
http://www.awf.org/content/wildlife/detail/baboon
“Diet
Baboons are opportunistic omnivores and selective feeders. Grass makes up a large part of their diet, along with berries, seeds, pods, blossoms, leaves, roots, bark and sap from a variety of plants. Baboons also eat insects and small quantities of meat, such as fish, shellfish, hares, birds, vervet monkeys, and small antelopes. “
http://www.blueplanetbiomes.org/savanna.htm
“A savanna is a rolling grassland scattered with shrubs and isolated trees, which can be found between a tropical rainforest and desert biome. Not enough rain falls on a savanna to support forests. Savannas are also known as tropical grasslands. They are found in a wide band on either side of the equator on the edges of tropical rainforests.
…
The savannas we are most familiar with [and evidently where humans evolved] are the East African savannas covered with acacia trees. The Serengeti Plains of Tanzania are some of the most well known. Here animals like lions, zebras, elephants, and giraffes and many types of ungulates(animals with hooves) graze and hunt. Many large grass-eating mammals (herbivores) can survive here because they can move around and eat the plentiful grasses. There are also lots of carnivores (meat eaters) who eat them in turn.”
you’re bloody brilliant. thanks for the list of vegans who died of cancer …
Yes, she is absolutely brilliant. I call her a “focused genius.” Probably, there is some redundancy here – geniuses tend to be focused.
“If men could only know each other, they would neither idolize nor hate.” – Elbert Hubbard. I don’t think it’s a compliment to be called a genius. I’ve been thinking of starting up a website about how small brains are utterly superior and large brains.. especially in typical humans… cause so much harm and destruction.
and I would talk about all the lies and myths about people with smaller brains and low IQs, such as being lazy or inferior or even bad for humankind, while the high IQ people easily get everything on a silver platter. Also the minute paradox of needing some small amount of intelligence to process and notice this fact about the world.
i agree 100% – that’s one of the major problems of our society: to overhype other people. invariably, they can’t live up to the hype – since we’re all just flawed humans, and then the reverse actions kicks in: shooting down previously touted “brilliant” or “genius” people. being aware of that – i was a little wary about posting that comment. but i still did it i guess out of habit … ?
let’s just say: i thoroughly enjoyed her dissection of another bogus “meat is evil ‘study’ ” like a couple of her other equally thoroughly researched and brilliantly WRITTEN articles.
i think that’s better … ?
Of course I do idolize her though for the amazing work she does and am a (online) student of hers. Not because of some inherent genius. Okay, I’ll quit making comments for a while!!
“Not because of some inherent genius.”
What the heck is that even supposed to mean???
“Oh yes the guy is an absolute genius — he comes from a long line of geniuses… except that every word out of his mouth is utter nonsense!”
Surely genius is measured on the strength of what someone says or does?
Once again I suggest you need to get some decent nutrients to your brain 😉
No, genius is very different. Yes, you can be a genius and talk utter crap. Everyone knows this, according to the typical meaning of the word genius.
Then you must be a genius 😉
Well, friends.
“Drinking milk is as American as Mom and apple pie. Until not long ago, Americans were encouraged not only by the lobbying group called the American Dairy Association but by parents, doctors and teachers to drink four 8-ounce glasses of milk, “nature’s perfect food,” every day.”
This how a certain well known chef starts his article in a well known paper and the well fed readers of this well known paper chime in the style; ” Yeah, big business, yeah, advertisements, yeah, yeah, yeah we don’t drink milk, etc.”
Just in case you don’t see a difference between this “charming” piece and Denise’s work, I’m offering my help.
Mr. Bittman and his well fed readers are not aware that the US isn’t the only country in the world. Unlike them, I know this for sure. I also know that there are people in other countries and believe it or not they’ve been drinking milk for many thousands years. Even more interestingly, some of these people praised their lands as that of “milk and honey.” Mr. Bittman and his well fed readers are clearly not familiar with the “text” I am referring to and anything else. Now, reread Denise.
Love this post. A similar list can be found on the ‘Let Them Eat Meat’ site at http://letthemeatmeat.com/post/3051392763/vegan-deaths-and-their-non-diet-related-causes – if a vegan ever dies, they are suddenly No True Vegan.
Doesn’t that just Burns you?
You didn’t mention a very famous person who was on a bizarre subset of a vegan diet (Steve Jobs), which I believe to be the main cause of his early death.
I also didn’t mention Davie Jones, from “The Monkeys” who died a few months ago while jogging. My understanding was that he was a strict vegan for many years, and a fitness fanatic, and yet, somehow he dropped dead of a heart attack, and an autopsy showed he had significantly clogged arteries… hmmmnnnn….
The main cause? Not the terminal cancer but the fact that he started eating a mostly fruitarian diet which he claimed to be doing far better on after he already had cancer?
Listen to me: You’re deranged. Steve Jobs died from cancer.
Yes the poor guy died of cancer but would he have died sooner or later (or even the same) had he taken the surgery when advised, or had he chosen to eat a different diet either post-diagnosis or for many years prior?
I guess we will never know the answers to those questions BUT so long as you you claim the right to speculate that his dietary choice had him “doing far better on after he already had cancer” I see no reason why another person cannot speculate that this was a poor choice; without you (once again) being rude to someone that you don’t know.
If you want to take part in an adult conversation, stop behaving like a child in the school yard 😉
Thank you for that. I had chosen to simply ignore Padraig since the rant had no value.
Steve Jobs ate a variety of suboptimal diets prior to getting cancer. Which very probably caused that cancer. About the only diet that he did *not* try was a very-low-carb, moderate protein, high-saturated-fat (mostly from animal sources, but coconut oil appears to be a reasonably healthy fat), low-toxin diet that probably would have slowed (or stopped, or — if early enough — prevented) the growth of his cancer.
What his “macrobiotic,” “vegan,” and “fruitarian” diets all did was give that cancer an abundance of it’s prefered fuel.
One clue that should be considered when evaluating the dietary advice coming from the “medical” and pharma mainstream is “follow the money.” If you are lean, healthy, and taking no prescription meds, then you are worthless to the mainstream “medical” and pharma industries. OTOH, if you are fat and chronically ill, you are worth a fortune. That’s why a cholesterol level of 230, which, by the AHA’s own numbers is associated with the *lowest* rate of all-cause mortality, is considered “high” — and “requires” treatment with a muscle toxin that has dozens of side effects, each of which “requires” yet another prescription pill.
FrankG, I did not speculate that, Steve Jobs said it himself. Once again: PLEASE actually read what I’m saying before giving an elaborate response to it. At least try to get the key points, god.
In fact, it was YOU who were/are speculating on whether he would live longer or shorter depending on his diet. I don’t know whether you’re really that blind, or whether you’re laughing to yourself at the utter ridiculousness of this situation.
And are we take take your word for it that this is what Steve Jobs said? Once again I see no reliable source… until one is forthcoming, it remains speculation or at best hearsay.
But it is ridiculous all right 🙂 this dream you have of swinging from tree to tree while eating bananas all day! The very idea that fruit is the perfect human diet! I’ve already demonstrated above that is not the case for Chimpanzees or even your much beloved Baboons…let alone for humans! So maybe you need to get some proper nourishment and see how much better your thinking becomes 😉
You say “even your much beloved Baboons”, but Chimpanzees are more frugivorous since they live in the jungle while Baboons live in the Savannah as you well know. You made this point about baboons and humans living in the savannah yourself. So you should say “baboons or even chimpanzees”
Try to pass an IQ test.
Keep it up honey you retarded, deranged, dimwit (just a few of your own choice words back at you)… 😉
Every time you comment you simply add to the point you made above about how “you can be a genius and talk utter crap.” 😉
uhm something else. How the hell can any news outlets post this horse dung when the comment section of the article itself is glowing with ire from people with titles such as ;:” nternist-Nephrologist, vascular specialist” …i dont even know what that means?! 😦 ..and “General Surgeon & Scientific Metodologist”, or how about “Advanced Laparoscopic and Bariatric Surgeon”. And the general message is; “FUCK OFF”, even if people with degrees put it nicer.
I was thinking … I think that vegans with their promotion of soy milk, soy cheese, soy burger, soy wine and soy chocolate are … agents of Ahmadinejad. Thank God for prisoners who have sabotaged this plot to kill the nation.
This is funny. A lady showed up on a health forum and announced that she knows how cure herself because she did research and read … “The China Study.” Ted Hutchinson explained to the lady that it’s probably not the best way to cure this particular disease and showed facts, charts and general information. No, the lady insisted, she believes in her God given path because she believes that “The China Study” is God given (something like that). They have been having this “conversation” for several days. One can only admire Ted. I would have ended this nonsense a long time ago with my favorite: “You are an idiot.”
Sorry, can’t resist: of which God are we talking in case of this vegan lady? Chinese, western, eastern….. ? 😉
You’re awesome! I loved reading this. Trying not to go to YouTube now..
Found yr site via Taubes/Attia. U have a way with words m’lady. Keep on keepin on when u find the time, thanks.
Talk about a come back post. You definitely made up for all the time you haven’t posted. I must hand it to you though, you really do have a way with words and can keep lengthy posts interesting.
On the longevity issue, here are some examples from my family:
Uncle, died 94 yo, living for many decades with a serious infection from the resistance, 80 years of smoking (rolled ciggarettes, no filters).
Grandparents from side A, Died 94yo and 93yo, one living with prostate issues, stroke in 94, other just had a stroke and died after 1 month, in 93. Very low calorie diet for decades. Living with undiagnosed heart problems for decades. That’s what they say. I bet they would live to be 150 if their followed the doctor’s magical advice.
Uncle, stroke at 82, full recovery within days, 85 now, will probably live to be 93-94.
Father, 81, no health issues yet. Very low labor for the past 30 years. Having his coffee, eating, drinking, sleeping. Heavy passive smoking for 8hours a day on average for 60 years or so. Very good shape.
Most of them drunk 2-3 glasses of wine daily, some of them smoked, all of them ate meat, lots of organ meat all the time in various dishes, pasta, legumes etc. Everything cooked and usually overcooked. They never heard about nutricion, or did any math about it. This is the true mediterranean diet, not the one you read about in books. And nobody realy does it anymore, not my generation at least.
Good genes probably, on the smoking deparment or perhaps something protective about the diet. Aging eventually gets you, but it’s funny to hear nutricion “experts” that recommend lifestyle and diet to others die in the 60s or 70s after all the work. We get to healthy 90s without even trying:)
I’m only 37. I feel like 20. I can’t remember when was the last time I had to visit a doctor. I was 11 I think and it was a virus. Then my girlfriend insisted I take tests when she heard I don’t like doctors much. The doctor was amazed on the heart/circulation/blood test department. Today, even people at my age have some degree of aging, even shades of metabolic syndrome and vessels problems. But me, none of tit. And no exercise whatsoever. No alcohol or sugar at all. No sodas, no sweets or ice cream. No smoking. Very few simple carbs. Good portions of meat, a little fish, lots of vegetables, a little fruit, massive amounts of tomatoes/ fine concentrated tomato sauce (greek cooking), lots of feta cheese. Everything is full fat of course. I believe all incredients are there for a reason. No processed meats. No processed/altered products really (besides cheese and pasta), 50g of almonds etc every day. Only extra virgin olive oil used. No more than 2000 calories a day just like my parents and grandfathers when they were not doing labor. No breakfast either. One heavy meal midday, one much smaller in the evening.180cm height, 70kg weight. I go for taste, just like my grandparents. I did food analysis on some typical days and I get about 50 to 200% of the recommended viatimin and mineral dosage every day. It’s close to 50% fat, 35-40% carb, 10-15% protein.
My girlfriend’s side is even better on the grandparents side. The diet is the same, but they got to 105yo some of them. Then we have her father. Heavy smoker, lots of sweets, lots of sodas, ice cream, chocolate milk, heavy sugar based breakfast, lots of stress, he is 52 and has seen tons of doctors, problems with stomach, ulcers, throat, gastro reflex, etc. His genes looked fine in both sides, but he is failing in his 50s. He must be doing something wrong.
What I’m really saying, is: Perhaps unprocessed food is the simple answer. If we avoid smoking and cut alcohol/sugar/fructose drinks and sweets we should be fine. There is no magical food. We don’t have to take unprocessed to the extreme. Cooked food isn’t bad IMHO. As long as you prepare it yourself with good whole incredients, it will be a good nutricious and healthy mix. Until I see some of the raw-diet, health-conscious, heavy exercise devotees live to be 100 or more. Then I will think if a few extra years are worth the trouble, because I really like eating anything I want and I prefer the cooked taste in everything, even tomatoes and peppers. True mediterranean diet gets you to 93-94 and we should even be able to improve that with what we know now. And sometimes, trying too hard to do what is supposed to be good might actually be bad. I find no reason to spoil a successful receipe for diet. Those of us who were lucky enough to live on a good climate where many sources of food of animal ,vegetable and fruit origin were available and widely consumed, should do what our grandfathers did.
Forsaken,
I like your comment. I see only a couple of things missing – stress and the more poisoned world now in general.
I am grateful for stressing the difference between the real Mediterranean diet and an imaginary one. I get sick when I hear babbling about no-meat Mediterranean diet.
Stress? Most of the them could fall asleep at a funeral. The war was bad and it shoock people. It’s hard to worry about the little things when you have gone through war and civil war, when you have seen crime in its worst form and have lost relatives and newborns from hunger. When things settled, you could do anything and make a living. Food was always on the table. Almost any business was a success and you could get a new job in a few days if you have 2 hands and 2 feet. Even the poorest families had very low stress. People are much less content today. The standards are up I guess. These generations were the equivalent of the baby boom generation in USA. 4 or 5 kids per family. That created lots of opportunity, and lots of need for labour, farming, housing, development etc.
This is just a limited point of view on mediterranean diet of the east but it’s better than nothing:
They didn’t eat much meat early in the century but they ate everything from the animal when they did. Every single part. And a lot of it. Some parts we cannot even buy legally today with the latest regulations. Many families couldn’t afford killing a large animal every few days, but they would eat massive amounts of milk and dairy which cost nothing but labor, and then occationally have meat for a couple of days. A chicken covered another day of animal protein. High ammounts of dairy by the standard we have today. Think 500ml of milk and 150g of cheese for each person. Protein was high even in legume days. Legume consumption were very high in other countries around Greece also. The amount of olive oil was also very high. A total of many tablespoons per person. There was no other type of oil. Some areas used butter or pork fat.
Due to olive oil and cheese, every single day had something of animal origin and was high in fat. They didn’t change their diet at all when they got old. The common knowledge was that kids, pregnant women and the elderly needed rich food, and people of productive age, the hard labourers also needed lots of extra bread. So it was extra carb calories for those who exersised. There was nothing vegetarian about the diet and those who could put meat on the table were considered blessed by fortune. I remember a documentary about people who lived far beyond 100 in Greece with good health. All of them mentioned they were fortunate to have meat and dairy. A few complained that they were not satisfied eating light meals with yogurt etc at the time of the documentary. They didn’t like the doctor’s advice in that department. Like I would have the nerve to give dietary recommendations to a 105yo lady!
Organ meats were considered top quality food. Something kids, pregant women and sick people should eat when an animal was slaughtered. Liver especially. A common dish was liver wrapped in suet, with garlic, salt and pepper, grilled.
The only time they went on a “diet” was in one day of the week or before Easter for 40 days or so. They didn’t eat meat, sometimes cheese and sometimes even olive oil (for a couple of days). This diet was generally normal in calories though, because they overloaded on legumes or ate green wild vegetables with lots of olive oil. Even when they appeared to eat very light meals, I would estimate there were above daily recommendations for their body weight. An exception is some days through the year, on which they could eat an estimated 500-800 calories total.
All families had trees they cultivated so there was lots of seasonal fruit. Don’t think of overconsumpion though. 2 apples or 2 oranges a day, 300gr of grapes perhaps. Most of the fruit was served to animals.
Red wine was standard. Each house had in their cellar 1) wine 2) olive oil 3) cheese 4) whole wheat flour. Wine was one of the four basics for survival. They made their own cheese, bread and wine. Very high quality bread. It would take 1 week without spoiling and due to hard labor consumption was very high. Rough bread, nothing like the whole wheat I see today. They didn’t like it at all though. They all happily converted to very low quality white bread and even considered it superior.
They believed that labor ruined health. Agriculture in those time was very hard on the bones. Many people from this generation had deformed spines and bad legs. By that I mean anatomical deforming but very solid bones at any age, men and women.
The typical food when they were working in the fields (think lunch break) was bread, olive oil, cheese, tomatoes, whole olives preserved in salt. When they were working they had 2 of those meals in a very long day. This was also the typical up to the 80s, for builders and workers in general. Sometimes anchovies were added, preserved in salt, and lots of oil on them also. When they didn’t work due to bad weather or holidays, they only had large 2 meals. Some didn’t even like having breakfast, others had just 150calories from milk.
Salads were very basic. Tomatoes, onions, cucumbers, whatever the season offered, nothing exotic.
Sugar was rare. I remember even in the early 80s, the only sugary food available in my grandparents house was a vanilla mix, a spoonful served under cold water. It consisted of glucose with traces of vanilline I believe. And very small portions of sweets. The typical “sweet” was boiled grapes or other fruit in syrup made from refined sugar. The portion was amazingly small, think 4 grapes in a tiny plate with a teaspoon of syrup. I can’t think of other sources of sugar in their diet besides a teaspoon in coffee, usually late in the afternoon, 2 hours after lunch or so. When season was low labour, they relaxed or slept for 1 hour in the afternoon. Then it was time for coffee. They only used sugar 3 or 4 times a year on celebration, to do traditional “sweets” of the season. Plus an occational quick snack using a little sugar and almonds, but that didn’t happen often. The acounts on this are interesting. My father’s generation believe that sweets were too much trouble and very expensive to prepare, but I can’t believe that. Sugar was cheap even in the 50s. My grandmother’s generation say that they didn’t have much interest in it. It was considered something for kids. An occational candy a relative brought to kids. They didn’t think it was bad for health, but they didn’t think it was good either. My grandfather used to say that sweets make you feel tired. On the other hand he thought that bread made you strong and helped in hard work, so they did put carbs into categories even at that time. Every generation want something and the previous one insist it’s bad from them:)
There was no sugary drink around. Nothing. No fruit juice or soda industry. No chocolate milk and no energy drinks. The grocery of the times didn’t really have processed food. Most families didn’t even have to visit a grocery, they grew everything they need, exchanged food and only occationally bought food.
The didn’t even put sugar in milk. They used a pinch of salt instead.
The typical food on a sunday or sometimes twice per week was boiled meat (with bones), most of the flavour came from marrow. This was served as soup, with lots of tomato paste or tomatoes if fresh were available. Overboiled meat was served on the side. Nobody found that interesting. They really cared about what was in the soup. There was the flavour, the medicine for those who were sick, the food for pregnant women.
A chicken once a week. Then another two days were usually high protein from legumes. Dried lentils, dried beans, etc. That leaves perhaps two days of fresh (green) beans with tomato sauce, boiled eggplant with tomato sauce, etc.
Occationaly they roasted meat instead of boiling, but using a wood oven was not fun, so they did that when they had to also do bread for the week. An occational celebration added another day of roasted meat every 15 days or so.
Fresh fish was available when logistics and preservation was not a problem. The boiled in water or fried in olive oil. Fish preserved in salt was very common. A quick meal in the evening.
What I discovered when I grew up was that they got massive amounts of vitamin C, through the entire year, even those who didn’t touch fruit. The basic sauce was a red tomato sauce, and two types were available, a thin one for boiled meat (and bones) served with small ammounts of pasta, and a thick sauce with fleshier parts of meat served with potatoes. The sauce was practically animal fats, vitamins from meat, potatoes and tomatoes and olive oil. And they ate every single drop of it, using bread. I remember my grandmother did that until she died. I haven’t met a person of her age who didn’t love that dish. She never needed any help with anything and her brain was fine till the end. The second sauce was made with lemon, eggs, and boiled meat. Very thick, served with rice in a soup. If I had to pick just one greek dish, it would be the heavy red sauce one. Boiled meat, heavy tomato sauce, feta or goat cheese, olive oil, and some bread. Very far from the fruit and vegetable notion of the mediterranean diet. If it wasn’t that, it would be legumes, beans or lentils in a similar sauce.
And lets not forget eggs. Grass-fed and sometimes corn fed according to season. Lots of eggs. About 8 each week for each person, more for kids. Eggs were no2 food for babies after milk. Poor families got cheese, olive oil and eggs “for the kids” from neighbors. Those living in the city were sent eggs “for the kids”.
A typical evening meal was “tomatoes and eggs”, some type of omelette that did not mix. Tomatoes boiled in their juices on a pan to remove their water content, then oil was added and scrabbled eggs.
They also prepared pies once a week, usually on a bread day. Pies were simple. Eggs, cheese, olive oil. Green pumpkin sometimes.
Boiled potatoes served with olive oil and cheese.
And chicken. Boiled in tomato/onion sauce. Skin included. Rooster was a favorite. Served with potatoes or pasta.
That was all really. A few incredients in great quantities. Very rich diet by modern standards, perhaps too rich. But they did fine on it. Then came white bread, sugar, oil other than extra virgin olive oil, margarines, low fat milk, modern processed food, cereal breakfast, western fast food. We started eating less cheese, eggs and legume. Young people move to strange diets based on juices, cereal, soft drinks and western fast food, women especially. Most women have problem with low iron, hair and nail growth. Today we are in the top three or four in obesity, directly competing with USA.
Forsaken, it’s kind of impressive actually that you wrote all this, but in terms of science it’s nothing but a heap of junk.
Wow, they “didn’t even put sugar in their milk” or their tea presumably. If you even consider doing that today then you’re not in a good frame of mind for eating well.
I don’t understand why you’re talking about them as if they’re some kind of model we should try to imitate, plenty of people have done all the wrong things and live far longer. Your genetics have a huge amount to do with it.
Why not rave on about people who smoked their whole lives and lived to 94?
Billy Bob and his brother and sister John and Amelie lived to 89, 96 and 92. Every day they drank large amounts of green tea. They smoked a lot, but it wasn’t the regular fags that are killing young people today… only the high quality cuban cigars and it didn’t do them a bit of harm. They had a small bit of meat on Sundays, and that was all the meat they ate over the entire week. They had a few biscuits and cakes every week, but it was the old more natural style of biscuits where you could really taste the oats. And they had only a few grapes at a time and never any honey… this must have been to protect themselves from postprandial glucose spike. Instead they had good old-fashioned bread and butter…
There is no evidence that any of what you’ve said helped your relatives in any way. Living to your 80s or 90s is very average and mundane…. if you told us that they lived until their 100s and 110s… then you’d get our attention. Or if you told us that they were jogging marathons before they died, it would be something. This is 100% worthless.
Padraig, relax and save the agression, it’s just information. It’s the reality of diet in a region of Greece from 1900 to 1970 or so. I hear a lot of misinformation when the topic is discussed, and that could only come from someone taking a very short vacation in the greek islands in the 70s.
And yes, obesity, and metabolic disease were very low in Greece and every other country. Enjoy your fiber-less sugars.
What amazes me is that you appear to believe that you know a lot about nutrition. I don’t know how many PhDs you have under you belt but the more I read on nutrition, the more I understand that we know very little. A friend who does have a PhD says that about 80% of doctors give bad advice on uric acid and choresterol. We do have some solid biology, we have some good in vivo work and we have some poor statistics many scientists do not trust. What we do know is that humans will do fine on a wide range of diets as long as it’s reasonably whole food, even when they do a few things wrong. The only exception is american diet recommendations after the 60s. There has to be something wrong with that because it’s improving nobody’s health, every decade is worse than the previous one. Something changed in the 60s and we have to fix it.
If you expect someone to offer you 110 years of good health, you will be disappointed or tricked into messing with your diet and lifestyle, you would be another victim ready to be exploited. That’s a wrong way to approach diet. That’s for snake-oil charlatans and their followers, cashing in on fear of disease and death, even death from natural causes.
Everyone would be happy with 90 years of good health in body and mind. You believe that’s a given today? Do you know many diet experts, fitness experts and billionaires (they can afford top health services and diet advice, right?) that get to a healthy 90? I see the opposite, most of those who recommended diets to us in the past 40years led their system to a relatively early failure considering the effort they put into it and even compared to the average person. All the best-selling authors and those who cashed in on our interest in diet. They were usually chasing ghosts, looking for superfoods, devil-foods, and panaceas. I have to give it to them, they believed in what they did. But what has belief got to do with diet or health? Sometimes the diet discussion appear to outsiders like discussion between religious fanatics. That can’t be a good thing.
I will have my wheat and milk, we have been eating that for thousands of years in the area and my system does well on it. I imagine that if you couldn’t take that in Greece, you were doomed from day one. That’s what diet tradition is about. Sometimes it’s a good starting point. I understand that someone from China from a relatively pure agricultural community will do fine on brown rice and could have intolerance for lactose or gluten. I wouldn’t feed an Eskimo tropical fruit or try to live on fish. Nobody is giving recommendations to anyone and searching for a super diet is IMHO a futile effort. My post was just my experience with the diet of my people. I’m glad you read it. Allow me to add that one should better approach diet from a logical and practical point of view, not with hostility. Any info and point of view is useful.
The diets of the past did well in many different parts of the world, very different diets and lifestyles. Those who didn’t die from easily cured diseases in their childhood or at any random age due to inferior health services, did quite well. I hope we manage to do well on our modern diet.
Peace:)
“I will have my wheat and milk, we have been eating that for thousands of years in the area”
Forsaken, this was my argument too. I have thousands years of recorded history of eating “milk and honey” and grains and meat, why should I suddenly stop eating this food?
Now, it’s possible that all this food has been modified, particularly in America, in an unhealthy way, but this is a different story.
forsaken – i first hesitated to slog though you rambling posts but when i did, i was, unlike the abundantly obnoxious peedig, impressed. a traditional diet that sustains healthy vigorous life – what a concept! – thanks for the input – there are precious few remaining traditional food stories as virtually all the planet is contaminated with industrialized food-like substances – thanks!
Uncommon sense in action! Good stuff here!
I’m late to the party, but these posts were fantastic Forsaken! Glad you wrote them. My background is from the Gaelic regions of Spain. What you ate, we also ate at home! Awesome food, and we never felt hungry or tired from it. However when I left home and started eating out with friends at restaurants and on the go, my health declined, I put on weight and developed many intolerances. After trying many diets, I looked at the versions mediterranean diets on the internet, but found that they’re so watered down that I wondered how my family could possibly have been so healthy and slender if we ate so ‘wrongly’, if you know what I mean. The elders in my family dismissed these so called mediterranean diets as rubbish, and after reading your post recalling your own experiences, I agree totally with it.
Forsaken, don’t ever tell anyone to “relax and save the agression” again. Never, ever, ever. It serves no purpose, assumes way too much, and is just a bad recommendation to suggest online. Never tell a person to not be so aggressive or angry, it’s a really perverse command that nothing good can come of.
Relax. You are being perversely aggressive.
this whole padriag thing is getting pretty creepy—
This is a great post. It’s a shame more journalists do not debunk naive believers of frequently hypocritical media portrayals on new nutrition based “research”. Thank you for being objective, and scientifically rigorous, as usual…
I do just LOVE your critical examinations of scientific research on nutrition. All those theories and studys out there are so confusingly conflicting to each other that often I got the feeling that choosing the healthiest way to eat is more like choosing a religion and starting to just believe in it, instead of being convinced by based on logical facts. (And to me – who was already born as a fully on “why’s that?” child – even believing in god is something I never managed, so how could I not question those studys out there?)
Also I enjoy every single paragraph of your (quite long) essays. You are a remarkable entertaining writer and I must admit – I cannot wait to purchase your book as soon as it is published.
I can relate, Healthninja,
Among other questions I ask there are these, for example: “Why do people brag and self promote all the time?,” “Why do people who never managed to believe in God often end up believing in Hitler, Stalin or anybody and anything else?”
Actually, I probably have the answers.
Love all your stuff. What reading can you recommend for sharpening up on how to read a scientific paper critically? Thanks.
Hey Paul, you could do worse than watch Tom (Fat Head) Naughton’s Science For Smart People presentation from the Low Carb Cruise…
This is weird. Don’t you need KNOWLEDGE (look up the word), just knowledge to begin with?
I despise this modern American superficiality/idiocy/corporate manipulation. To be a good person you have to smile. Do be a good employee you have to firm “handshake.” To read scientific or scholarly papers you need “skills.” Sure. There is a least one generation of absolute and perfect morons, smiling, shaking, strategically planning, team working etc.
I would recommend going to school and study, study, study .. “Sharpening” will come. Ah, intelligence is usually helpful too.
So much name calling, intolerance, and emotional personal attacks! Is this what meat eating does to a person? To be fair I have seen some of that in vegan forums, but not to this extent.
You seem to be confused. Padraig and Richard and company are vegans, not omnivores.
As I have repeatedly stated over and over, I am not a vegan or a vegetarian and have no intention of ever being one and I never have been one, ever. I think it’s a ridiculous and unnatural thing to aspire to. You see how a lot of you people just make up things and confabulate things in your own mind?
Actually, one of the side-effects of the eating disorder called veganism is impaired reading comprehension. Your confusion is a case in point.
Hi, excuse my mean english. I was reading some paragraphs by Denise, when a doubt appeared in my mind, a thought I would like to share with you; it’s not related to the subject in discussion (are low carb-diets killing sweden?) but I guess people who is surfing this site is reading the last comments, so I will put my thought here.
Ok, what about Carl Lewis? He states he was a vegetarian when competing at the top level. I would think: If an anti-meat diet can make a person weaker instead of healthier, either he was a superhuman capable to eat what he wanted and despite of that able to be the best, or he is lying to us.
What do you think about this fact?
people do all kinds of things eating all kinds of foods…if you like eating vegetarian and it’s agreeable to your physiology then eat vegetables. If it is a fact that Carl Lewis was a succesfull athelete and a vegetarian it dosen’t mean anything more than he was a successfull athelete and vegetarian.
I see your point, wyatt. I think like you. I will give the vegan diet a try; first I will see my physician, I am going to do a blood analysis before entering in the diet, and after 30 or 40 days I will make another analysis to compare.
Dellfiora – blood tests are a great way to get establish a baseline for down the road. Although I did not do this before becoming primarily a meat eater the test results 6 months after I began this new way of eating have prooved themselves to me 3 years later and the recent testing I had done. Not to mention qualtiy of life, energy etc. Not everyone wants to be or should be primarily a meat eater so do the best you can for yourself, there is no better way than to experiment and find a way of eating eliminates cravings, increases energy and restores health. Bon bon appetit’!
OK, let’s try again. Lewis was a VEGETARIAN. Your logic is incorrect. Actually, the life preceding a switch to VEGETARIAN diet, including pre-natal period, MATTERS. It takes, for example, some ten years to deplete B12. And yes, it matters what the mother ate and what a person ate as a child, etc. Try harder. Ask for better talking points.
anna, I think the best way to know if a person is able to improve his/her health on a vegan/vegetarian diet is just trying, of course with the assistance of a good physician/nutritionist. I tell you, I will give it a try for some months, and if I don’t get any improvement on my joints (I have pain in my joints, I tried Platelet-Rich-Plasma infiltrations but almost nothing happened) to treat my knees, then I will get back to eat meat and drink milk.
I read Denise’s critiques of Campbell’s work. They are very good. I
read B’s critiques of Denise’s critiques (B is a user from 30bananasaday.com). They are very good too. I don’t know who is lying, who is wrong and who is right, so I will take an action, of course in a prudent way.
I think some people is more suitable for living as a vegan/vegetarian than others; the same with another people, who success on a meat-based diet. That’s the most coherent thing in this subject, I think; that’s why scientists can not find the final truth about what is the best for human nourishment, maybe they think we are all the same as far as human nutrition is concerned.
Bye.
And why is it so difficult to understand that there is no such thing as vegan/vegetarian? And why is it so difficult to understand that if in human history not a single human group has been VEGAN, maybe, maybe, maybe humans are not meant to be vegans.
So, you have pain in joints and you want to go vegan? Good luck, good luck. You will need a lot of it. Vegans are notorious for having all sorts of arthritis.
Did you check your vitamin D level?
Why do you ask me about my vitamin D level? No, I didn’t check it…
Anna, I will try it for a limited time, in a controlled way. If I see any sign of weakness or a drop in my blood analysis, don’t think I am mad… I will get back to the fruits-vegetables-meat-milk diet.
I will go on this diet if I see results from it. Another thing: look at veganbodybuilding.com. People on the site look pretty healthy.
Another thing… what about you? do you have knowledge about nutrition or something like that?
So, you don’t know what your level of vitamin D is, you don’t want to check the connection between veganism and arthritis, but you just look at pretty pictures.
Hmmm.
BTW, I am not telling you to drink milk.
OK, Dellfiora, let’s go.
Check your vitamin D… now, immediately (you’ll be better off than looking at pretty pictures).
Start reading …. maybe here (an easy version):
http://www.livestrong.com/article/381986-paleo-diet-and-arthritis/
I myself am not paleo, but relatively speaking low-carb omnivore.
http://www.livestrong.com/article/457720-vitamin-d-causing-joint-pain-arthritis/
It can take as little as one month for some people to deplete their B12, although most store 3-6 years’ worth. 10 years is an outlier figure, for those with the most efficient recycling mechanism. It takes 90 days of intensive supplementation to rebuild the stores. After a major health crash caused by a short vegan period following nearly 2 years of ovolactovegetarianism, it took weekly IV transfusions of B12, alpha and gamma globulins, and a cocktail of vitamins and minerals, over several months, tapering off over a year, to get me functioning again.
Being a Vegan is not easy. But they all have their own way of staying healthy and I respect that. But we must also know that it’s not always the right way of living a normal life if you can’t accept someone who is not a Vegan.
You know …. this is tiring.
THERE IS A DIFFERENCE BETWEEN BEING A VEGETARIAN AND A VEGAN.
It’s dishonest to shift from vegetarian to vegan (and back) when it seems convenient.
Again, why do I bother?
BTW, can someone translate what Kimy is saying into normal? I mean from some Orwellian into normal? Are all vegans propagandists?
Lock them up.
Hey, I’m 42 – and still young! LOL. Will get younger still, now that I am going to add the proper amount of carbs into my diet for my non-stop activity.
These is a proper veganism and vegetarianism and wrong one:
http://www.diseaseproof.com/archives/debunking-diet-myths-weston-price-take-your-pseudoscience-elsewhere.html
Please, read all comments under the article.
“And, but the way, I call these people veg-junkatarians, because when you look at what British vegans and most vegans and vegetarians eat, it is mostly nutritionally barren grains and processed foods.”
But there is no proper low carb diets, high meat at all :
http://aje.oxfordjournals.org/content/95/1/26.abstract
http://discovermagazine.com/2004/oct/inuit-paradox/article_view?b_start:int=1&-C=
“On a truly traditional diet, says Draper, recalling his studies in the 1970s, Arctic people had plenty of protein but little carbohydrate, so they often relied on gluconeogenesis. Not only did they have bigger livers to handle the additional work but their urine volumes were also typically larger to get rid of the extra urea. “
Andrew, I would rather have a bowl of muesli with milk thrown over my face than read an article that says it’s “debunking Dr. Weston Price”. When the title itself is obviously horse crap then you know you’re in for a ride. Dr. Price did a lot of good, honest work and had a great book. Only someone with some sort of problems would deny this.
I’m a supporter of a 90%+ fruit diet, but talking about “debunking” the good Dr. Price is just absurd nonsense. “debunking”… most of Dr. Price’s points are about the degeneration of people in the “civilized” world due to their diet.
“Dr. Price did a lot of good, honest work and had a great book. ”
I read his book it is available online. It is not scientific work, it is rather a tourist notes.
1) WP judge health of people only by their teeth which is complete wrong. You can visit places in present day rural Africa where 50 or persent of population have AIDs and where you can hardly find person older than 50 and they have very good teeth. And this is only one example.
2) WP does not describe what king of physical activity, how many calories objects of study burned in everyday activities.
http://bjsm.bmj.com/content/44/2/121.abstract
3) He does not describe what exactly and which amounts of every food was consumed by objects of study.
So his book contains no data which can help to build any for any diet .
So, please read all articles.
“I’m a supporter of a 90%+ fruit diet”
It is a madness.
I wonder what happened to the hedgehogs after this photo? The fact that a hand is holding them like that in what is probably a kitchen is not an encouraging thought. Probably went right into the pot for some exotic dish. 😦
Eating Lots of Carbs, Sugar May Raise Risk of Cognitive Impairment
http://www.sciencedaily.com/releases/2012/10/121016103411.htm
“A high carbohydrate intake could be bad for you because carbohydrates impact your glucose and insulin metabolism,” Dr. Roberts says. “Sugar fuels the brain — so moderate intake is good. However, high levels of sugar may actually prevent the brain from using the sugar — similar to what we see with type 2 diabetes.”
Low Carb reduce and Intermittent Fasting Reduce the growth hormone/insulin-like growth factor-1
Starvation Hormone Markedly Extends Mouse Life Span, Without Need for Calorie Restriction
http://www.sciencedaily.com/releases/2012/10/121016103411.htm
FGF21 seems to provide its health benefits by increasing insulin sensitivity and blocking the growth hormone/insulin-like growth factor-1 signaling pathway. When too abundant, growth hormone can contribute to insulin resistance, cancer, and other diseases, the researchers said.
FGF21 is a hormone secreted by the liver during fasting that helps the body adapt to starvation. It is one of three growth factors that are considered atypical because they behave like hormones, which are substances created by one part of the body that have effects in other parts, the researchers said.
“Prolonged overproduction of the hormone FGF21 causes mice to live extraordinary long lives without requiring a decrease in food intake. It mimics the health benefits of dieting without having to diet,” said co-author Dr. David Mangelsdorf, chairman of pharmacology and a Howard Hughes Medical Institute (HHMI) investigator at UT Southwestern.
Correct link;
Eating Lots of Carbs, Sugar May Raise Risk of Cognitive Impairment
http://www.sciencedaily.com/releases/2012/10/121016092154.htm?
Charlie, people who eat 90-100% fruit don’t eat a lot of “carbs, sugar”. The amount of “carbs, sugar” they eat is a tiny fraction of the amount of the people that suffer any form of impairment from them eat. People who eat 90-100% fruit generally only eat about 1500-2000 calories a day, while people who are fat eat 3000+. People who eat 90-100% fruit eat more percentage wise, but vastly, vastly less overall.
Typical confusionist, trying to post a study about high GI/processed foods and pointing it to fruits. Utter nonsense, are you Mingers alter-alias?
Fruits have cellular walls which prevent you from absorbing the sugar all at once, unlike coca-cola for example.
About the immortality thingy: I wondered if there are any LONG TERM low carb people over the age of 80. Just wondering.. Please answer somebody 🙂
no, there isn’t.
Great post on human nutrition, thanks for sharing
Denise, the worlds oldest living people were all life-long chain-smokers. Should we all start smoking now too?
http://www.forces.org/static_page/oldest.php
http://www.forces.org/evidence/hamilton/other/oldest.htm
Worlds oldest low carb dieter? non-existent
Denise Minger fails to realize that the accomplishments of man are measured in accomplishments of mind rather than length of life. (low-carbers lose in both of these btw)
Leonardo DaVinci was vegan for one and I could name many more, and we can rest assured that many more were high-carb as civilized man (not the ape looking Masai) has been for thousands of years.
Low-Carb geniuses? If you consider shirtless book peddlers and Minger’s China Study debunking to be great innovation: you might consider living amongst the utopian Masai tribe (who haven’t invented anything in over 6000 years, have building skills comparable to that of a beaver, and have the average mental capacity of an 11 year old from any civilized culture.)
Ah, irony
> Denise, the worlds oldest living people were all life-long chain-smokers. Should we all start smoking now too?
>Leonardo DaVinci was vegan for one and I could name many more.
Should we all start eating vegan now too?
“Denise Minger fails to realize that the accomplishments of man are measured in accomplishments of mind rather than length of life.”
Measured by who? “accomplishments of mind” is a very dangerous idea to be throwing around as being the “accomplishments of man”. I’ve read stuff from sick-minded eugenicists who also think that “cultural achievements” have some sort of mystical value and inherent worth. In other words, that humans should start becoming slaves to creating “achievements” for their own sake, not even pretending it is for humanity. SICK MINDED NONSENSE.
This is a great blog!!! And has helped me a lot… recently I came across a few videos on youtube and I would like to share them here and like to get your opinions on them…
Please let me know what you guys think…. I would love to get your opinions
Great read, Thanks for sharing. This Raw Food Diet Change my Life.
I have been following protein diet for 1 month then i took a gap of 1 week in that i followed low carb diet.. then again for one month i followed protein diet… i achieved my targets.. now could any one help me with what to follow now to maintain my wt?? Suggest me with a good diet plan that wouldn’t cause bouncing back of my previous weight….
Moderate intake of food will always be the best way! Exercise and proper diet can never go wrong.
Denise, having unfortunately bought this book recently and actually been quite aggressively refused a refund due to its weakness, I was wondering what you made of Freelee and Go Fruit Yourself?
http://www.30bananasaday.com/FreeleesEbook
Having looked around the 30 bananas a day forum it seems to be full of people who are struggling and not thriving, and certainly not overcoming issue such as candida which was my initial interest in the approach.
Hi, Can anyone please tell me what is the minimum fitness level required for flying abroad to countries like sweden, finland?
Yo I didn’t make it past the human animal hybrid video.
What the fuck is that all about?
lol
protein are amino acid and most difficult to digest and utilizes energy from fat or carb. and if u intake less carb or fat then protein will will use your existing body fat to digest and that how body fat is reduced and your weight.
You are sexy
what a horrible lot of people there are in the world, nasty people write nasty comments. whay donlt you all shut up
Denise Minger’s latest lecture ends with “Ditch government advice and look at what healthy populations are doing.”
Well the Wilcox data on the Okinawan’s eating habits of 1950 has them eating 0 eggs, 0 dairy, 0 meat, 1% fish.
Good advice.
^ the available data on the New Guinea Kitavans (who have the highest @birth life expectancy of any known hunter-gatherers) has them at:
70% of calories from carbs, 20% from fat, 10% protein.
They, like the Okinawans, eat 0 eggs, 0 dairy, 0 meat, negligible fish
As I remember from the Blue Zones work by Buettner, Okinawans eat eggs, though never more than one a day, that they eat pork simmered in broth with sea vegetables, and that fish is by no means unknown in their meals. The Kitavan fish intake is not described as negligible by the researcher, Staffan Lindeberg, who studied their diet.
Lindeberg said something very interesting about the Kitavans: that less than 0.2% of their diet is Western. That is, the Kitavans do not eat industrial seed oils, sugar, refined starches, and the other foodlike substances making up the base of the Standard American Diet. The same used to be true of the Okinawans where, sadly, soda and snacks are an ever-larger part of the diet of the youth.
All of Buettner’s Blue Zones groups had in common the lack of Western “foods”. In Costa Rica, eggs were common in the diet, eaten daily along with large amounts of lard. Pork was eaten whenever it could be afforded, usually for Sunday lunch, or when a pig was killed. Most of the groups were very poor, and engaged in daily hard labour, even when old. The wealthy Loma Linda-ers were not all vegan, and it was noted that the healthier community members were those who ate fewer doughnuts and cookies.
This leads inevitably to the suspicion that what healthy people do NOT eat on their diets, traditional or self-selected, may be just as important as what they do eat. Fortunately there is an immense study, Nutrition and Degenerative Diseases, that compared and contrasted the health of peoples eating their traditional diets with groups of the same peoples – hence same genetic stock, same environmental conditions – eating Western foods, mostly white flour, white sugar, jam, condensed milk, and canned meats. The British islanders who were astoundingly healthy on fish and potatoes, the Swiss highlanders whose health and strength on rye bread and goat cheese was legendary, leading to high demand for their services as personal guards to kings and popes, the Africans thriving on millet, yams, and fish, all lost their health within two generations. Not included in this book is the case of the thriving Pima in the USA, who went,, within the same two generations, from healthy and wealthy on their corn, beans, squash, meat and fish diet, to obese and diabetic when confined to reservations and issued white flour, white sugar, jam, canned meat, canned lard…American Army rations…
The work of Robert McCarrison is particularly valuable and interesting in this light, as is Wrench’s book, The Wheel of Health.
Another factor to be considered is evolution. Traditional peoples who have coevolved with their food supply develop physical adaptations to it. For example, peoples whose ancestors have, for hundreds or thousands of years, eaten a low starch diet, have very few copies of the gene coding for salivary amylase, AMY-1, which not only starts the conversion of starch to sugar in the mouth but continues it in the small intestine, while those whose ancestors ate a high starch diet have multiple copies. The genes for lactase persistence evolved separately in Europe and Africa, and different genes are involved, giving a fortunate 30% of the world’s population the ability to drink the milk of cows, sheep, goats, horses, water buffalo, and camels.
Then there are enterotypes. Humans have three basic gut biomes, made up of specific guilds of the bacteria that do most of our digestion. Each enterotype, which irreversibly alters the gut to suit itself only shortly after the birth of a baby, works best on particular food groups. The Japanese have a gut bacterium that permits them to digest seaweed.
I think that the day will come when we are all food typed at birth just as we are currently blood typed. We owe our success as a species as much to the plasticity of our gut as to the size of our brain or our bipedal gait. Wherever we went, there were at least a few individuals who could digest the local food offerings, and that is the key to survival!
I think low carb diet should be opted for, when there is an ardent desire to loose extra pounds. Once desired weight is achieved then the regular and balanced diet should be resumed. It is unhealthy to continue with it for a longer period of time.
The problem with returning to the “regular and balanced diet” is that the pounds usually return, bringing with them a few friends, relatives, and general hangers-on…
There is no reason for a low carb diet to be unhealthy regardless of duration if the carbs are chosen to be low starch and low sugar. Many low carbers eat the greatest volume of their food as veggies and fruit.
I’ve found that I can tweak my weight up and down by 6-7lb, while keeping calories and exercise constant, simply by tweaking the starch content of my diet. At more than 30% starch, up goes my weight! My bloodwork comes back to me with “Beautiful” Keep it up!” written across it, my colonoscopy was likewise described as “Beautiful!” and the Archimedes algorithm gives me less than 3% lifetime risk of heart disease or diabetes. The low starch, low sugar, diet also minimizes the frequency and intensity of both hot flashes and migraines.
“Low carb” is not a diet, it is the natural way to eat – adapted to the needs of the particular individual. There is no regular and balanced diet.
Lex Rooker eats Zero Carbs. He has been eating only raw red meat and fat for five years, and his health, both in his personal reports and his lab records, improves year by year. He’s now 61. http://www.rawpaleodietforum.com/journals/lex%27s-journal/
Very interesting!
I keep getting this error page…
“An Error Has Occurred!
Sorry Guest, you are banned from using this forum!
This ban is not set to expire.”
Hmm, that’s weird. %27 snuck into the url, replacing the apostrophe in Lex’s, even though I copied and pasted. http://www.rawpaleodietforum.com/journals/lex's-journal/. I’ve deleted the additions and replaced the apostrophe, and will test it right away.
Isn’t this whole world of dietary continuum fascinating??
Okay, it works now. Later today I’m going to print out Lex’s results and make a graph of his health markers.
top text in this html. marry me. i eat sprouts, raw organic beef and avocado.
Ross Horne drank a beer almost daily and ate whatever his wife cooked him. He promoted 811 as the ideal although when it came to walking the walk he failed in those regards.
Bif Naked said herself she was an accidental raw vegan for almost a decade and has been fruitarian for almost 3. Just from that you can gather that she is not vegan for the health reasons and her primary motive is for ethical reasons. When she was diagnosed she said she was like an anorexic boy, that is a clear sign that she was undernourished. She is also very pale and clearly needs to get some more sun.
Harvey Milstein constantly medicated himself at a young age dropping some antibiotics at the first sign of a cold. It wasn’t until he got kidney stones for the second time that he changed his lifestyle to follow being a natural hygienist. Though he still admitted to using raw honey. He was not vegan.
There is very little to support Robin Gibb following a vegan diet. Apparently it was just one blog that mentioned this. I doubt he was high carb and he probably consumed vegan junk food. He also would have led a pretty destructive lifestyle in his younger years. According to his son he did not die from the cancer which had gone into remission and was undetectable. He suffered a kidney/liver failure which was the side effect of his chemotherapy treatment. Medical staff neglected the families wishes for how he was to be cared and made decisions which ultimately lead to a rapid decline in his health resulting in his death.
There is little on Vihara Youkta and the only information is that she was under a lot of life stresses at the time of her declined health. Out of all the examples she seems like the person that should have been the one to die this way the least.
T.C. Fry came to Natural Hygiene at the age of 45 in very poor health with a battered and bruised body. He was practically on deaths doorstep. He switched to raw Natural Hygiene overnight which resulted in a massive recovery in health and a healing of his illnesses and ailments. This is what sparked him to promote the lifestyle. He did however have occasional slips as everyone does during lifestyle transitions. Due to switching overnight this means that he went straight back to bad choices in foods that were on the complete opposite end of the spectrum of natural hygiene. Leading up to his death he was not following natural hygiene principles despite declining in health he was eating cooked foods and following other alternative treatments which were neither anything to do with natural hygiene or modern medical treatments. Joel Fuhrmen noted his vitamin B12 levels were extremely low however he only presented his opinion towards his death and this was not confirmed as cause of death. In fact about 40% of the US are in the low normal range of B12 and 6% are outright deficient. So to use this as an argument against veganism is ridiculous. Other sources note that he was low in DHA however it is clear that he was not even following the lifestyle correctly so his use in the argument is also null and void.
Almost one year. Needing some proof of aliveness.
@Wade: It can be argued, in exactly the same way, that unhealthy omnivores are not doing the diet correctly.
The weakness of the “not doing it properly argument” is its basic assumption that there is a single correct diet that is correct for everybody, and that any deviation from said diet will lead to sickness and premature death – and that will serve you jolly well right, you sinner! The wages of sin, you know…
Denise! That was sneaky. You knew some of us just can’t resist scratching our curiosity itch, I just had to click over to look at those Piccinini Hybrids. EEEW . . .
To the poor souls subscribed to comments on this site: apologies for the deluge of spam lately! I just tightened moderation, so that hopefully won’t be a problem anymore. Sorry for making y’all wade through gibberish and hyper-link-stuffed advertisements.
Blogging and updates to resume in T-minus three weeks.
Dear Denise, Please update soon like you said and update more or I’ll go to your house and molest you!!!
I think the science is clear on this. Taube gives the best presentation I’ve seen on the subject of high fat diets. See it here:
http://www.best-clickz.com/althealth/gary-taubes-what-foods-makes-you-fat
I didn’t read more than a paragraph of your blog as I got side tracked googling human animal hybrids, which has inspired me to begin an independent study looking into the diets of scientists who are interested in creating animal human hybrids. It will likely be a 15 year study but I will keep you posted as the study reaches it’s mid point.
Congratulations, Denise.
Denise, These sentences in your summary concern me: “But so far, raw veganism has had a less-than-impressive track record for longevity. The raw foodists who’ve made it into old age in good health typically included some animal products.” Are you implying that the mere 7 cancer related deaths of raw vegans you that described are enough to establish a “track record” of any kind? Or that the 2 raw foodists who consumed animal products constitute any kind of “typical”? I’m surprised and disappointed you made blanket statements like that without ample evidence/data. (In this article anyway – maybe you have other articles with the data that backs up these statements?)
debiamh, I believe those are clearly Denise’s own opinions on the matter. She didn’t imply anything she stated raw veganism has had a less-than-impressive track record for longevity, it doesn’t IMPRESS her. This is based on her opinion and analysis after sticking around raw food vegan boards for a really long time. She’s not required to produce some mythical 50-year longitudinal study for every impression she gets. She just compiled a list of the well-known raw food vegans who died early, partly I suppose to prove she knew what she was talking about… she didn’t suppress another 10 that lived until their 90s. I’m still a little suspicious after her strange turnaround in the wild and ancient fruit article where at one point she stated her readers were a specific group of people and she wouldn’t make those claims to a group of esteemed pomologists… but I think at this time it’s safe to say that from her and from lots of people… raw food vegans should not expect to live longer than raw foodists who add a little meat… if she really based it on those examples they should barely expect to live longer than people who eat SAD every day of their lives.
Hi, I read the beginning of your book, and I was wondering if you had amalgam fillings, or how you felt about them.
Love this fab blog! Exciting. I’m a lover of animals but I can’t help needing to eat meat usually grass fed. Looking forward to legit, non toxic lab generated meat that actually tastes like meat produced in an environmentally smart method.
Kraft, General Foods…carb. loaders are eventually doomed so they better get smart and jump on the bandwagon of reality by investing their ill gotten fortunes for humane and healthy food options. Sugar, gluten and starch are slow killers and these magnet producers are the demons of the world if they keep marketing their poisons especially their garbage candy laden cereals to growing children. Yes, Coke is a Joke, thank’s for that handy catchphrase Dr. Mercola.
Every time I see a school shooting or hear about kids bullying I know part of the underlining causation.
Currently loving Dr. Perlmutter’s, Grain Brain. We are catching on and it’s about time.
low carb is high fat, not high protein, that is a common misconceptions. Until the scientific studies take that into consideration all tests will be flawed. After a year of Lchf dieting my triglycerides went down and my hdl went up, my blood pressure went down and i even had my hypothyroid medication lowered. All the studies that compare low carb high fat to low fat high carb diets show that things like triglycerides and hdl fair better in lchf. High protein is the real danger, too much protein creates problems and your body will end up metabolizing it like sugar and the combo of high fat high carb is the real danger.
Denise, I have to ask:
HOW does one go about maintaining good health when there is an incredible amount of factors to consider?! I mean, if cronometer.com, or even blood tests cannot tell me if my diet is supplying me with adequate nutrients, must I pay to see a naturopath? Or is it simply necessary for me to invest an incredible amount of time for researching, as you have, in order to achieve the knowledge necessary to manage my own health?
Great post! The only thing I would say is that we have to avoid sugar at all costs! This great infograph explains the difference between “good” carbs and “bad” carbs and to tell you the truth you can be vegan, low-carber or paleo but avoiding processed sugar is crucial. http://www.lowcarbfoods.org/good-carbs-vs-bad-carbs.php
Seriously, your blog RULES. You are the dissecter-in-chief! Rock on. Rock on.
Leaving diabetes out of the picture again?
When nest to Finland has the highest incidence of type 1 diabetes IN THE WORLD:
http://www.exodiab.se/research-areas/type-1-diabetes/
Oh! and It was second, in annual consumption of milk, after Finland:
http://en.wikipedia.org/wiki/Milk
Any thoughts?
Interesting facts about Sweden. But this is too easy to find, isn´t it?
What’s actually killing Sweden is multiculturalism.
All the observational nutrition studies are problematic. All of them are vulnerable to the kind of number Denise Minger did on the China Study: as Valter Longo says in an interview, you can make them say what you want (although he does not go on to dismiss them as one of the tools in guiding dietary advice). And they all point the same way.
The LCHF and the high-starch diets agree on avoiding junk food. Beyond that, LCHF is underpinned by some interesting insights into the physiology behind it, and no real long-term data, and is informed by the more ‘mechanistic’ aspects of science (it is no accident that one supporter, Ivor Cummings, constantly uses engineering as an analogy).
By contrast, high-starch, mainly plant diets, if the observational studies are worth anything (and low-carbers think they are not, and perhaps doubt that the Japanese traditionally ate mainly rice), are associated with long healthy lives in many places.
My money is on the consensus of observational studies, although such studies can undoubtedly be discredited, one by one, by the kind of argument Denise Minger does so well. Having puzzled over the competing voices long and hard, I regard high fat diets as a ‘Big Fat Experiment’ owing to the paucity of epidemiological data.
However, if you have tried LCHF diet and feel satisfied and healthy, naturally you would want to share this success, and I wish those who are persuaded by the LCHF arguments a long life and best of health!